Health and Care Experience Survey 2015/16 - National Results
Results from the 2015/16 Health and Care Experience Survey.
This document is part of a collection
8 GP Practices - Medicines, Tests, Referrals and Mistakes
Summary
- Patients responded very positively to the questions about medications. The statements 'I knew enough about how and when to take my medicines' and 'I took my prescription as I was supposed to' received the highest positive responses in the survey. Ninety-eight per cent of respondents in agreement or strong agreement with them.
- Patients also responded positively to questions about tests arranged by their GP practice. However, they were noticeably more positive about the need and purpose of the test being explained to them (96 per cent) than they were about the results being explained in a way they could understand (81 per cent).
Medicines
8.1 Medicines are the most frequently used intervention in healthcare. In primary care, there are some 101 million prescriptions dispensed each year with an annual drugs bill of around £1.2 billion [17] (around ten per cent of the annual healthcare budget).
8.2 Policies centre on promoting a healthier Scotland, and that everyone can access the medicines they need and make choices about managing and improving their health.
8.3 Importantly, more effective medicine use can help
- deliver better care outcomes for patients
- reduce the incidence of avoidable hospital admissions and
- improve the efficiency and effectiveness of treatment.
8.4 Central to this is supporting the patient with the right level of information and advice in taking his/her medicine as prescribed by a doctor or other trained healthcare prescribers (such as a pharmacist or specialist nurse). This is an objective common to a range of healthcare professionals, including GPs and community pharmacists / chemists and aims to improve health outcomes as well as reduce waste in prescribed medicines.
8.5 Patients were asked how much they agreed or disagreed with six statements about the last time they had been prescribed medicines at their GP surgery:
- It was easy enough for me to get my medicines
- I knew enough about what my medicines were for
- I knew enough about how and when to take my medicines
- I knew enough about possible side effects of my medicines
- I would know what to do if I had any problems with my medicines
- I took my prescription as I was supposed to.
8.6 In general, patients responded very positively about medication. The four most positively answered GP questions all related to medication. Fully 98 per cent agreed or strongly agreed with the statements 'I knew enough about how and when to take my medicines' and 'I took my prescription as I was supposed to'.
8.7 However, as in the previous surveys, the side effects of medication were less well understood. Compared with the highs of 98 per cent for the questions highlighted above only 82 per cent agreed or strongly agreed that they knew enough about possible side effects. The next least positive question was knowing what to do if they had any problems with their medicine (89 per cent) (Table 4).
Table 4: Summary results of questions about medicines
| Statement | Strongly agree/agree (%) |
Neither agree nor disagree (%) |
Disagree/strongly disagree (%) |
Change since 2013/14 |
|---|---|---|---|---|
| It was easy enough for me to get my medicines | 96 | 2 | 2 | 0 |
| I knew enough about what my medicines were for | 97 | 2 | 1 | 0 |
| I knew enough about how and when to take my medicines | 98 | 1 | 1 | 0 |
| I knew enough about the possible side effects of my medicines | 82 | 12 | 6 | 0 |
| I would know what to do if I had any problems with my medicines | 89 | 7 | 4 | -1 |
| I took my prescription as I was supposed to | 98 | 1 | 1 | 0 |
GP Practices - Tests arranged by the practice
8.8 In response to a significant number of freetext comments relating to blood tests, x-rays and other tests arranged by GP practices new questions were added to the 2013/14 survey to explore patients' experiences of such tests - a common feature of primary care.
- 71 per cent of respondents had had a test arranged in the past 12 months
8.9 Those that had were asked whether they agreed with four statements:
- It was explained to me why a test was needed
- I was satisfied with the length of time that I waited for my test results
- I was satisfied with the way that I received the result
- The results of the test were explained to me in a way I could understand
8.10 The most positive result was that 96 per cent of patients agreed or strongly agreed that it had been explained to them why a test was needed. This was also the only question of the four that did not get worse from the previous survey.
8.11 Responses for the other questions were noticeably less positive. 80 per cent agreed or strongly agreed that they were satisfied with the way that they received the result and 81 per cent felt that the test were explained in way that they could understand. These are both modest drops from the previous survey (Table 5).
8.12 This discrepancy may in part stem from how the different information is communicated. The initial need for a test is likely to be explained in a face to face consultation with a doctor or nurse, whereas results may well be provided over the phone and/or by a non-health professional.
Table 5: Summary results of questions about tests
| Statement | Strongly agree/agree (%) |
Neither agree nor disagree (%) |
Disagree/strongly disagree (%) |
Change since 2013/14 |
|---|---|---|---|---|
| It was explained to me why a test was needed | 96 | 3 | 1 | 0 |
| I was satisfied with the length of time I waited for my results | 85 | 8 | 7 | -1 |
| I was satisfied with the way I received my results | 80 | 10 | 10 | -1 |
| The results of the test were explained to me in a way I could understand | 81 | 11 | 8 | -1 |
GP Practice - referrals to another professional
8.13 General Practitioners have a role as the gateway to secondary care. The referral process is therefore an important component of quality care, which requires coordination and communication between different health and care services. Problems with referrals can lead to poor continuity of care and delayed treatment.
- 54 per cent of patients had been referred to other health or care services and a further one per cent felt that they should have been referred to services, but were not.
8.14 Respondents who had been referred were asked how they would rate the arrangements for getting to see other health or care services.
- 77 per cent of patients who were referred by their GP in the last twelve months rated the referral arrangements as excellent or good;
- 15 per cent rated the arrangements as fair;
- eight per cent rate the arrangements as poor or very poor
8.15 These results are slightly less positive than the previous survey, but have remained broadly similar over the last three surveys (Figure 13).
Figure 13: Positive rating of referral arrangements (%)
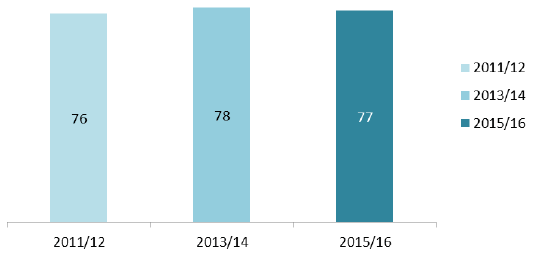
Mistakes
8.16 In line with the healthcare quality strategy outcome for NHS Scotland that ' Healthcare is safe for every person, every time'. questions regarding mistakes were introduced to the 2013/14 survey in order to provide an insight into the incidence of mistakes as well as patients' experiences of how mistakes were dealt with.
8.17 Respondents were asked whether they believed a mistake was made in their treatment or care by their GP practice.
- seven per cent of respondents believed such a mistake had been made in their treatment or care, a modest increase from the previous survey (six per cent).
8.18 Of those that felt a mistake had been made in their treatment or care:
- 46 per cent were satisfied with how it had been dealt with overall
- 54 per cent were not satisfied
8.19 These are the least positive GP results in the survey. It is worth noting however, that they only apply to the seven per cent of respondents who believe that they experienced a mistake.
8.20 The results would suggest that mistakes, where they do occur, are not consistently dealt with to patients' satisfaction. It is not possible to establish the seriousness of the mistakes that patients are referring to when answering these questions. The survey question itself provided examples of mistakes as occurring in 'test results, medicines prescribed [and] diagnosis'.
Contact
There is a problem
Thanks for your feedback