Health and care experience survey 2017 to 2018: national results
Results from survey asking about people’s experiences of GP practices and other local healthcare services.
This document is part of a collection
8. Out of Hours Care
Summary
- In the last year, 45 per cent of people got advice or treatment from an Out of Hours (OOH) service. The most common service people ended up receiving treatment or advice from was pharmacists / chemists.
- People were most positive about experiences of person-centred behaviours around understanding the information they were given and being listened to. People were least positive about having the opportunity to involve the people that mattered to them.
- Most people (83 per cent) rated the overall care they had experienced from the service they ended up receiving treatment or advice from positively.
Introduction
Many people contact the NHS in a way that is unplanned, for example if they become ill during the day or night, or at the weekend. It is crucial that the NHS responds in a way that meets the needs of the patient in a timely, person-centred, safe and clinically appropriate way. Often the journey of care will involve more than one part of the healthcare system so it is important for systems and process to be joined up.
While many of these unplanned contacts will involve a patient's GP practice, NHS boards have a legal responsibility to ensure the services provided by GP practices are provided at all times, including OOH services [23] . OOH services include NHS 24, emergency services and pharmacies and can often be accessed by individuals at any time, whether their GP practice is open or closed.
A National Review of Primary Care Out of Hours Services was undertaken in 2015. The resulting report [24] contained a number of recommendations, including a focus on ensuring that primary care out of hours services:
- are person-centred, sustainable, high quality, safe and effective;
- provide access to relevant urgent care when needed; and
- deliver the right skill mix of professional support for patients during the OOH period.
Use of OOH Services
Forty five per cent of people had tried to get treatment or advice from a pharmacy, NHS 24 or an emergency service in the last 12 months. This is a much higher proportion than had been reported as using OOH services in previous surveys (27 per cent in both 2015/16 and 2013/14) as the wording of the question has been revised to be clearer about which services it is asking about and to incorporate those who had used an OOH service when their GP practice was open. This means the results will not be comparable with those from previous surveys.
Respondents were asked to specify which service they had ended up being treated or advised by the last time they used an OOH service. Figure 8.1 shows that the most common services that people ended up being treated or advised by were pharmacists/chemists (28 per cent), their own GP practice when it was open (20 per cent) and phone advice only from NHS 24 (19 per cent).
Figure 8.1: Which service did you end up being treated or advised by?
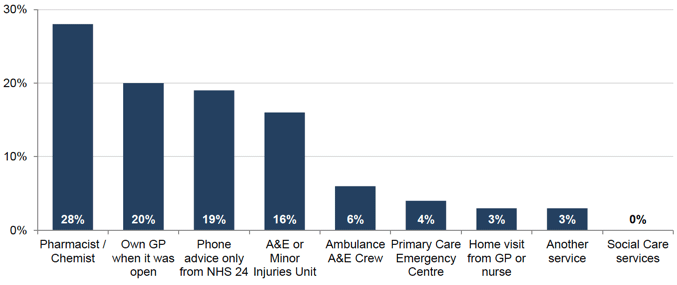
The proportion of people ending up receiving treatment / advice from a pharmacist or chemist and their own GP practice has been much lower in previous years (three and five per cent respectively in 2015/16). Conversely, the proportion of people ending up receiving treatment / advice from A&E or a Minor Injuries Unit and from Primary Care Emergency Centres has been much higher in previous years (35 and 17 per cent respectively in 2015/16). These changes are most likely due to reframing the OOH questions in the 2017/18 survey, rather than a real change in advice provision.
Half of those who had used an OOH service did not try to contact their GP practice first (51 per cent), see Figure 8.2. The proportion of people who did not try to contact their GP practice first was highest for those who had ended up being treated / advised by a pharmacist / chemist, an ambulance A&E crew or at A&E / a Minor Injuries Unit (74, 66 and 63 per cent respectively). It was lowest for those who ended up being treated / advised by their own GP practice when it was open (8 per cent).
Figure 8.2: Contact with GP practice before contacting an OOH service
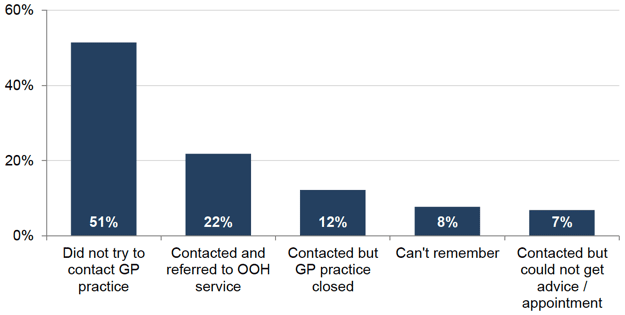
Fifty eight per cent of both those who ended up being treated / advised by their own GP practice when it was open and those who received a home visit had contacted their GP practice first and had been referred. This was noticeably higher than the national figure for those who had contacted their GP practice first and had been referred (22 per cent).
Seven in ten people had received treatment or advice for a physical health problem – 17 per cent for an injury or accident and 52 per cent for another type of physical health problem. Only three per cent of people had received treatment or advice from an OOH service for a mental health problem.
Person-centred Care
The survey asked respondents whether they agreed or disagreed with seven statements relating to person-centred behaviours they experienced the last time they used an OOH service, mirroring those asked about experiences at the GP practice. People were generally positive about their experience of an OOH service.
The most positively rated statements were 'I understood the information I was given' and 'I was listened to' (93 and 92 per cent positive respectively), see Figure 8.3. This is consistent with the most positively rated person-centred statements asked about the GP practice. The statement with the lowest positive rating was 'I was given the opportunity to involve the people that matter to me' (63 per cent). However, it should be noted that this statement also had the largest neutral response ('Neither agree nor disagree') and the proportion of people rating the statement negatively was still relatively low (5 per cent).
Responses varied depending on the service that individuals had ended up receiving treatment or advice from. Looking across all the statements, those who had a home visit were the most positive, with the per cent positive responses higher than the national figure for six out of the seven statements. People who ended up receiving treatment or advice from social care services or by phone from NHS 24 were the least positive, with the per cent positive responses higher than the national figure for only one out of the seven statements for both services.
Figure 8.3: Summary of responses to person-centred statements
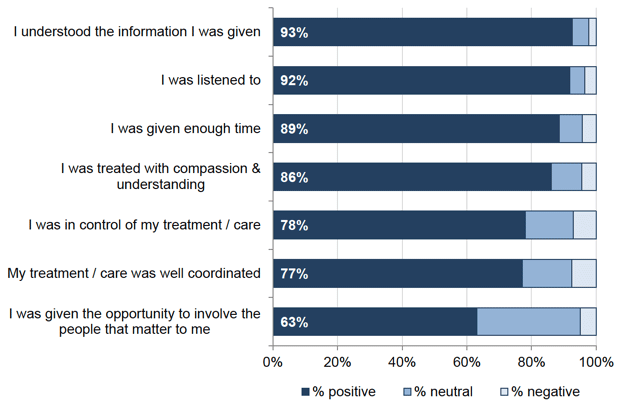
Overall Experience of Care
Most people (83 per cent) rated the overall care they had experienced from the service they ended up receiving treatment or advice from positively. This shows a notable increase from the proportion of people rating the care they experienced from OOH services positively in previous years (70 per cent in both 2015/16 and 2013/14). This is likely due to the reframing of the questions in this section rather than a real improvement in experiences.
Figure 8.4 shows how people had rated their care by the service they had used. Pharmacists / chemists, ambulance A&E crews and home visits all had the highest proportions of positive ratings (89, 89 and 88 per cent respectively). Social care services had highest proportion of negative ratings (15 per cent) however only a very small number of people had used this service.
Figure 8.4: Overall rating of care experienced by service
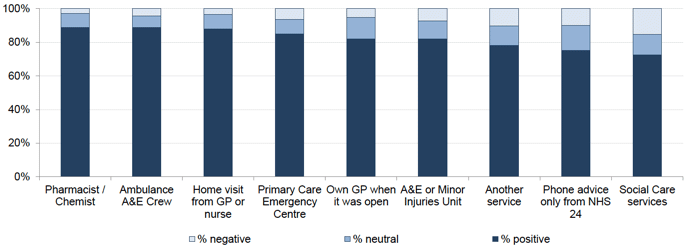
Contact
There is a problem
Thanks for your feedback