Scottish Health Survey 2015 - volume 1: main report
Findings and trends of the Scottish Health Survey 2015, providing information on the health of people living in Scotland.
This document is part of a collection
2 General Health And Multiple Conditions
Linsay Gray and Alastair H Leyland
Summary
- In 2015, around three-quarters (74%) of men and women aged 16 and over described their health as 'very good' or 'good'. There has been little change in this level since 2008.
- The proportion of adults reporting to be in 'very good' or 'good' health declined with age from 88% of those aged 16-24 to 55% of those aged 75 and over.
- Nearly all (95%) of children were reported to be in 'very good' or 'good' health.
- General health was broadly similar for boys and girls, with 65% of boys and 67% of girls having 'very good' reported general health.
- Levels of 'very good' health ranged between 65% and 73% for those aged 0‑11 but declined from 63% for those aged 12-13 to 52% for those aged 14‑15.
- Half (50%) of adults had at least one long-term condition in 2012-2015. These were split equally between 25% with only one condition and 25% with more than one condition.
- Older adults were more likely than younger adults to have multiple long-term conditions, with 59% of those aged 75 and over having at least two conditions compared with 6% of those aged 16-24.
- Age-specific patterns of long-term conditions prevalence were similar for men and women, although, among those aged 16-24, men (81%) were more likely than women (72%) to have no long-term conditions. Just under a fifth (18%) of those in the least deprived areas had multiple conditions compared to around a third (34%) of those living in the most deprived areas.
- In 2012-2015, 9% of adults had both a physical health condition and symptoms of mental disorder.
- Adults with one or more physical condition were twice as likely to exhibit symptoms of a mental disorder compared with those with no physical conditions (22% and 11%, respectively).
- In the most deprived areas, 29% of those with a physical condition also had a possible mental disorder, compared with 14% in the least deprived areas.
2.1 Introduction
This chapter covers two interrelated topics: self-assessed general health, and co-morbidity of multiple long-term conditions.
Population measures of self-reported health can be a general indicator of the burden of disease on society. They can reflect subjective experiences of both diagnosed and undiagnosed illnesses, and their severity, which more objective measures for the whole population can sometimes overlook.
Self-assessed general health is often a reflection on the presence or absence of long-term conditions, both physical and mental. Such conditions account for 80% of all GP consultations and for 60% of all deaths in Scotland. People with a long-term condition are twice as likely as those without to be admitted to hospital and stay in hospital disproportionately longer [2] . Older people are more likely to have multiple long-term conditions. Given Scotland's ageing population (in 2014, 8% of the population were 75 and over; this is predicted to rise to 14% by 2039), this has become an increasingly important public health issue [1] .
Mental health problems can often impact on the ability of individuals to manage their own physical health. The co-morbidity of mental health and physical health problems is now recognised as being a particularly important public health issue, whereas historically the two were treated separately [4] . There is a critical interdependence on outcomes.The associations with deprivation, lifestyle factors and wider health determinants are also of importance in Scotland given its persistent health inequalities [1] . Long-term conditions therefore represent personal, social and economic costs both to individuals and their families as well as to health and care services and Scottish society more widely.
2.1.1 Policy background
In recognition of the challenges posed by long-term conditions, the Scottish Government's National Action Plan for long-term conditions [1] was published in 2009. This defined long-term conditions as 'health conditions that last a year or longer, impact on a person's life, and may require ongoing care and support'. Conditions include mental health problems and a wide range of physical conditions such as chronic pain, arthritis and inflammatory bowel disease. Delivering on a commitment made in the earlier Better Health, Better Care: Action Plan, the National Action Plan recognised the need for system-wide action in response to the challenge presented by the increasing prevalence of long-term conditions within the context of an ageing population, the links to health inequalities, and the particular challenges of multi-morbidity.
One of the Scottish Government's National Outcomes is the overall strategic objective for health: We live longer, healthier lives [5] . This is supported by a number of National Indicators including 'improve self-assessed general health' [5] . Data from the Scottish Health Survey ( SHeS) is used to monitor progress towards this indicator. In addition, the purpose target to improve healthy life expectancy over the 2007 to 2017 period uses Scottish Health Survey ( SHeS) data for children (aged 0-15) in the calculations used to measure progress.
2.1.2 Reporting on general health and multiple conditions in the Scottish Health Survey
This chapter reports on self-assessed general health by age and sex of adults in 2015 and children in 2014/2015. Analysis is presented for the prevalence of multiple long-term conditions, by age and sex, and by area deprivation for the years 2012-2015 combined. The combination of the presence of common mental disorders as measured by the GHQ12 scale, and physical long-term conditions is also reported for the same time periods and demographics.
2.2 Methods and definitions
2.2.1 Self-assessed general health
Each year, participants aged 13 and over are asked to rate their health in general with answer options ranging from 'very good' to 'very bad'. For children under the age of 13 the question is answered by the parent or guardian completing the interview on their behalf. This question is used to monitor the National Indicator 'improve self-assessed health', while the data for children (aged 0-15) is used in the calculation of healthy life expectancy used to monitor the related purpose target.
2.2.2 Multiple long-term conditions
All participants were asked if they had any physical or mental health condition or illness lasting - or likely to last - for twelve months or more. Those who reported having such a condition were asked to provide details of the type(s) of conditions or illnesses reported. Answers were recorded verbatim and then coded by an analyst. These questions did not specify that conditions had to be doctor-diagnosed; responses were thus based on individuals' perceptions.
At a later stage of the interview, participants were asked about a number of specific health conditions, including diabetes and hypertension. If the participant mentioned that they had doctor-diagnosed diabetes or that they had doctor-diagnosed hypertension in response to these questions, but they had not mentioned them as a long-term condition, they were each counted as such a condition.
The number of long-term conditions a person had was thus calculated based on the sum of different conditions reported in response to the long-term conditions questions, and any additional diabetes and / or hypertension doctor diagnoses. This definition differs from those used in previous years; as a result comparisons should not be made with previously published long-term condition figures.
Conditions were considered different if they came under mutually exclusive chapters in the International Classification of Diseases (ICD-10) [6] (15 in total, using chapters I to XIV, plus an "other"). The exceptions to this were with respect to chapter IV, in which diabetes and other endocrine and metabolic illnesses were counted separately, and chapter IX, in which stroke, angina, hypertension, other heart problems, and other circulatory system problems were all counted separately. Thus, up to 20 different conditions were counted:
- Certain infectious and parasitic diseases
- Neoplasms
- Diseases of the blood and blood-forming organs and certain disorders involving the immune mechanism
- Endocrine, nutritional and metabolic
- Diabetes
- Other endocrine and metabolic illnesses
- Mental and behavioural disorders
- Diseases of the nervous system
- Diseases of the eye and adnexa
- Diseases of the ear and mastoid process
- Diseases of the circulatory system
- Stroke
- Angina
- Hypertension
- Other heart problems
- Other circulatory system problems
- Diseases of the respiratory system
- Diseases of the digestive system
- Diseases of the skin and subcutaneous tissue
- Diseases of the musculoskeletal system and connective tissue
- Diseases of the genitourinary system
- Other long-term conditions
The number of conditions a person had that were specifically physical were counted in the same way, but with conditions coded under chapter V of the ICD (mental and behavioural disorders) excluded.
This definition of multiple conditions was created following a comprehensive review of co-morbidity using SHeS data [7] and will be re-examined on an on-going basis.
2.2.3 Symptoms of Mental Disorder (GHQ-12)
GHQ-12 is a widely used screening tool for common mental disorders. It consists of 12 questions on concentration abilities, sleeping patterns, self-esteem, stress, despair, depression, and confidence in the previous few weeks. Responses to each of the GHQ-12 items are scored, with one point allocated each time a particular feeling or type of behaviour is reported to have been experienced 'more than usual' or 'much more than usual' over the previous few weeks. These scores are combined to create an overall score of between zero and twelve. A score of four or more (referred to as a high GHQ-12 score) has been used here to indicate the presence of a possible mental disorder. A score of zero on the GHQ-12 questionnaire can, in contrast, be considered to be an indicator of psychological wellbeing. GHQ-12 measures deviations from people's usual functioning in the previous few weeks and therefore cannot be used to detect chronic conditions.
2.3 Self-Assessed General Health
2.3.1 Self-assessed general health among adults in 2015, by age and sex
In 2015, around one third (34%) of those aged 16 and over reported their general health as 'very good', with 40% saying it was 'good' and 18% as 'fair'. A further 6% assessed their health as 'bad' and 2% as 'very bad'. The proportion (74%) of adults who stated their health was either 'very good' or 'good' was similar to figures reported in each survey year since 2008 (74-77%) [8] . Men and women's assessments of their own health were almost identical.
The significant variations in self-assessed health by age were similar to those reported for previous years of the survey [8] . Figure 2A and Table 2.1 show that the proportion of adults reporting to be generally in 'good' or 'very good' health declined as age increased (from 88% of those aged 16-24, to 55% of those aged 75 and over). Correspondingly, self-reported 'bad' or 'very bad' health was more prevalent among older age groups (ranging from 1% of adults aged 16-24 to 13% of those aged 65 and over). A similar age-related variation in self-assessed general health was seen for both sexes.
Figure 2A, Table 2.1
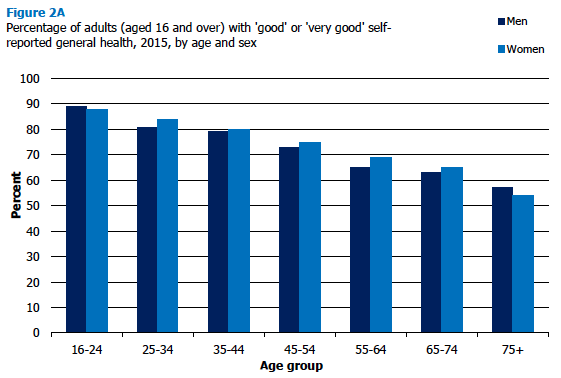
2.3.2 Self-assessed general health among children in 2014/2015 (combined), by age and sex
In 2014/2015, nearly all (95%) children aged 15 and under in Scotland were reported to be in 'good' or 'very good' health. Two thirds (66%) had general health which was considered to be 'very good', 29% 'good' and 4% 'fair'. General health was 'bad' or 'very bad' for just 1% of children. Figures on general health for boys and girls were largely similar, with 65% of boys and 67% of girls stated to have 'very good' general health and a further 29% of both sexes having 'good' general health.
Levels of 'very good' health were generally similar from age 0-1 to 10‑11 (between 65% and 73%) but had a significant drop between the ages of 12-13 and 14-15 (from 63% to 52%). This may in part reflect differences in the way parents report their child's health (for those aged 0-12), and the way children (aged 13-15) report their own health.
The decline in 'very good' health as children aged was steeper for girls than boys. Around three quarters (76%) of girls aged 0-1 were described as being in 'very good' health in general with this declining to 47% of those aged 14-15. A shallower decline was seen for boys, from 70% of those aged 0-1 to 56% of those aged 14-15.
2.4 Multiple long-term conditions in adults
2.4.1 Prevalence of multiple conditions in 2012-2015 (combined), by age and sex
In 2012-2015, half (50%) of adults aged 16 and over in Scotland had at least one long-term condition, as shown in Table 2.3, with a quarter (25%) having one condition and the remaining quarter (25%) reporting multiple (two or more) conditions. Five percent of adults had four or more long-term conditions. The mean number of long-term conditions did not differ significantly according to sex.
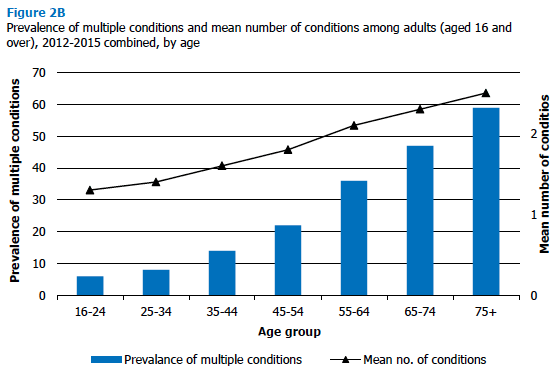
Being free of long-term conditions in 2012-2015 was markedly less common among older age groups than younger ones, with 14% of adults aged 75 and over reporting having no conditions compared with 77% of those aged 16-24. A higher proportion of those aged 55 and over (28-30%) had one condition than those aged 16-24 (18%), with older age groups also being significantly more likely than others to have multiple conditions. Those aged 75 and over were around ten times more likely than those aged 16-24 to report having two or more conditions (59% compared with 6%).
Age-specific patterns of long-term conditions prevalence were similar for men and women, with the exception of those aged 16-24, where men (81%) were more likely than women (72%) to have no long-term conditions.
The mean number of long-term conditions in 2012-2015 was similar for men (1.9) and women (2.0). The mean number of conditions for those aged 75 and over (2.5 conditions for both men and women) was around double that for those aged 16-34 (means of 1.2-1.3 conditions for men and 1.4 conditions for women).
Figure 2B, Table 2.3
2.4.2 Prevalence of multiple conditions in 2012-2015 combined, by area deprivation
Just under a fifth (18%) of those in the least deprived quintile had multiple (two or more) conditions compared to around a third (34%) of those living in the most deprived quintile, using age-standardised data. Patterns by deprivation were largely similar for men and women.
There was a significant association between the age-standardised mean number of long-term conditions and area deprivation. Adults living in the least deprived areas of Scotland had a mean of 1.7 long-term conditions compared with 2.2 conditions for those living in the most deprived areas. There was little difference by sex, with both men (1.7) and women (1.8) in the least deprived areas having a lower mean number of conditions than those in the most deprived areas (2.1 and 2.2, respectively).
2.5 Symptoms of Mental Disorder ( GHQ12) by prevalence of physical conditions in adults
2.5.1 Symptoms of mental disorder ( GHQ12) by prevalence of physical conditions and sex in 2012-2015 combined
Two in five adults (42%) in 2012-2015 had at least one long-term physical condition, while one in six (15%) showed symptoms of a mental disorder (scoring 4 or more on the GHQ12 scale). Just under one in ten adults (9%) had both a long-term physical condition and showed symptoms of a mental disorder.
Table 2A Symptoms of distress (using GHQ12) and presence of physical conditions, 2012-2015 combined
| |
Number of physical conditions | Total |
|
| |
None | One or more | |
| GHQ12 score | % | % | % |
| 0 | 38 | 23 | 61 |
| 1-3 | 13 | 11 | 24 |
| 4 or more | 7 | 9 | 15 |
| Total | 58 | 42 | 100 |
Table 2.5 shows age-standardised GHQ12 scores by presence of physical conditions for adults aged 16 and over in 2012-2015. Just over a fifth (22%) of adults with one or more physical condition had a GHQ12 score of 4 or more compared with 11% for those with no physical conditions. Conversely, 68% of adults with no physical conditions had a GHQ12 score of zero, compared with 52% of those with one or more conditions. Patterns for men and women were largely similar.
2.5.2 Symptoms of mental disorder ( GHQ12) by prevalence of physical conditions by area deprivation in 2012-2015 combined
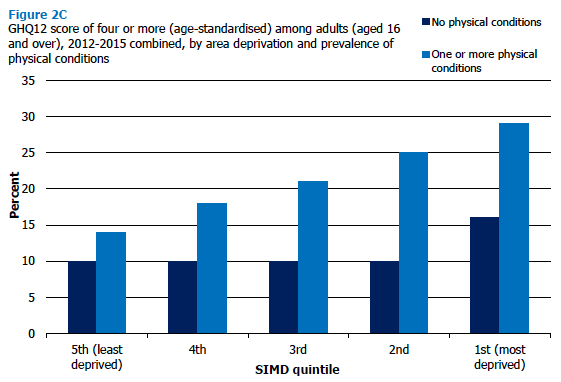
Symptoms of mental disorder (indicated by age-standardised GHQ12 scores) by number of physical conditions are shown by area deprivation for those aged 16 and over in 2012-2015 in Figure 2C and Table 2.6.
The association between symptoms of mental disorder and area deprivation differed significantly according to physical symptom status. Among those with no physical conditions, presence of symptoms of a mental disorder did not vary greatly across the deprivation quintiles. In contrast, among those with one or more physical conditions, the proportion with symptoms of a mental disorder increased with deprivation, with those in the most deprived areas in Scotland being around twice as likely as those in the least deprived areas to have a GHQ12 score of 4 or more (29% and 14%, respectively).
Figure 2C, Table 2.6
Contact
Email: Julie Landsberg, julie.landsberg@gov.scot
There is a problem
Thanks for your feedback