Scottish Inpatient Experience Survey 2016 Volume 1: National Results
Report detailing the results from the Scottish Inpatient Experience Survey 2016.
This document is part of a collection
Results - Staff
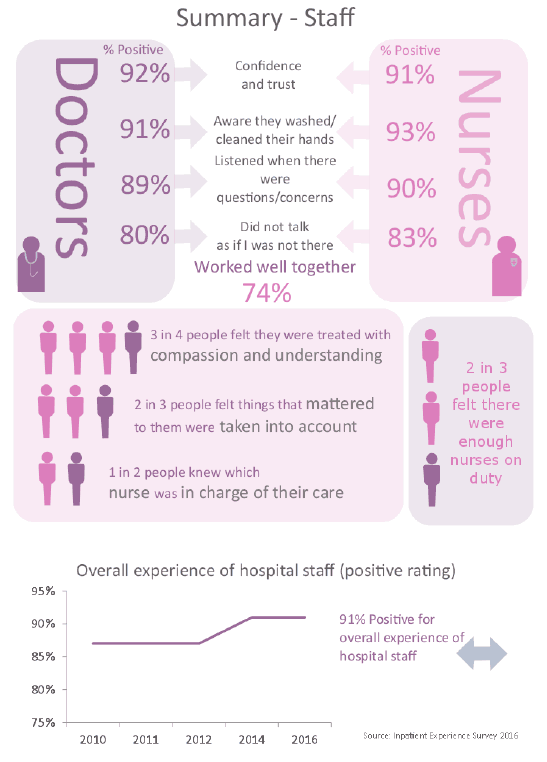
Summary
Overall people were largely positive about their experiences of hospital staff. With all staff related questions results either showing similar results to the previous survey in 2014 or the positive rating increasing slightly.
The overall rating for staff patients came into contact with was mainly positive, over nine out of ten people ( 91 per cent) rated staff as 'excellent' or 'good'.
Results also suggested that more could be done to improve some areas of communication, particularly with doctors. One in ten people ( ten per cent) reporting that doctors had talked in front of them as if they were not there.
Overall rating of staff
People were asked to provide an overall rating of the staff they came into contact with, nine out of ten ( 91 per cent) rating the staff positively (Figure 22 and 23).
Figure 22 Overall, how would you rate all the staff you came into contact with? (%)
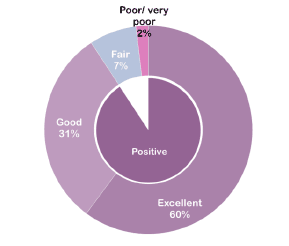
Figure 23 Overall, how would you rate all the staff you came into contact with? (%)
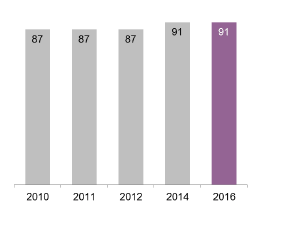
Support and compassion questions
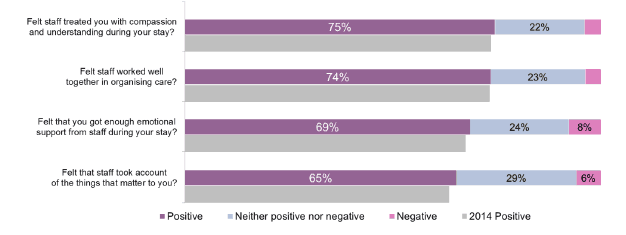
People were asked how well patients' care was organised and whether staff took account of the things that matter to patients, emotional support, and compassion and understanding (Figure 24):
- three out of four people ( 75 per cent) said that staff had 'always' treated them with compassion and understanding
- three out of four ( 74 per cent) indicated that staff had 'definitely' worked well together in organising their care
People were less positive about whether staff had taken into account the things that mattered to them and about emotional support (Figure 24):
- around two thirds ( 65 per cent) indicated that staff had ' definitely' taken account of the things that mattered to them, a rise of one percentage points from 2014
- similar proportion ( 69 per cent) indicated that they 'always' received emotional support from staff
These questions use a response scale different from most of the questions mentioned previously in the report, which may have had an effect on the way people responded, lowering the response rate to the positive option and increasing the percentage of options 'to some extent' or 'sometimes', which would typically be considered as neutral.
Figure 24 Summary of general staff questions (%)
Doctors
People were asked how much they agreed or disagreed with six statements about doctors (Figure 25).
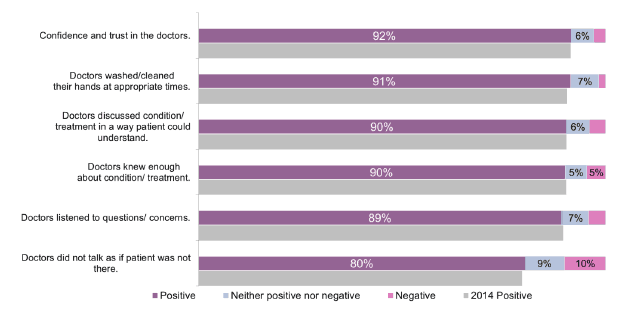
The percentage of people answering positively ranged from 80 per cent (' Doctors did not talk in front of me as if I was not there) to 92 per cent ('I had confidence and trust in the doctors treating me').
Figure 25 Summary of doctor-specific questions (%)
Nurses
People were asked how much they agreed or disagreed with six statements about nurses (Figure 26).
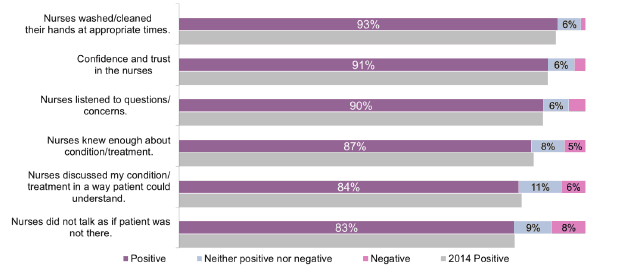
The percentage of people responding positively ranged from 83 per cent (' Nurses didn't talk in front of me as if I was not there') to 93 per cent (' As far as I was aware nurses washed/cleaned their hands at appropriate times').
Releasing Time to Care [ 18]
The Releasing Time to Care ( RTC) Programme was offered to all NHS Boards in April 2009 and its final report [ 19] recommended that all fifteen boards adopted the recommendations for sustainability and spread. One of the aims of the programme is to increase the proportion of time nursing staff spend on direct patient care. People were positive ( 90 per cent) about nurses listening to them if they had any concerns or questions.
Figure 26 Summary of nurse-specific questions (%)
Hand washing
The practice of staff routinely washing and cleaning hands after contact with patients is essential to control the spread of infection within hospitals. As part of the National Hand Hygiene campaign NHS boards undertook bi-monthly audits of hand hygiene between 2007 and September 2013. From 1 st October 2013 individual NHS Boards have been responsible for monitoring and reporting of compliance data [ 20].
The results of the survey show that patients thought that nurses and doctors washed their hands at appropriate times; only one and two per cent of patients disagreed that nurses and doctors respectively washed their hands which are similar results to 2014.
Nurses in charge of care
People were asked if they knew who was in charge of their care (Figure 27):
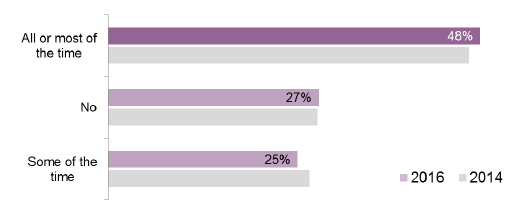
- nearly half ( 48 per cent) indicated that they knew 'all or most of the time' which nurse was in charge of their care, a rise of one percentage points from 2014
- 25 per cent indicated they knew 'some of the time'
- the remaining 27 per cent indicated they didn't know who was in charge of their care
There was considerable variation seen across the NHS Boards around knowing which nurse was in charge of patient's care, with positive results ranging from 35 to 74 per cent. Improvements were seen across many Boards but were particularly high in several.
Of those people who did not know which nurse was in charge of their care, 35 per cent would have liked to know and 65 per cent were not bothered.
Compared to results for knowing which nurse was in charge of the ward (reported in Hospital and Ward Environment section), it seems that people are more able to identify which nurse was in charge of their care rather than the ward (48 per cent of people indicated they knew 'all or most of the time' which nurse was in charge of their care compared to 43 per cent for in charge of the ward).
Figure 27 Summary of whether patients knew which nurse was in charge their care (%)
Adequate nurses on duty
People were asked whether they thought there were enough nurses on duty during their stay in hospital (Figure 28):
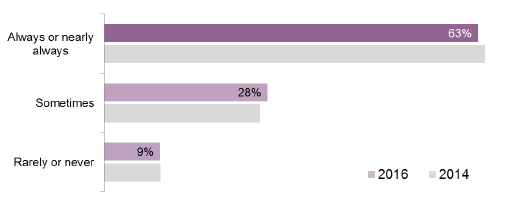
- nearly two thirds ( 63 per cent) thought there were 'always or nearly always' enough nurses on duty to care for them in hospital
- 28 per cent thought there were 'sometimes'
- nine per cent said 'rarely or never'
Figure 28 Summary of whether patients felt there were enough nurses on duty to care for them in hospital (%)
There was considerable variation between NHS Boards for this question, with positive results ranging from 52 to 92 per cent.
Further analysis was undertaken to assess how peoples' responses to the question about adequate nurses on duty correlated with their responses to the following questions about staff and care and treatment:
- Overall, how would you rate your care and treatment during your stay in hospital?
- Nurses knew enough about my condition and treatment.
- Nurses discussed my condition and treatment with me in a way I could understand.
- Nurses talked in front of me as if I was not there.
- Nurses listened to me if I had any questions or concerns.
- I had confidence and trust in the nurses treating me.
- Did you feel that you got enough emotional support from staff during your stay?
- Did you feel that staff treated you with compassion and understanding during your stay?
The results of this analysis are presented in Table 6 and show that those who answered positively about there being enough nurses on duty were more likely to answer positively about other aspects of care and treatment and staff.
The differences can be seen across all the questions we compared but are particularly noticeable in those relating to person-centred care: 84 per cent of the people who thought there were 'always or nearly always' enough nurses on duty indicated that they were 'always' given enough emotional support compared to 50 per cent of the people who thought that there were only 'sometimes' enough nurses on duty.
Similarly, 88 per cent of people who thought there were 'always or nearly always' enough staff on duty indicated that they were always treated with compassion and understanding compared to 60 per cent of those who thought that there were only 'sometimes' enough nurses on duty.
Although these differences are pronounced, there may well have been other factors influencing these results beyond simply the level of nurses on duty. A fuller variations analysis will help establish whether these differences in experience are a genuine result of the number of nurses on duty or not.
Table 6 Care rating by level of nurses on duty(%)
| Positive answers (per cent) | |||
|---|---|---|---|
| Question | There were always or nearly always enough nurses | There were sometimes enough nurses | There were rarely or never enough nurses |
| Overall, how would you rate your care and treatment during your stay in hospital? | 97 | 86 | 56 |
| Nurses knew enough about my condition and treatment. | 95 | 81 | 56 |
| Nurses discussed my condition and treatment with me in a way I could understand. | 92 | 78 | 53 |
| Nurses talked in front of me as if I was not there. | 89 | 78 | 58 |
| Nurses listened to me if I had any questions or concerns. | 96 | 86 | 62 |
| I had confidence and trust in the nurses treating me. | 97 | 87 | 61 |
| Did you feel that you got enough emotional support from staff during your stay? | 84 | 50 | 26 |
| Did you feel that staff treated you with compassion and understanding during your stay? | 88 | 60 | 34 |
Note: Due to the absence of certain sampling strata amongst respondents selecting the last option (rarely/never enough nurses on duty), the percentages for this option are not directly comparable with those for the other two options (always/nearly always and sometimes enough nurses on duty).
Contact
Email: Nicola Kerr, nicola.kerr2@gov.scot
There is a problem
Thanks for your feedback