Understanding the patterns of use, motives, and harms of new psychoactive substances in Scotland
This report presents the results of mixed methods research on new psychoactive substance use.
5. Consequences of Use
5.1 Introduction
The consequences of NPS use were reported in the NPS survey and in interviews, as well as being described by staff through the staff survey and focus groups.
5.2 Positive Effects
Given that pleasure was reported as one of the motivators for use it is important to understand the positive effects of use as reported by NPS users. Positive effects were noted across all key NPS groups, although there were specific effects associated with different types of NPS.
5.2.1 Stimulant-type NPS and mephedrone
23 people reported on the health effects of stimulant-type NPS and mephedrone, which shared the same positive effects:
- 9 respondents reported that they made them more alert
- 8 respondents reported that they gave them more energy
- 6 respondents reported an improvement in mood
Around half of people who have taken stimulant-type NPS or mephedrone (48%, n=11) stated that they continued to take these substances because they liked taking them, suggesting that the effects of alertness and energy were experienced as positive.
5.2.2 Benzodiazepine-type NPS
Fifty-eight respondents reported on the health effects of benzodiazepine-type NPS. Of these:
- 47 respondents (81%) felt their use reduced their anxiety
- 40 respondents (69%) felt that use made them more relaxed
- 22 respondents (38%) associated their use with improvements in mood
This reflects the views reported in the previous chapter about health related motivations for starting and continuing benzodiazepine-type NPS.
5.2.3 Synthetic cannabinoids
31 respondents reported on the physical health effects of synthetic cannabinoid use. A key positive effect noted by one quarter (26%, n=8) of those who had taken synthetic cannabinoids was sleep promotion. This was also described in the interviews:
Interviewer: And what would you say you enjoyed about it the first time you used it [Bombay Blue - synthetic cannabinoid]?
"The sleeping. I loved it."
Interviewer: And is sleeping difficult for you?
"Yes. I don't sleep very good." [100]
However, the sleep-promoting effects of synthetic cannabinoids were not always experienced as unequivocally positive. This is discussed in more detail in the section below. Around one fifth (21%, n=7) reported that use made them more relaxed.
5.3 Negative Effects
Negative effects were identified by interviewees in relation to intoxication and 'comedowns' and by NPS and staff survey respondents in relation to mental health, physical health, social and relationship effects. These are discussed below.
Intoxication Effects and 'Comedowns'
Interviewees in the qualitative interviews sometimes described positive intoxication effects of NPS use, however they were frequently understood to have negative effects subsequent to use. These two phases of intoxication - positive and then negative - were integrated experiences for some:
" MCAT [mephedrone] - at the time I felt banging - the next day I felt like a total junkie. The come down off it was a fucking horrible, man - horrible. It was the worst comedown I've ever had in my life.... I felt so disgusting." [101]
In addition, unwelcome intoxication effects were noted by interviewees, particularly, but not exclusively, in relation to synthetic cannabinoids. These included nausea (" I spewed everywhere [after taking a synthetic cannabinoid]") [102] in one case loss of bladder control ( "A pished myself [after taking 'Burst' - ethylphenidate]") [103] and general feelings of being unwell ( "I actually thought I was going to die on that thing [Sensate - a synthetic cannabinoid]") [104] .
5.4 Mental Health Harms
Staff and those who reported using NPS often differed in their views on the mental health effects of NPS in both the quantitative and qualitative elements of this study.
When asked in the survey about the effects of taking NPS on their mental health, small numbers of respondents across all groups reported positive effects as a result of use, however larger numbers reported negative mental health effects, in particular anxiety and paranoia, mood swings, depression and psychosis.
5.4.1 Anxiety and Paranoia
Across current NPS users overall, 25% (n=47) described use as increasing anxiety and 12% (n=22) reported experiencing paranoia as a result of use.
33 respondents who had used within the last 6 months provided information on mental health impacts of synthetic cannabinoids. Increased anxiety was identified by:
- Two in three (67%, n=22) people who had used synthetic cannabinoids within last 6 months
- Increased anxiety was also identified by over half (54%, n=99) of staff working with synthetic cannabinoid users.
23 respondents provided information on mental health impacts of stimulant-type NPS and mephedrone. An increase in anxiety was identified by:
- 43% (n=10) of people who had used within the last 6 months
- This was also the most frequently cited mental health effect noted by staff for mephedrone (34%, n=62) and stimulant-type NPS use (31%, n=57).
There was therefore a strong correlation between the perception of staff and those who reported using NPS about the role of synthetic cannabinoids, stimulant-type NPS and mephedrone in increasing anxiety. However, there was a noticeable difference in perceptions of the anxiety-producing effects of benzodiazepine-type NPS between those who took them and staff.
- Four in five of benzodiazepine-type NPS users (81%, n=47) said that use reduced their anxiety.
- 42% (n=77) of staff felt that the use of benzodiazepine-type NPS increased anxiety in those who took it.
Anxiety was also discussed by a number of interviewees in the qualitative interviews who reported use of these substances, particularly among those whose use was sustained. In particular, feelings of anxiety were often experientially bound up in feelings of paranoia, and to a lesser extent depression:
"It can cause like quite a lot of anxiety obviously because if you're fearful of like whether you're going to die on it [synthetic cannabinoids] or not, but like depression can be quite a big one off it too. Paranoia, because you can think people are talking about you behind your back, stuff like that, folk are looking at you." [105]
Overall, 17% (n=32) reported experiencing both anxiety and paranoia.
This overlap between anxiety and paranoia came out particularly strongly in survey results with people who had taken synthetic cannabinoids:
- almost as many synthetic cannabinoid users reported paranoia as a mental health effect (64%, n=21) as anxiety (67%, n=22), and 29% (n=10) reported both.
Similarly, as many stimulant type NPS users cited paranoia as a mental health effect (38%, n=5) as anxiety (38%, n=5), and 23% (n=3) reported both.
5.4.2 Mood Swings
Across those who had used NPS in the last six months, 15% (n=28) described mood swings as an effect of use. Mood swings were a main effect of use reported by almost half of the 13 respondents who reported on health effects of taking stimulant-type NPS (46%, n=6). This finding was supported by results for the staff survey, where it was the primary mental health effect identified in relation to stimulant use, cited by 32% (n=58) of staff working with people who use stimulant-type NPS.
Although not a main effect reported by those who took benzodiazepine-type NPS or mephedrone, mood swings were nonetheless a main mental health effect noted by 36% (n=67) of staff in relation to the use of benzodiazepine-type NPS and 30% (n=55) of staff in relation to mephedrone use.
Mood swings were discussed infrequently in interviews, and tended to be in relation to withdrawal rather than being under the influence:
"Mood swings, you know, in a state of anxiety at times when I couldn't get any gear [mephedrone]." [106]
5.4.3 Depression
Across those who had used NPS in last six months, 20% (n=38) described depression as an effect of use. Apart from mood swings, depression specifically was not reported as a main mental health effect in the NPS survey for any substance.
However, depression was noted by 25% (n=45) of staff in relation to any NPS. It was the second most common mental health effect of benzodiazepine-type NPS use, cited by 39% (n=71) of staff. It was also the third most commonly cited mental health effect of synthetic cannabinoids noted by staff (48%, n=88). GHB/ GBL, which was taken almost exclusively by MSM, similarly produced concerns about depression among 16% (n=30) of staff working with people who used these substances.
5.4.4 NPS and Underlying Mental Health Conditions
37% (n=94) of those who reported NPS use in the NPS survey were or had previously been in contact with mental health services. 52% (n=96) of staff identified exacerbating underlying mental health conditions as an effect of NPS overall. Of the four key NPS, this was highest for synthetic cannabinoids, and lowest for mephedrone.
Figure 5.1 gives an overview of staff perceptions on exacerbation of mental health by substance type.
Fig. 5.1 Percentage of staff identifying exacerbation of underlying mental health conditions as an effect of NPS use by NPS- type. [107]
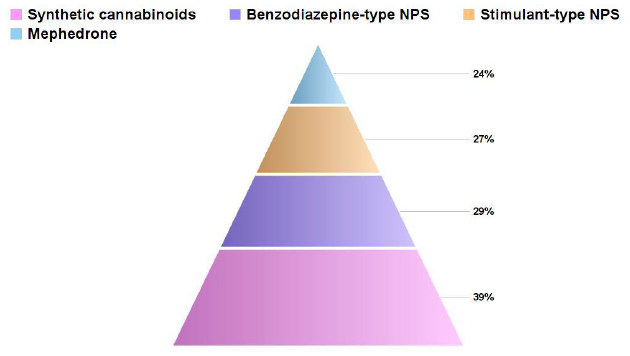
Base (n=184)
The interviews highlighted a range of different views, with some interviewees suggesting that their use of NPS had exacerbated their underlying mental health conditions:
"Aye but I've got the paranoia with the schizophrenia and that any way, so obviously that [ethylphenidate] made it worse." [108]
Others, however, felt that their mental health conditions were due entirely to their NPS use:
"My anxiety is bad, very bad and it's due to legal highs because I wasn't like that before I'd taken legal highs."
Interviewer: Had you had any mental health problems before you used legal highs?
"No." [109]
Others still, felt that their mental health conditions were entirely unrelated to their NPS use:
"Although I do suffer from depression, I don't link that to legal highs." [110]
This range of views was not consistent by either NPS of choice or type of mental health condition.
In focus group discussions with staff, NPS was seen to exacerbate underlying mental health conditions. It is important to note that very few survey or interview participants had used NPS exclusively and had other risk factors which could contribute to mental health issues including homelessness, adverse childhood events and family health histories. Therefore, although some participants attributed their mental health problems to their NPS use, it is not possible from this data to determine causality.
5.4.5 Psychosis
Psychosis was not specifically asked about in the NPS survey apart from the chemsex section as it did not emerge as a key theme in the qualitative interviews outside of MSM interviews. Very small numbers of MSM (n=3) reported psychosis as a mental health effect. It was not reported as a key mental health effect in the NPS survey for any substance. However, psychosis was the third most common mental health effect of stimulant-type NPS noted by staff, identified by 30% (n=55) of staff working with people who use stimulant-type NPS. Ethylphenidate, which was taken primarily by PWID, similarly produced concerns about psychosis among 19% (n=34) of staff working with ethylphenidate users.
Psychosis was discussed in focus groups, and one staff respondent felt that it was the move from heroin use to ethylphenidate use by their clients that had triggered an increase in psychosis across the population.
"All our clients, previous heroin users, had mental health problems but no mental illness, you know, working for years with no mental illness and then they start taking these legal highs and then they were displaying symptoms of psychosis, and some who will never recover from it and will be on medication for the rest of their lives". [111]
Another staff respondent highlighted the role of additional factors in psychotic symptoms including other drug use and sleep deprivation.
"It's difficult to sort of disentangle sometimes whether it's people stopping their heroin use as well, a lot of people sort of managing their behaviours with a lot of heroin and then when they stop using that and also not quite sure how much, we're attributing a lot to the drug, but just not sleeping for five days is very bad for you and I wonder, it would be interesting to sort of see how much of it is about sleep deprivation, the strain of psychosis that goes on. We're attributing a lot to this drug I think, but I don't know, but I do wonder how much, because people who drop their heroin use, sort of managing their behaviours sometimes." [111]
5.5 Physical Health Harms
There was more consensus in terms of staff and NPS users' perceptions of effects in relation to physical health than there was for mental health effects. When asked in the NPS survey about the effects of taking NPS on their physical health, across NPS users who had used in the last 6 months the main harms identified were problems with co-ordination (20%, n=38), difficulty sleeping (20%, n=37), and increased or decreased heart rate (14%, n=26).
The main physical health effects reported by those who had taken synthetic cannabinoids were exclusively negative. The main physical health effects reported in relation to benzodiazepine-type NPS, stimulant-type NPS and mephedrone were more ambivalent, with respondents including improvements to physical health as well as harms among their main effects.
5.5.1 Sleep Difficulties
Amongst those who reported currently using NPS in the NPS survey, 20% (n=37) reported difficulties sleeping. This was given as one of the main physical health effects by people who had used synthetic cannabinoids, stimulant-type NPS or mephedrone in the last six months.
- Of the 13 people who currently use stimulant-type NPS, 9 respondents (69%) reported that their use made sleeping more difficult for them.
- Of the 10 people who currently use mephedrone, 6 respondents (60%) reported that their use made sleeping more difficult for them.
This was supported by data from the staff survey. Staff identified sleeping difficulties amongst their clients in relation to stimulant-type NPS (36%, n=67) and mephedrone (30%, n=56).
In relation to benzodiazepine-type NPS, there were conflicting views amongst NPS users and staff:
- 91% (n=52) of benzodiazepine-type NPS users reported improved sleep
- 11% (n=6) of benzodiazepine-type NPS users reported sleeping difficulties, and
- 16% (n=30) of staff linked sleeping difficulties to benzodiazepine-type NPS use amongst their clients.
Difficulty sleeping as a result of synthetic cannabinoid use was also reported by both NPS users and staff:
- 36% (n=11) of synthetic cannabinoid users who had used in the last six months reported difficulty sleeping in relation to synthetic cannabinoids
- 26% (n=8) reported improved sleep, and
- 29% (n=53) of staff linked synthetic cannabinoid to sleeping difficulties amongst their clients.
Interview data revealed that taking synthetic cannabinoids often promoted sleep. Whereas this was viewed positively by some, such as Debbie (Section 5.2.3), others saw this sleep-promoting property as having a negative effect on their wellbeing ( "I was constantly tired, I was never sitting up, I was always lying down") [112] .
It is important to note that NPS survey respondents did not describe what they regarded as a sleeping difficulty or improved sleep e.g. the quality of their sleep, duration, ease of getting to sleep or whether it was uninterrupted.
5.5.2 Problems with Co-ordination
Problems with co-ordination were reported by 20% (n=38) of the currently using NPS survey respondents. This was:
- the primary physical health effect noted by people who have taken synthetic cannabinoids (42%, n=13)
- the secondary physical health effect reported by people who have taken benzodiazepine-type NPS (46%, n=26)
- not reported to be a health problem by any participants in relation to stimulant-type NPS or mephedrone use.
This is supported by findings from the staff survey. Problems with co-ordination were seen as:
- the main physical health consequence of benzodiazepine-type NPS use reported by 36% (n=66) of staff, and
- a key consequence of synthetic cannabinoid use reported by 33% (n=60) of staff.
By contrast, only 11% (n=20) of staff reported difficulties with co-ordination for either stimulant type NPS or mephedrone.
5.5.3 Seizures
Seizures were reported by 10% (n=18) of the currently using NPS survey respondents. Seizures were reported particularly by people who had used synthetic cannabinoids (39%, n=12). Seizures were not identified in the NPS survey as a main physical health effect of benzodiazepine-type NPS or stimulant-type NPS and none of the 10 current mephedrone users who responded to the questions on the physical health effects of mephedrone identified seizures as being associated with its use.
In contrast to this, only three staff respondents associated seizures with synthetic cannabinoid use. However, five staff did identify seizures as a main physical health effect of taking mephedrone.
Seizures (commonly called 'fits' or 'fitting') were a fairly commonly physical health effect noted during the qualitative interviews, impacting on those who have taken synthetic cannabinoids, mephedrone, and ethylphenidate. However, interviews revealed an ambivalence among some towards the perceived risks of 'fitting'. Most who discussed seizures during interviews looked upon this as a negative consequence:
"We had a joint out of it [Exodus - a synthetic cannabinoid], then I went all funny and all that on it and then I took a fit.... My sister saved my life from it, she found me after I'd had that Exodus in a joint." [113]
However the experiences of fitting did not always act as a deterrent to continued use:
"I remember of fitting, I remember of taking it [mephedrone] and then being in my bedroom and seeing my daughter, actually fitting, and seeing my daughter in her wedding dress. And I would see Jane, my mother-in-law, and then I would open my eyes to see an ambulance being there, eh. And I got took into the hospital, and then I'd come back out, and I'd still have four or five grams in my bra, and then I would do it again, eh. It was bad". [114]
One respondent saw fitting as a positive marker of efficacy:
"Most of the time [combining mephedrone with MDMA] was alright, but you would get the one person that would, or most of the time somebody was fitting or, most of the time me. If I didn't get a fit, I didn't think it was a good bit" [115]
While seizures were reported as a physical health effect by people who had used synthetic cannabinoids, and staff working with people who have used mephedrone, this does not necessarily mean that they were regarded as an unequivocally negative health experience, or a deterrent to future use.
5.5.4 Hunger and Weight Change
Decreased hunger was not a main physical health effect for people taking any of the four key NPS, and was reported by only 7% (n=14) of NPS survey respondents currently using NPS. Due to restrictions on the survey software, we were unable to give weight-loss as an option, so were required to phrase as decreased hunger.
However, unplanned weight loss emerged as a key theme in interviews. Realisation of unplanned weight change was often presented in the context of relationships with others. Nick described how it was only after seeing his mother after a six-month gap that he realised the severity of his weight loss:
"I didn't notice it was as bad as that at that point, but then it deteriorated until my mum came up, she hadn't seen me for six months, she said I looked like a junkie seeing how much weight I'd lost. That's when I decided to wean myself off it [Exodus - synthetic cannabinoid]." [116]
5.6 Social Effects
174 NPS survey respondents reported on social harms of NPS use. The main social effects reported by NPS survey participants across all groups and all key NPS types were spending more money than planned or selling something to pay for NPS, and missed appointments. Staff survey respondents identified debt, loss of employment and education, loss of tenancy and anti-social behavior as the main social effects of NPS use, common across all key NPS types.
5.6.1 Money and Debt
Of the 174 NPS survey respondents who reported on social harms, 60% (n=105) reported spending more money than planned or selling something to pay for NPS. This was highest among people in contact with mental health services (67%, n=49). [117]
Table 5.1 illustrates the borrowing and repaying data from NPS survey participants by risk group.
Table 5.1: Borrowing & repaying debt
| |
Total respondents | Have ever borrowed money to pay for NPS | Always been able to repay | Never been able to repay | |||
| N | N | % | N | % | N | % | |
| Homeless | 75 | 44 | 58 | 22 | 49 | 3 | 7 |
| PWID | 131 | 69 | 53 | 37 | 58 | 7 | 11 |
| Mental Health Service Users | 92 | 43 | 46 | 29 | 64 | 1 | 2 |
| Young People | 35 | 15 | 43 | 8 | 56 | 2 | 13 |
| MSM | 33 | 6 | 18 | 5 | 16 | 1 | 3 |
| Overall [118] | |
89 | 39 | 51 | 50 | 9 | 9 |
In interviews, participants discussed borrowing (and stealing) from friends and family members, often resulting in damage to those relationships, selling possessions and pawning items to pay for NPS:
"Just borrowing off my dad, selling my hoose, selling my whole hoose. All I've got left is my washing machine and my couch". [119]
5.6.2 Missed appointments
Use of NPS also correlated strongly with missed appointments. Of the 174 NPS NPS survey respondents who reported on social harms, 60% (n=104) reported missing appointments such as with the Job Centre, GP or treatment as a result of their NPS use.
This was lowest among MSM (44%, n=10) and vulnerable young people (54%, n=14) and highest among homeless people (72%, n=41), people with in contact with mental health services (71%, n=52) and people who inject drugs (66%, n=67). [120] Even among the groups with lower rates of missed appointments, almost half of these groups had missed an appointment due to NPS use.
5.6.3 Education and Employment
Loss of education and employment was the second most frequently identified social harm associated with NPS use in the staff survey after debt. Overall, it was identified by 49% (n=91) of staff, and specifically as:
- the primary social harm associated with mephedrone use, identified by 23% (n=43) of staff
- a main social harm identified in relation to synthetic cannabinoids, identified by 32% (n=58) of staff, and
- a main social harm identified in relation to benzodiazepine-type NPS, identified by 25% (n=46) of staff.
Problems with work or employment did not appear as one of the three main harms identified by any group within the NPS survey except MSM, just over half of whom (52%, n=12) identified it as consequence of NPS use. 46% (n=12) of vulnerable young people and 32% (n=23) of people in contact with mental health services who answered the question on social effects of NPS use cited problems with work or employment as a consequence of NPS use. This suggests that while not among the most important effects identified by NPS survey respondents outside the MSM group, problems with work or employment nonetheless affected a notable minority of NPS survey respondents.
5.6.4 Loss of Tenancy
Loss of tenancy was also frequently identified as a social harm associated with NPS use in the staff survey. It was identified by 49% (n=90) of staff overall, and specifically by:
- 29% (n=54) of staff in relation to the use of synthetic cannabinoids
- 23% (n=43) of staff in relation to benzodiazepine-type NPS, and
- 21% (n=39) of staff in relation to stimulant-type NPS.
Loss of home or tenancy did not appear as one of the top three main harms amongst any group in the NPS survey, being reported by 20% (n=35) of respondents who answered a question on problems caused by NPS overall.
Other social harms mentioned by front line workers in the staff survey were anti-social behavior (particularly in relation to the use of benzodiazepine-type NPS and stimulant-type NPS), for which it was identified as a main harm. In addition, increased aggression, involvement in sex work, the carrying of knives and other weapons due to paranoia and increased involvement in crimes such as shoplifting to fund NPS use were also other reported social harms by respondents to the staff survey.
5.7 NPS Use and Relationships
Taking NPS was seen by both NPS survey and staff survey respondents to affect relationships, particularly damaging relations with family and impacting on ability to fulfill caring commitments. Gender-based and intimate partner harms also emerged as a theme in qualitative data collection.
5.7.1 Relations with Family, Partners and Friends
Respondents to the NPS survey were asked to identify whether they thought the effect of their NPS use had a positive, no effect or a negative effect on key relationships. Across all groups the majority of respondents (47%, n=117) felt that taking NPS had had an overall negative effect on family relationships. Considering responses from each of the five population groups, MSM were the only group where this was not the top negative relationship impact. Qualitative data illustrates that this damage to relationships could extend from minor conflict to being disowned by family:
"My full family disowned me a couple of weeks ago due to legal highs [synthetic cannabinoids], going to prison because I'm stealing things, like stealing £6 out her [mum's] purse, tenners and that - wasn't thinking about that at the time, was just like that's another £6 man and that was a gram.... They've just all disowned me." [121]
Over a third of all respondents to the NPS survey reported experiencing a negative impact on their relationships with partners (37%, n=93). Interviews revealed that damage to relationships with partners often resulted in relationships ending, as John, quoted above, goes on to say:
"My missus is trying to break it up, know what I mean. We did split up there for a while because obviously of legal highs and I almost lost my girlfriend through legal highs." [121]
Across all groups, the third most impacted relationship was friendship, although 63% (n=159) of respondents to the NPS survey reported that taking NPS had had no effect on friendship. Again, the interviews provided an insight into the nature of this type of harm, by highlighting damage to friendships due to either losing interest in friendship:
"You basically just seclude yourself when you've got these [synthetic cannabinoids]. I mean friends and family that I've known for 20 years, I disowned them." [122]
Or becoming isolated from non- NPS taking friends:
"When I started smoking legal highs [synthetic cannabinoids], none of my friends wanted to be with me because I would be at a party and they would all be drunk and I would be sitting there rolling a legal joint and just sparking it up. Everybody would be like, "What's that smell? Is somebody smoking legals in this house?" I'd be like, "Yeah, it's me, what the fuck's your problem?" [123]
5.7.2 Fulfilling Caring Commitments
Struggling to fulfill caring commitments was reported by 26% (n=45) of NPS users who answered the question on social harms of NPS.
- Of the 73 people in contact with mental health services who provided information on social harms, (33%, n=24) reported struggling to fulfill caring responsibilities
- Of the 102 PWID who provided information on social harms, (26%, n=27) reported struggling to fulfill caring responsibilities
- Of the 57 homeless people who provided information on social harms, (21%, n=12) reported struggling to fulfill caring responsibilities
- Of the 26 vulnerable young people who provided information on social harms, (19%, n=5) reported struggling to fulfill caring responsibilities, and
- Of the 23 MSM who provided information on social harms, (17%, n=4) reported struggling to fulfill caring responsibilities.
Staff working with these populations also reported on whether they thought NPS had an impact on their clients' caring commitments. Over half of staff that worked with any group thought that NPS had an impact on fulfilling caring responsibilities (57%, n=105). This ranged from 63% (n=83) of staff working with PWID to 55% (n=45) of staff working with vulnerable young people.
Broken down by substance, difficulties with their clients managing caring responsibilities were reported by:
- 37% (n=68) of staff working with benzodiazepine-type NPS users
- 34% (n=63) of staff working with synthetic cannabinoid users
- 26% (n=47) of staff working with mephedrone users, and
- 23% (n=42) of staff working with stimulant-type NPS users.
Where participants discussed children in interviews, they did not talk about difficulties they had managing childcare, but rather the role that parenthood played in decisions to reduce or stop their NPS use:
Interviewer: What do you think the main things were that got you to stop [using mephedrone]?
"Losing my son. They were gonna take him off me. And I just couldn't, I wouldn't have been able to live with myself." [124]
5.7.3 Gender-Based and Intimate Partner Harms
For ethical reasons, gender-based and intimate partner harms were not asked about in the NPS survey, however they did emerge as a relationship theme in focus group discussion with front line workers. Concerns raised by staff focused primarily on concerns about consent in the context of chemsex (both among MSM and heterosexual couples), and concerns about the vulnerability of young women in public places due to intoxication, and sex-for-drugs relationships with vendors, particularly in shops were also highlighted.
In addition to these harms which cut across all populations, a number of population-specific harms emerged.
5.8 Population-Specific Harms
Population-specific harms were identified in relation to chemsex among MSM, injecting NPS among PWID and unsupervised opiate detoxification among opiate users. These groups represent small sub-groups of total NPS survey respondents. However, considering them separately provides an opportunity to explore reported consequences of NPS use in more depth.
5.8.1 Chemsex
All MSM who had ever used NPS (n=38) were invited to complete an additional survey section on chemsex. This section of the report focuses on the 29 respondents who completed this part of the survey, which addressed the physical and mental health effects of NPS use during their last chemsex experience.
Of the 29 MSM who answered survey questions on chemsex, 15 reported no change to their mental health either during or after their last chemsex experience:
- Just over half (n=15) reported feeling happier
- Just under half (n=14) reported feeling more confident during their last chemsex experience, and
- Just under one third reported feeling regret (n=9) and shame (n=8) after their last chemsex experience.
Physical effects reported were increased sexual function during (n=13) and after (n=1) their last chemsex experience. Under one quarter reported decreased sexual function during (n=7) and after (n=1) their last chemsex experience. Just under half (n=14) reported disturbed sleep after their last chemsex experience. Five reported blackouts during their last chemsex experience, one afterwards, and two both during and after their last chemsex experience.
Disinhibition following NPS use during sex emerged as a theme in interviews with MSM and some heterosexual participants. [125] Interviewees discussed disinhibition leading to unsafe sexual practices. Disinhibition was also described as having an effect on drug choices, and routes of administration, including being injected by others.
"At the end when I'm trying to inject myself, so I'm saying 'Can you inject me now?'". [126]
The feelings of shame and regret noted above were also linked to disinhibition.
"I even found myself doing things like, sexually, that I would just not entertain either, you know. Just 'cause I was like, away with it on this drug [mephedrone], you know.... Your inhibitions are just totally gone, and so I did, I found myself in situations that, you know, when I think back, like it does, it makes me cringe." [127]
Twenty-four MSM answered questions about the social consequences of their last chemsex experience. Over half (n=15) reported no social consequences to their most recent chemsex experience. Slightly under one third (n=7) did identify having spent more money than they intended to. Three participants said that their last chemsex experience had resulted in damage to their relationship with their partner, and one said it had improved it. Two participants stated that they lost friends as a result of their last chemsex experience, in contrast to one participant who made new friends.
5.8.2 Injecting NPS
All PWID who completed the survey (n=141) reported taking traditional drugs, and of these, 97% also used NPS. Of those who used both traditional drugs and NPS, only 35% injected NPS (the remainder used other routes of administration). This section focuses on the 47 respondents who had ever injected NPS and the nine respondents who reported current injecting of NPS at the time of the survey.
Among the nine current injectors, the majority (n=6) did so on a daily basis, an average of five times a day. Arms were the most popular injection site (n=8), but five reported they used multiple sites. All nine current injectors did so intravenously. Two always and four occasionally used vitamin C or citric acid to prepare their NPS.
Five out of nine reported sharing their needles and seven reported sharing injecting equipment. Six reported occasionally using without a filter and therefore not removing the impurities from the substance, increasing the risk of injecting related complications.
When asked about their injecting experience, five said they often felt a burning sensation while injecting, and seven reported occasionally having irritation at the injecting site. Six occasionally experienced redness at the injecting site. Seven occasionally missed hits, four occasionally got infections. Seven of the nine never got abscesses and none reported collapsed veins. One of the nine had been hospitalised for their wounds.
5.8.3 Unsupervised Opiate Detoxification
Finally, a theme which emerged in the qualitative data was in connection to unsupervised opiate detoxification. This was most commonly associated with use of ethylphenidate and mephedrone.
Some opiate users described the role of mephedrone or ethylphenidate in their reduced opiate consumption in positive terms, as illustrated below:
"Psychologically, you'd forget to take your script and the next minute we were all clean." [128]
However, staff working with these populations expressed concerns about medically unsupervised withdrawal from opiates and opiate replacement treatment ( ORT) with NPS, with one noting a reverse trend back towards opiate use:
"Yes a few of our guys after the ethylphenidate ban started using mephedrone and.... it was more expensive and they were also finding it heavy on their chest I think as well. I had reports of them feeling like they were going to have heart attacks and stuff with the mephedrone. So it's kind of gone back to heroin." [129]
5.9 Discussion
There are a wide range of harms that span the use of different NPS. It is difficult to attribute specific harms to specific substances definitively as harms experienced may be in part due to factors such as poly-use or pre-existing health issues. Harms are also interpreted differently (some 'harms' aren't seen as such by some users).
The NPS and staff surveys reveal important differences in perception of the mental health effects of NPS between those who have taken NPS and staff in services. Benzodiazepine-type NPS users identified use with reduced anxiety and increased relaxation. In contrast, staff identified use of benzodiazepine-type NPS with increased anxiety. In line with discussion on motives for use, this can most likely be explained in terms of a concern of experiencing rebound anxiety [130] and other withdrawal effects. [131] This suggests a need to continue developing our knowledge of the consequences of NPS use and the impact of NPS on mental health and wellbeing in order to develop effective treatment responses.
The vast majority of people who have taken benzodiazepine-type NPS and a minority of people who have taken synthetic cannabinoids reported improved sleep. In contrast, improvements in sleep were not recognised as a physical health effect for either substance by staff. In addition, a number of respondents reported that synthetic cannabinoid use led to sleeping difficulties. Qualitative data suggest that these difficulties included both excessive sleep and being unable to sleep. Current research on cannabis use shows that withdrawal from sustained cannabis use can lead to sleeping difficulties [132] , suggesting a possible parallel with effects of synthetic cannabinoid withdrawal on sleep.
The risk of overdose with benzodiazepine-type NPS is high, especially when used in conjunction with other substances. This is evidenced by the role of benzodiazepine-type NPS in drug related deaths in Scotland. [133] There are also clear risks in relation to potential patterns for overdose when someone returns to opiate use with a reduced tolerance. These risks are clearly documented with increased rates of overdose following liberation from prison. [134] Both these issues highlight the need for improved information and treatment responses.
There are also specific harms associated with patterns of use and route of administration. This highlights an information need for both NPS users and staff who support them. Patterns of behaviours such as frequent injecting or equipment sharing can lead to injecting related injuries including abbesses [135] or risk of contracting blood borne viruses such as HIV and Hepatitis C. [136]
Finally, this chapter has also shown that there are specific harms associated with population-specific groups such as chemsex amongst MSM, which impact on people who use NPS. This poses a challenge for services to engage with populations not in treatment but whose NPS use and associated behaviours are likely to result in significant risks to those who use NPS and wider public health.
Contact
There is a problem
Thanks for your feedback