NHS Scotland assets and facilities 2016: annual report
Sixth edition of the state of NHS Scotland assets and facilities report (SAFR).
1.0 Performance of NHSScotland's Assets
This section of the report provides an overview of the current state of NHSScotland's assets whilst also reviewing asset and facilities services performance. The intention is to gain an insight into the significance of this asset base and also to appreciate where opportunities lie for improving performance.
The data used within this report is based on that currently available and reported from the beginning of the financial year 2016/17 i.e. April 2016. This includes:
- The latest asset performance information provided by NHS Boards in May 2016 covering property, office accommodation, vehicle and medical equipment assets.
- The latest facilities management costs published within the Scottish Health Service Cost Book (published in December 2015), covering NHS Boards' annual accounts for the reporting period 2014/15.
- PPP/ PFI service charge costs from NHS Board's audited accounts for 2014/15.
- Information from NHSScotland's 2016 patient questionnaire survey which reports every two years.
- The limited available information on eHealth IM&T asset cost information, which was collated in 2012.
All 22 NHS Boards have contributed to this report by submitting their annual asset performance returns during May 2016.
All costs reported in this document include the impact of inflation but exclude the cost of VAT or other on-costs, unless specifically noted.
1.1 The Current Status of NHSScotland's Property Assets
The following provides an overview of the current status of NHSScotland's assets, with some comparative information on annual changes. More detailed information on the current status of property assets can be found in Annex A of this report.
| Current status of NHSScotland's property assets | |||
|---|---|---|---|
| Current Net Book Asset Value (all assets) | 2016 | ||
| Property: | £5.6bn | ||
| Other: | £0.6bn | ||
| Total: | £6.2bn | ||
| Floor Area ('000's sq.m) | 2014 | 2015 | 2016 |
| Total: | 4,512 | 4,478 | 4,434 |
| Age (% less than 50 years old) | 2014 | 2015 | 2016 |
| 74% | 78% | 77% | |
| Condition (Good - category A or B) | 2014 | 2015 | 2016 |
| 58% | 66% | 70% | |
| Estate Utilisation (Fully Utilised) | 2014 | 2015 | 2016 |
| 77% | 81% | 83% | |
| Functional Suitability (Good - A or B) | 2014 | 2015 | 2016 |
| 65% | 72% | 69% | |
| Backlog Maintenance | 2014 | 2015 | 2016 |
| Including Inflation uplift | £789m | £898m | £887m |
| Excluding inflation uplift | £809m | £763m | |
Most NHS Boards have reported a general improvement in the condition of their estate and utilisation of accommodation this year, along with a slight improvement in overall backlog maintenance. The change in functional suitability is mainly due to a reassessment of a small number of buildings across a few Boards.
1.2 The Current Status of NHSScotland's Vehicle Assets
The following provides an overview of the current status of NHSScotland's vehicle assets, with some comparative information on annual changes. More detailed information on the current status of vehicle assets can be found in Annex B of this report.
| Current status of NHSScotland's vehicular assets | |||
|---|---|---|---|
| Number of Vehicles | 2014 | 2015 | 2016 |
| Owned*: | 1,897 | 1,932 | 1,938 |
| Leased: | 2,178 | 2,516 | 2,264 |
| Staff Car Scheme: | 6,485 | 5,548 | 5,356 |
| Long term hire: | 198 | 155 | 222 |
| Total: | 10,758 | 10,151 | 9,780 |
| Age (% less than 5 years old) | 2014 | 2015 | 2016 |
| 85% | 83% | 81% | |
| Total Mileage (000's) | 2014 | 2015 | 2016 |
| Owned: | - | 30,616 | 32,900 |
| Leased**: | - | 24,332 | 19,841 |
| Staff Car Scheme**: | - | 27,049 | 21,533 |
| Private Car Business Travel: | - | 51,690 | 51,093 |
| Total: | - | 133,688 | 125,368 |
| Fuel Type | 2014 | 2015 | 2016 |
| Petrol: | - | 21.9% | 20.6% |
| Diesel: | - | 77.7% | 78.7% |
| Alternative: | - | 0.4% | 0.7% |
* 65% of NHSScotland's owned vehicles belong to the Scottish Ambulance Service.
** The Leased figures and Staff Car Scheme figures do not include Long and Short Term Hire vehicles
The quality of information returned by NHS Boards on their vehicle assets has further improved this year again (but with scope for further improvement). This enables more information to be presented on the current state of these assets. The age profile of these assets suggest that they are in good condition and thus well maintained, with some Boards suggesting that vehicles beyond 5 years old are often due to their lower annual mileage enabling an extended life.
1.3 The Current Status of NHSScotland's Medical Equipment Assets
The following provides an overview of the current status of NHSScotland's medical assets, with some comparative information on annual changes. More detailed information can be found in Annex C of this report.
| Current status of NHSScotland's medical equipment | ||
|---|---|---|
| Replacement Cost* | 2015 | 2016 |
| Radiotherapy equipment | £66m | £65m |
| Imaging equipment | £269m | £271m |
| Renal dialysis equipment | £16m | £16m |
| Cardiac defibrillators | £20m | £20m |
| Flexible endoscopes | £84m | £78m |
| Infusion devices | £37m | £34m |
| Other high value equipment: | £440m | £438m |
| Other low value medical equipment | n/a** | £108m |
| TOTAL: | £932m | £1,030m |
| Radiotherapy equipment (linear accelerators and CT simulators) |
2015 | 2016 |
| Number of items: | 35 | 38 |
| Proportion within minimum lifecycle age: | 100% | 100% |
| Imaging equipment | 2015 | 2016 |
| Number of items: | 2,745 | 2,658 |
| Proportion within minimum lifecycle age: | 69% | 70% |
| Cardiac Defibrillators | 2015 | 2016 |
| Number of items: | 3,850 | 3,926 |
| Proportion within minimum lifecycle age: | 85% | 78% |
| Infusion Devices | 2015 | 2016 |
| Number of items: | 20,190 | 20,757 |
| Proportion within minimum lifecycle age: | 76% | 73% |
| Flexible endoscopes | 2015 | 2016 |
| Number of items: | 3,035 | 3,106 |
| Proportion within minimum lifecycle age: | 85% | 81% |
| Renal Dialysis | 2015 | 2016 |
| Number of items: | 944 | 980 |
| Proportion within minimum lifecycle age: | 66% | 63% |
* estimated cost of replacing all medical equipment, & leased / privately financed equipment
** n/a - represents comparative data not available in 2015
Medical equipment is a valuable asset both in monetary terms and in the important role it plays in the delivery of quality and safe healthcare across NHSScotland. The annual change in the replacement cost of medical equipment is mainly due to this year's addition of data for low value medical equipment (less than £5k for an individual item), which adds a further circa £100m. Improved information also makes it possible to report on the proportion of each type of equipment that is within the minimum recommended age before needing to consider its replacement (Proportion within minimum lifecycle age). This suggests that many of these categories of equipment are getting older, except radiotherapy and imaging equipment which have nationally coordinated replacement programmes to ensure that equipment is replaced within its minimum lifecycle age.
1.4 National Asset and Facilities Performance Framework
A key objective of this report is to monitor year on year change in asset and facilities services performance, and the National Asset and Facilities Performance Framework (below) has been used since first introduced in 2011 to provide an essential link between asset and facilities services performance and patient needs, as defined in the NHSScotland Quality Strategy's three Quality Ambitions.
The Framework uses 20 key performance indicators to monitor year on year progress in asset performance towards the achievement of the 2020 Vision targets. It should be noted that the 2020 Performance Targets are (a) aspirational and subject to review to reflect funding availability and the outcome of the work on the 2020 Visioning, and (b) based on the qualification that their attainment will not reduce service quality. Broadly, half of the KPIs are based on quality measures and half are based on cost measures.
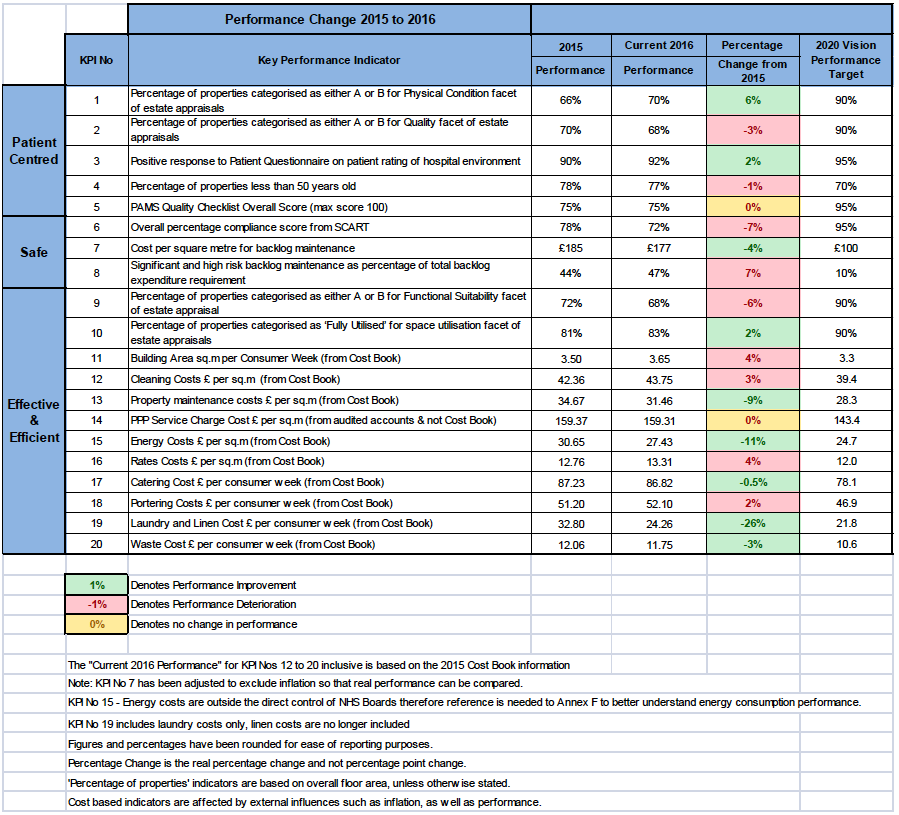
Annual changes to these KPIs are further explained in the following section.
1.4.1 Changes in National Asset Performance Framework KPIs
The following provides an overview of performance change between 2011 (when the performance framework was first developed) and 2016, along with a short commentary on the changes.
| KPI Nos 1 to 10 - Derived from property appraisal information and PAMS provided by Boards (Note: 'Percentage of properties' indicators are based on floor area, unless otherwise stated). | |
|---|---|
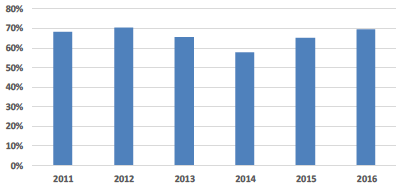
| Physical Condition (Percentage of estate area in Category A & B) |
Physical Condition Over that last three years there has been a steady improvement in the reported physical condition of the estate. Contributions to this improvement includes:
|
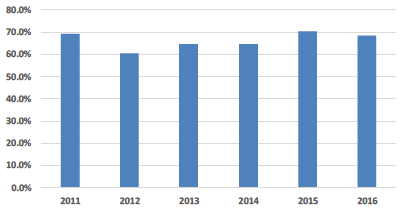
| Quality (Percentage of estate area in Category A & B) |
Quality This facet tends to show a broad correlation with the physical condition facet, but indicates a small decrease this year. Over the next few years it is expected to improve in line with physical condition as investment in new facilities is implemented. |
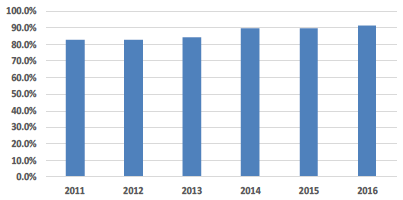
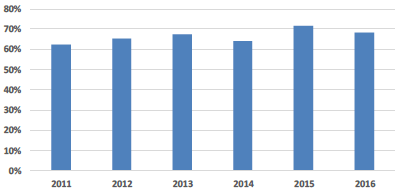
| Positive Patient Rating of Hospital Environment |
Patient Rating of the Hospital Environment There has been a gradual rise in this indicator of patients' opinion on the quality of the hospital environment. Patients with a positive response to their environment whilst in hospital have reached 92% for the first time in 2016. This is an extremely encouraging response rate. |
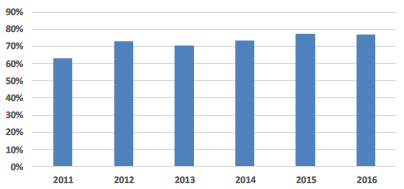
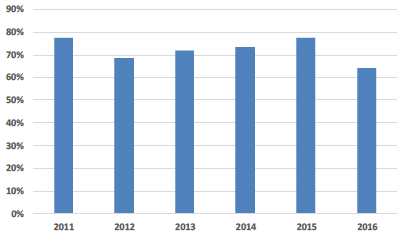
| Properties less than 50 years old |
Properties less than 50 Years Old The proportion of properties less than 50 years old has steadily improved over the full reporting period which is indicative of the substantial investment programme that has taken place over that period. This indicator has however remained relatively static over the last 12 months. Future investment projects are expected to compensate for a naturally aging estate to support continued improvement in this indicator, which includes:
|
| Overall SCART Score |
Overall percentage compliance score from SCART SCART is a self-assessment tool that indicates general compliance with policies and procedures related to property aspects of statutory compliance. This tool has recently been expanded to cover a wider question set and, as it begins to be adopted, is the reason why there is a temporary dip in the indicator this year. |
| Backlog Cost per sq.m (excl. inflation) |
Backlog Maintenance Cost per sq.m. This indicator excludes the impact of inflation to provide a more realistic indictor of performance in reducing the proportion of backlog maintenance within the current estate. Backlog per square metre has reduced by circa 21% since 2011, which includes a further reduction over the last 12 months. This reflects the continued focus on reducing backlog maintenance. Section 1.4.3 provides further details on the current status and movement of reported backlog maintenance. |
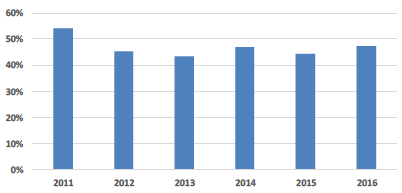
| Percentage of High and Significant Risk Backlog |
Proportion of Significant & High Risk Backlog Maintenance The main impact on this indicator this year has been the identification of infrastructure maintenance works needed at Ninewells Hospital in NHS Tayside, which has mainly been assessed as either Significant or High risk. Most other Boards have managed to reduce this category of backlog maintenance this year. |
| Functional Suitability (Percentage of area in Categories A&B) |
Functional Suitability The change in this indicator for 2016 has mainly been a result of a reconfiguration and/or reassessment of parts of NHS Boards' estate. The programme of new investment projects to be delivered over the next 5 years should help to improve this indicator in future years as it delivers modern, service designed accommodation. |
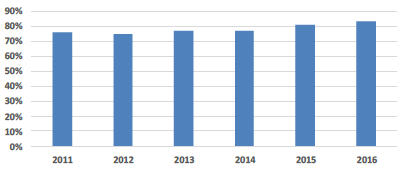
| Space Utilisation (Percentage of area fully utilised) |
Fully Utilised Space The efficient use of NHSScotland's estate continues to improve as shown by this indicator. Also, the accompanying reduction in overall floor area suggests an effective rationalisation programme is taking place following completion of new facilities. |
| KPI Nos 11 to 20 - Cost Book Derived KPIs Note: 2016 SAFR Cost Book data is based on financial information for financial year 2014/15 | |
|---|---|
| As part of the measures to improve the quality and consistency of data, the unit of measurement for building size was changed from 100 cu.m to sq.m in the 2012 Cost Book. Therefore, comparisons can only be made for the last four years on these KPIs. | |
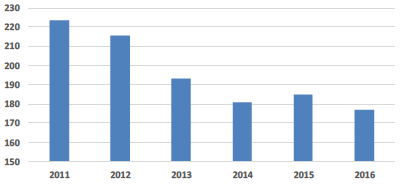
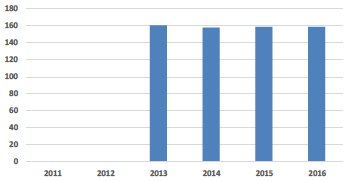
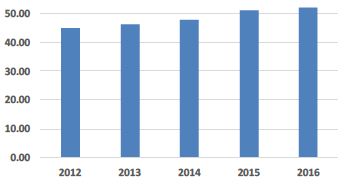
| Building Area (sq.m) per Consumer Week |
Space Utilisation - Building Area per Consumer Week This indicator shows the hospital estate floor area relative to inpatient service activity. The SAFR 2016 data is based on reported cost information for 2014/15 which was a transition year for Glasgow as it introduced its major new hospital in South Glasgow before then being able to remove the associated redundant estate. This is a key reason why this indicator has increased this year. |
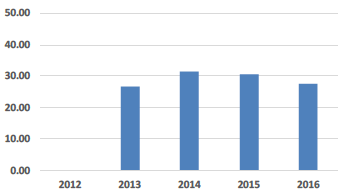
| Cleaning Costs £ per sq.m |
Cleaning Costs Higher cleaning standards as a response to increased HAI standards of cleanliness, increased activity and usage of space, and normal inflationary / salary cost pressures have all impacted on this KPI. However, this seems to be offset by efficiency performance improvements which have reduced such increases to below inflation levels. |
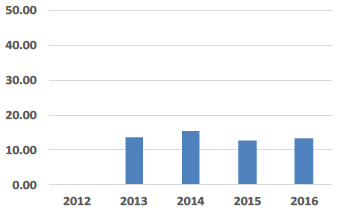
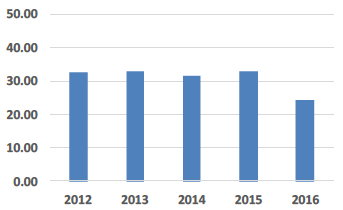
| Property Maintenance £ Costs per sq.m |
Property maintenance costs Property maintenance costs have reduced slightly this year which is mainly as a result of varying revenue spend on backlog maintenance included in the expenditure figures for property maintenance. |
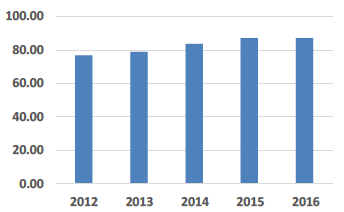
| PPP Service Charge Cost per Sq.m |
PPP - Service Charge Costs This KPI shows only the service charge element of PPP/ PFI operating costs taken from NHS Boards' audited accounts (i.e. not from Cost Book information). It doesn't include interest or recharge payment elements of a unitary charge. The 2016 KPI shows very little change from that reported last year despite any inflationary pressures. |
| Energy Costs £ per sq.m |
Energy Costs This KPI shows a slight reduction in energy costs per square metre over the last year which is mainly as a result of reduced energy consumption during a year of generally milder temperatures. However, as energy cost changes are outside the direct control of NHSScotland then energy efficiency improvements are the main measure for reducing consumption and thus overall costs. Further information on energy performance is provided in Annex D. |
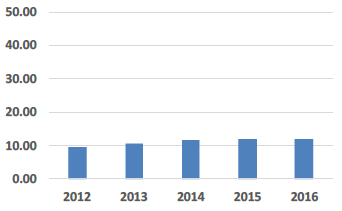
| Rates Costs £ per sq.m |
Rates Costs Rates are generally index linked to inflation which is the main reason behind the small increase in this indicator. |
| Catering Costs £ per Consumer Week |
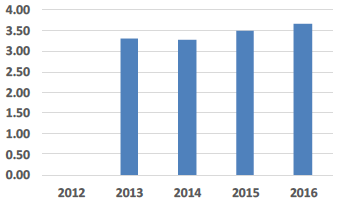
Catering Cost £/consumer week This KPI shows a steady increase in catering costs per consumer week over the five year reporting period during which time patient choice and food quality have both improved. The cost impact of these improvements in service delivery seems to be offset by efficiency performance improvements as the costs increases are generally lower than inflation over the same period. |
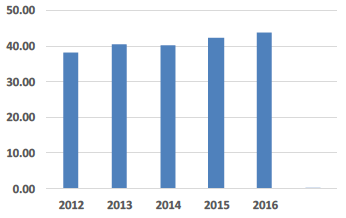
| Portering Costs £ per Consumer Week |
Portering Costs Boards explain that their Portering service is being used to carry out additional tasks in order to reduce pressures on front-line staff and the need for additional security staff in some instances. This is a key reason why the cost per consumer week has steadily risen since 2012. |
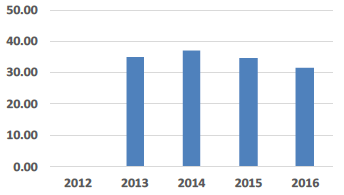
| Laundry & Linen Costs £ per Consumer Week |
Laundry (& Linen) Costs Laundry & linen costs have generally remained the same since 2011, despite inflationary pressures. However, the reduction in this indicator for 2016 is mainly due to a change in reporting of this cost as it no longer includes the cost of linen i.e. it now only includes laundry costs. Efficiency measures such as the move from conventional linen to fitted bedding have helped to control any cost increases. |
| Waste Costs £ per Consumer Week |
Waste Costs The cost associated with increased regulation on clinical waste and stricter controls over the segregation and disposal of waste have both put pressure on overall waste costs since 2012. |
The scale of the above cost charts has, when convenient to do so, been kept at 0 - 50 to enable comparison of the scale of costs between charts.
The Strategic Review of Soft Facilities Management Services Programme and the Facilities Shared Services Review are both carrying out strategic reviews of FM services across NHSScotland to identify further improvements and efficiencies that can be made to these services.
It should be noted that a number of the above Cost Book derived KPIs use "consumer weeks" as the denominator in the KPI. This is primarily a measure of inpatient activity however it also takes some account for day patient activity. Studies have shown that it is primarily inpatient activity which drives the numerator in each of these KPIs i.e. the two variables in each of these KPIs are highly correlated.
1.4.2 Performance variation across Boards
The Performance Framework is intended to provide a useful "national picture" of performance on a range of asset and facilities management services. The tables that follow compare each Board's performance on each of the 20 KPIs in the Framework. However, it should be recognised that comparisons between NHS Boards should be treated with some caution because:
- The size and scope of each Board's estate has historically developed in different ways over time.
- Increased spending can be a result of an improvement initiative.
- Boards may use different service delivery models to suit local circumstances i.e. number and type of duties carried out by domestic services staff may vary from site to site.
- Smaller Boards will be unable to achieve the economies of scale evident in the larger Boards.
- There are different specifications between Boards in the scope of each service.
- Allocation of costs between services and sites may not be uniform.
- Annual variances in non-recurring expenditure may distort operational KPIs i.e. expenditure on backlog incorporated within annual property maintenance costs.
- The introduction of new initiatives which improve performance take time to implement across NHSScotland.
- Clinical complexity / specialist services vary between hospitals and may drive cost differentials i.e. specialist clinical activity may result in higher clinical waste quantities and costs.
- Differences in pay and supplies costs across geographic areas i.e. some Boards may incur higher cost arising from remote and rural locations.
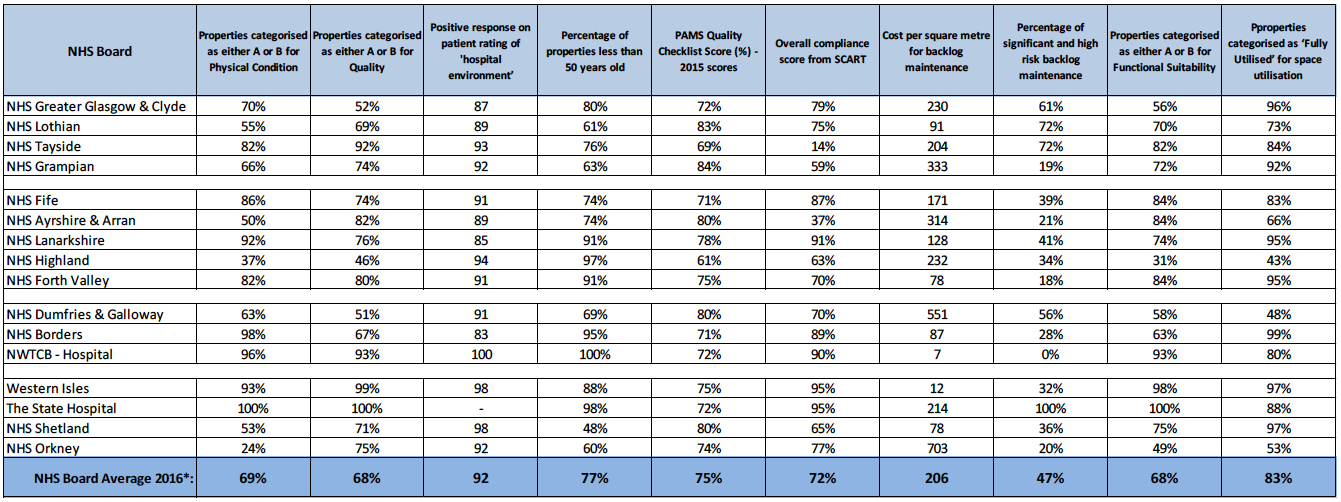
The size, scope and historical development of each Board's estate influences the 2011 starting performance base indicator and thus continues to impact on Boards' variation from the NHS Board Average.
Backlog in this table includes the cost impact of inflation.
The NHS Board Average 2016 excludes NHS Special Boards*
The PAMS Quality Checklist score is now only carried out every two years when Boards submit their full PAMS, hence, the 2015 scores are recorded in the above table.
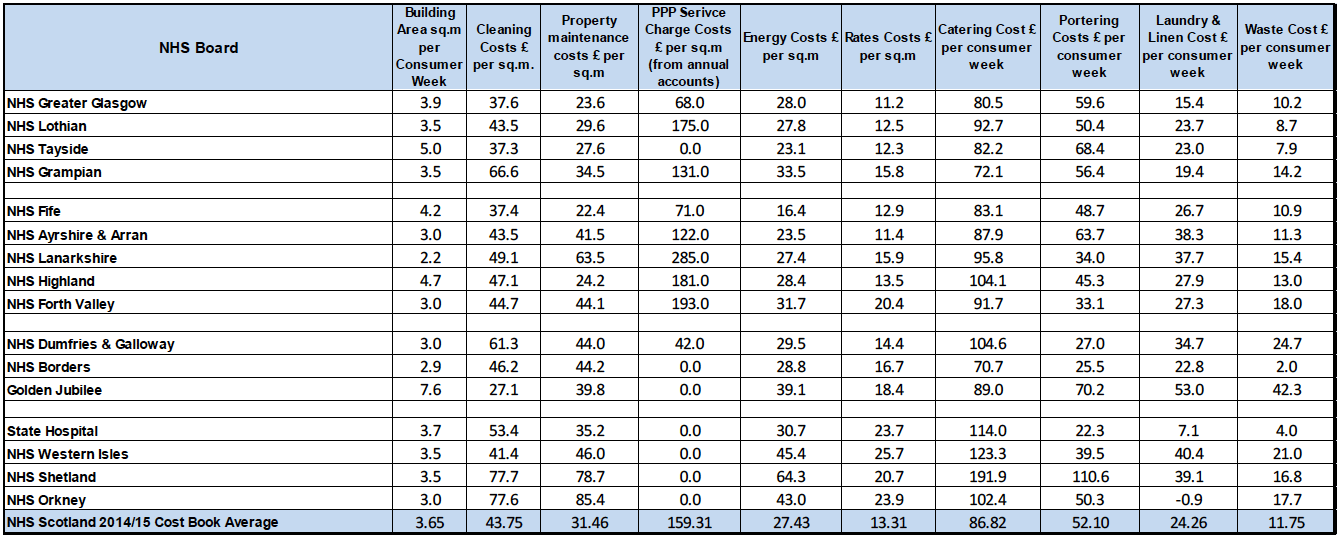
Comparisons between NHS Boards should be treated with some caution for the reasons outlined at the beginning of this section.
Cost information is sourced from the latest Cost Book data for 2014/15.
PPP Service Charge Costs are derived from Boards annual accounts and their proportion of PPP accommodation.
1.4.3 Current status of Backlog Maintenance
The current backlog maintenance expenditure requirement is the base cost required to bring those parts of the existing estate which are currently not in satisfactory condition, back to Condition B (satisfactory). It is, however, only a singular reference to understanding the current state of the estate and should not be considered in isolation to other important indicators such as the physical condition, age, and functional suitability of available accommodation; as described earlier in the National Asset and Facilities Performance Framework.
The 2016 backlog maintenance expenditure requirement is reported as £887m, which is a decrease of circa £11m since 2015. When the impact of inflation on costs is excluded from this indicator, the reduction in backlog maintenance has been circa £45m. Contributors to this reduction include:
- NHS Greater Glasgow & Clyde: (£23m).
- NHS Lanarkshire: (£14m).
- NHS Lothian: (£13m).
- NHS Grampian: (£12m).
- NHS Fife: (£8m).
The main increase in backlog is seen at NHS Tayside, who have identified the need to invest in the engineering service infrastructure at Ninewells Hospital, which has increased their reported figure by £27m (excluding inflation).
The following chart provides a breakdown of the current total £887m of backlog maintenance across each NHS Board:
Backlog Maintenance Comparison - NHSScotland Total is £887m
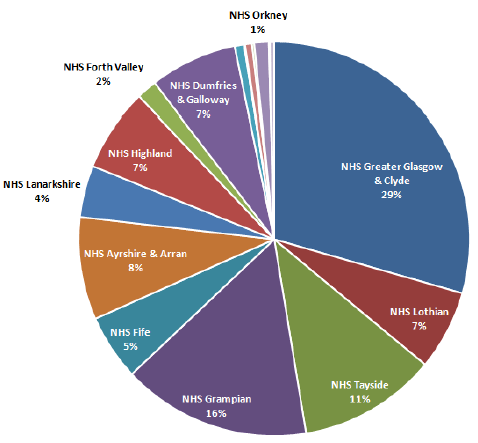
Note: the above chart includes all 22 NHS Boards and Special NHS Boards but those whose backlog is below 1% have not been separately identified for clarity of presentation reasons only.
Improved asset management practice introduced since 2010 requires that all identified backlog maintenance is risk assessed so that appropriate mitigation actions can be implemented and maintenance activity can be logically planned and prioritised. This provides the necessary governance arrangements to enable the expected life of property elements to be extended and backlog to be managed in a safe and financially sustainable manner.
The total backlog in the estate has been risk assessed and the results of this are shown in the chart that follows.
Backlog Maintenance Risk Profile
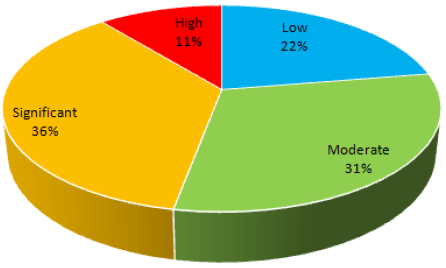
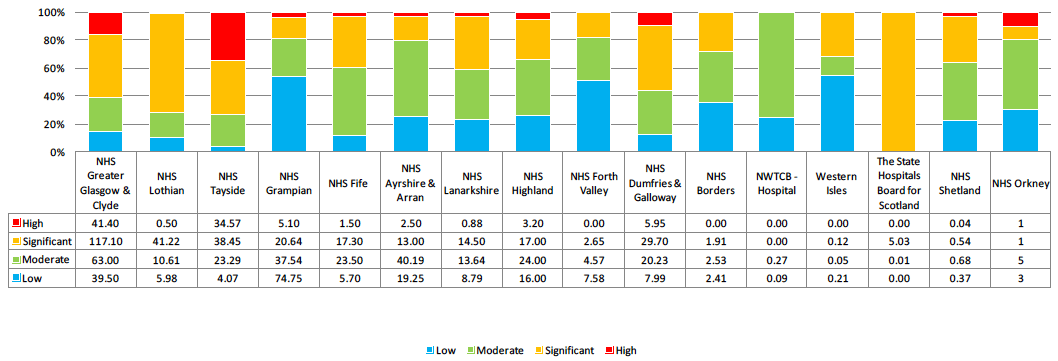
The proportion of Significant and High risk backlog maintenance has increased from 44% reported in 2015 to 47% reported this year. This is mainly attributable to the increase in Significant and High risk backlog reported by NHS Tayside (as discussed above). Most other Boards have either maintained or improved on this indicator which demonstrates that they are continuing to address this issue.
NHS Boards are continuing to review their current risk assessments to ensure that they appropriately reflect the level of risk to service and business continuity once adequate mitigation actions have been introduced to manage these risks. This has the potential of reducing the current risk profile of outstanding backlog maintenance.
The variation in risk profile across the different NHS Boards is highlighted in the following table:
2016 Backlog Maintenance Risk Profile - NHS Boards
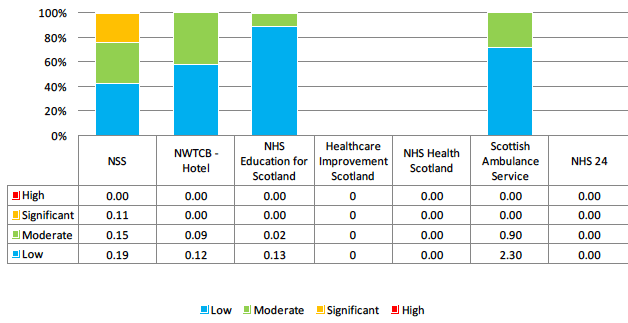
2016 Backlog Maintenance Risk Profile - Special Health Boards
Although backlog is identified as an expenditure requirement, in practice it is likely to be addressed by a combination of:
- Estate rationalisation and disposal of older properties avoiding the need for expenditure on backlog. The scope of planned disposals over the next 5 years is outlined in Section 3.
- Replacing older properties with new facilities and avoiding the need for expenditure on backlog e.g. the estate rationalisation following the completion of the Queen Elizabeth University Hospital in Glasgow and further estate rationalisation once the new hospital replacement projects are completed in Dumfries and Orkney.
- Incorporating backlog works within major redevelopment, modernisation and refurbishment projects.
- Undertaking specific projects to target the high and significant backlog.
- Incorporating backlog work within operational repair and cyclical maintenance.
These strategies have been used to reduce the backlog maintenance expenditure requirement since a total figure of £1,010m was first reported in the 2011 SAFR. The following table provides a summary of the progress that NHS Boards have made in reducing this backlog between 2011 and 2016 (i.e. excluding inflationary cost adjustments and any additional newly reported backlog in that period):
| SAFR Reporting Year | Change to backlog costs since originally reported in 2011 SAFR (£m) |
|---|---|
| 2011 | 1010 |
| 2012 | 911 |
| 2013 | 803 |
| 2014 | 702 |
| 2015 | 655 |
| 2016 | 584 |
The table shows that NHSScotland has been able to successfully reduce the backlog maintenance expenditure requirement identified in 2011 by £426m to a current total of £584m in 2016. However, as identified earlier, the total backlog expenditure requirement reported by Boards in 2016 is £887 million which takes account of the impact of inflation on maintenance costs as well as additional newly identified backlog over the same period. Hence, the backlog reported by Boards in any one year is a total figure which incorporates both the impact of their investment to reduce the backlog identified in previous years and any new backlog and cost adjustments identified within the year.
It should also be recognised that newly identified backlog in buildings and engineering systems is an inevitable consequence of aging buildings that occurs as a result of:
- Building and engineering elements coming to the end of their operational life, which can vary significantly depending on the element - engineering components and systems can have relatively short operational lives with most requiring replacement within 20 years whereas building elements tend toward longer operational lives of up to 60 years.
- Variations in normal day to day operational usage which can result in shorter than expected operational lives of elements and in some cases unpredicted failure of systems and the need for earlier than expected replacement.
The following chart uses the original backlog figure reported in the 2011 SAFR to track the actual annual change in this backlog (i.e. excluding the impact of newly reported backlog or inflation) up to 2015/16, and then plots the future reductions needed to meet the aspirational target of reducing this total to below £500m by 2020 with no outstanding High risk backlog maintenance:
Past and Projected Backlog Maintenance Expenditure Requirement (excluding new backlog & inflation)
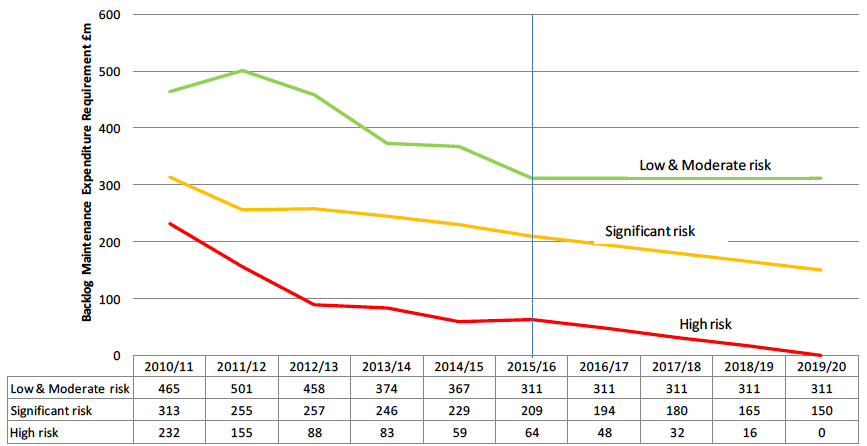
* excluding newly reported backlog & inflation
The chart shows that the reductions in backlog this year (2015/16) is generally in line with that forecast necessary to achieve the aspirational target for 2019/20. However, continued focus will be needed if NHS Boards are to eliminate all High risk backlog within that period. Also, in future years the growing level of new backlog will need to be incorporated into property improvement plans.
It is recognised that in practice new build and refurbishment / upgrade schemes will inevitably reduce all categories of risk assessed backlog when, for instance, this backlog is in the same building/area in which the high and significant risk backlog is present; hence, it is accepted that some reduction in low and moderate risk backlog will continue to take place in parallel with the reductions in high and significant risk backlog and is a practical consequence of undertaking improvement works in buildings.
Whilst this analysis and projections of future backlog provides a high level indication of how backlog might be reduced over the next few years, it needs to be recognised that in practice it is very difficult to accurately project changes in backlog in existing buildings, and timings for estate rationalisation can be influenced by a number of factors including operational priorities and market forces (in relation to disposals).
1.4.4 Asset Performance for Office Accommodation
The NHSScotland Smarter Offices Programme was established in October 2013 with the aim of supporting improved utilisation of office accommodation across the NHS estate by supporting NHS Boards and Special Boards in the development of a strategic approach to their office accommodation. This expected to gain the following benefits:
- Provision of affordable support accommodation to the NHS that is better able to respond to future changes in strategic direction
- Improved quality of working environment which facilitates the retention and recruitment of staff
- Improved availability of staff welfare facilities promoting positive staff morale.
- Flexible, well designed, efficient space that is able to cope with uncertainty around future property needs, support opportunities to change working practices, and introduce new technology
- Supporting Scottish Government environmental sustainability agendas through the appropriate procurement, design and operation of its property assets.
- Maximised opportunities for staff to develop and deploy their knowledge, skills and personal qualities creatively to add value to the organisation.
- More integrated/collaborative working and thereby encourage better use of skills and resources.
- Synergies from shared use of accommodation and support services.
By drawing on wider research undertaken by UK Government, the Programme has developed a set of performance measures covering workplace standards and benchmarks which this report has adopted as the Office Performance Framework. This includes setting a benchmark of 8sq.m. per Whole Time Equivalent ( WTE) (i.e. space per person) for new and refurbished office space and 10sq.m. per WTE for all other office accommodation. It also includes a Desk to WTE of 80% (i.e. desks per person).
The tables over the page show NHS Boards' position in relation to these benchmarks, as well as the annual change in costs associated with this accommodation type. For territorial health boards the space standards have improved over the last 12 months with the space per WTE changing from 14.5 sq.m. to 12.7 sq.m., and the desk to WTE ratio changing from 104% to 98%. Variance across Boards suggests scope for even further improvement in these indicators. Across all NHS Boards, the total occupancy cost per net internal area has reduced slightly from £194 to £190 per sq.m. Each of these indicators suggests that NHS Boards are improving the effective utilisation of this accommodation type but this will continue to be monitored to ensure ongoing cost effectiveness.
Contact
Email: Alan Morrison, Alan.Morrison@gov.scot
Phone: 0300 244 4000 – Central Enquiry Unit
The Scottish Government
St Andrew's House
Regent Road
Edinburgh
EH1 3DG
There is a problem
Thanks for your feedback