Developing a community child health service for the 21st century
A report on a review of the community child health service in Scotland.
Section 9: Scottish Association of Community Child Health/Royal College of Paediatrics and Child Health questionnaire 2010: summary of results
At the first meeting of the CCH21 Steering Group, Dr Helen Gibson, the SACCH representative, offered to undertake a questionnaire of all consultant paediatricians working in CCH in Scotland to ascertain their work patterns. With the permission of SACCH, the results of the survey are summarised here.
Methods
The RCPCH Scottish Office kindly circulated the survey to all consultant paediatricians in Scotland. Colleagues were asked to respond if they undertook one or more clinical sessions per week in traditional community paediatric disciplines. Prior to the survey SACCH estimated there to be about 40 consultant paediatricians working in CCH. The estimate was based on membership lists and the knowledge of committee members.
Results
There were 48 replies with 44 meeting the inclusion criteria. Only 32% of the group had a specific reference to "community" in their job title. Responders came from 10 of the 14 Health Boards in Scotland with 25.6% from Greater Glasgow and Clyde Health Board ( GGC) and 60.5% from GGC, Lothian and Grampian Health Boards.
Because of a noticeable diversity of answers it was decided to analyse the responses by the amount of CCH work undertaken. Responders divided into two groups:
- Group 1 - More than 75% of job plan in CCH (n=16)
- Group 2 - Less than 50% of job plan in CCH (n=11)
Although the sample was small the findings are useful. The groups differed substantially in their characteristics in relation to on-call, main place of work and patterns of work and between the type of service in which they worked. In GGC, Lothian and Grampian 90% of survey Consultants work more than 50% of the time in CCH roles compared with 21% in other Health Boards. 82% had intended to work in CCH specialties, 82% had over 6 months training in CCH, suggesting that better trained and motivated paediatricians are attracted to the major teaching centres' CCH services.
On-call Commitment by Group
There are significant differences between the two groups in terms of on-call commitments, with Group 1 ( CCH duties dominant) doing child protection on-call, and Group 2 (integrated model) doing more general (acute) on-call and less child protection on-call. The newer consultants' job plans (delivering CCH in an integrated fashion) provide general acute paediatrics on-call. The future sustainability of separate child protection on-call rotas is doubtful.
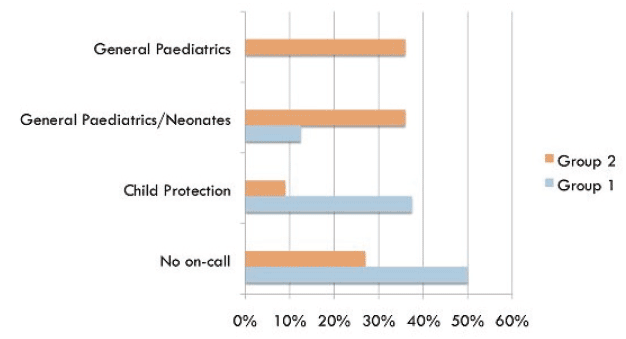
Main Place of Work by Group
Overwhelmingly Group 2 were based in DGHs. Group 1 were in various community settings. Responders in Group 1 were drawn mainly from large urban centres (Lothian, GGC and Aberdeen) versus Group 2 consultants whose job plans may have been created to sustain acute rotas in DGHs.
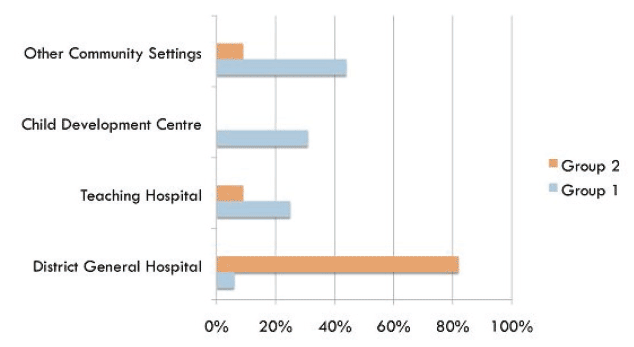
Pattern of Work
Examining the CCH component of responders' work, 93.8% of the Group 1 consultants understand neuro-developmental work and 43.8% worked in four or more CCH areas of work (eg adoption and fostering, sensory impairment, child protection, behavioural paediatrics etc.).
Amongst the integrated consultants (Group 2), 55.6% undertook eurodevelopmental work but 27.3% stated they had no dedicated sessions in CCH. It has to be assumed that these consultants are undertaking CCH duties as part of their general paediatric commitment and the skills and competencies are not considered to be specific to CCH.
Dr Gibson highlights the following comments from three Group 2 (Integrated) consultants:
"I … see many children with problems traditionally CCH (mainly neurodevelopmental and elimination disorders), referred directly to the General Outpatient service."
" CCH work was and is an automatic part of general paediatrician's duties."
"I do not think of my child protection duties as CCH."
When asked about pressures on their CCH practice the consultants responded as follows:
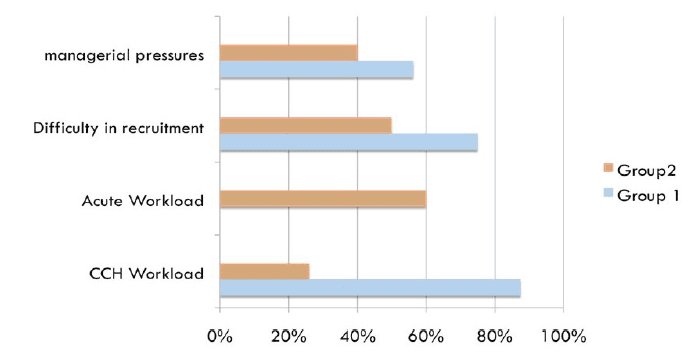
Comment on CCH Pressures
"I am employed for 8 sessions, but regularly work 12-14. My referrals have increased 5-fold and the complexity has increased significantly. I could not possibly take on acute commitment in addition."
In terms of the consultants' original career intentions:
- 73.3% of the whole group had intended to work in CCH as a consultant
- 100% of group 1 had intended to work in CCH as a consultant
- 14.3% of group 2 had intended to work in CCH as a consultant
- 20.5% of the survey had previously worked as Non-Consultant Career Grade Paediatricians
These replies indicate that a number of the consultants in Group 2 (integrated model) find themselves undertaking CCH duties even although they never intended to do so.
Previous Training in CCH
Responses about previous training in CCH showed about 30% of Group 2 had had only core training in CCH and 30% no training at all . Of Group 1, 55% had had more than 2 years. This finding concurs with the findings of the ST survey. 60
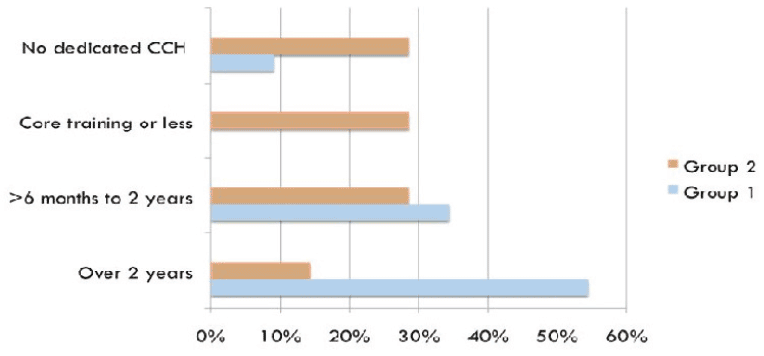
Summary of Survey Findings
Dr Gibson showed two predominant models of Consultant work in CCH in Scotland - the Group 1 the "traditional" model - working predominantly in CCH in community settings, covering a number of CCH specialties and the Group 2 an "integrated" model - with the majority of their workload in general paediatrics.
The integrated model (Group 2) was mainly based in DGHs where consultants had less specific CCH training and original intention to work in CCH. Consultants describe acute paediatric workload stresses and problems in recruitment of doctors with community expertise as their main pressures.
The traditional model (Group 1) consultants emphasise their greater training and expertise in CCH. Their work was community-based with a tradition of multi-agency and multidisciplinary team working. However, significant pressures in CCH workload have arisen from increased referrals and greater complexity.
Author's Comment on SACCH Findings
This study confirms that workforce challenges are driving the consultant model in DGH settings towards combining general paediatric and CCH duties. There remain concerns about the competency and skills in CCH of these general paediatricians, especially in leadership and advocacy for the smaller subspecialties of CCH such as the care of Looked After and Accommodated Children and Young People.
Contact
- Mary Sloan mary.sloan@gov.scot
There is a problem
Thanks for your feedback