Evaluation of Working Health Services Scotland, 2010-2014
The Working Health Services Scotland (WHSS) was introduced to provide support to employees in small and medium sized businesses', whose health condition was affecting their ability to work.
The programme offers telephone based case management & some fac
3 Service provision by Boards
3.1 Overview of models
The way that WHSS was implemented varied between the participating Boards, and in some cases varied over time with staffing changes. A broad overview of the staffing and models of implementation is given in Table 9. It should be noted that these arrangements were not fixed and consistent over the duration of the WHSS evaluation period, so variations across the years are not fully represented. The case management function was either in-house (by an individual or a team, and the case manager may have also been a therapy provider) or contracted to Salus (where case managers were not also therapy providers). Therapy provision (physiotherapy, counselling / psychological services and occupational therapy) could be provided from within an in-house WHSS team, provided from within the NHS therapy teams, or contracted out to private practitioners. Boards that contracted their therapy provision to external providers were responsible for ensuring that the service provided was occupationally / vocationally focussed.
The models can be summarised as:
A. In-house multidisciplinary team who deliver the case management and interventions - Borders, Dundee & Tayside, Fife, Forth Valley, Lothian.
B. In-house case management with all interventions delivered by external contractors - Greater Glasgow & Clyde, Highland, Lanarkshire.
C. In-house case management with interventions delivered through a mix of external contractors and local NHS arrangements - Ayrshire & Arran, Dumfries & Galloway, and Grampian.
Note that during the course of the programme Highland and Greater Glasgow & Clyde changed from having an in-house case manager to their case management being provided through Salus ( NHS Lanarkshire).
There are also significant differences between the Board areas in terms of populations and geographical coverage (and therefore ease of access for clients to get to therapy providers). It is therefore difficult to directly compare service delivery between the Boards.
In the subsequent tables and figures, the following abbreviations are used:
| A&A | Ayrshire and Arran |
| BD | Borders |
| D&G | Dumfries & Galloway |
| D&T | Dundee and Tayside |
| FF | Fife |
| FV | Forth Valley |
| GGC | Greater Glasgow and Clyde |
| GP | Grampian |
| HL | Highland |
| LK | Lanarkshire |
| LT |
Lothian |
Table 9: Board arrangements for service provision
| Model |
Case Manager ( CM) |
Physiotherapy |
Counsellor |
Occupational Therapy |
Other services |
Comments |
|||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| Part of core team |
Sessions from NHS |
External Contract |
Part of core team |
Sessions from NHS |
External Contract |
Part of core team |
Sessions from NHS |
External Contract |
|||||
| Ayrshire & Arran |
C |
1 CM |
Yes |
Yes |
Yes |
Admin |
Physio is transferred to mainstream if need on-going |
||||||
| Borders |
A |
1 CM |
Yes |
Yes |
For some of program |
Admin |
|||||||
| Dumfries & Galloway |
C |
1 CM |
Yes |
Yes |
Yes |
Admin |
|||||||
| Dundee & Tayside |
A |
Team |
Yes |
Yes |
Yes |
||||||||
| Fife |
A |
1 CM |
Yes |
Yes |
Yes |
OH Nurse |
|||||||
| Forth Valley |
A |
1 CM |
Yes |
Yes |
Yes |
||||||||
| Greater Glasgow & Clyde |
B |
1 CM / Salus |
Yes |
Yes |
None |
Initially own CM & used external contractors; Salus delivery from 2012. |
|||||||
| Grampian |
C |
1 CM |
Yes |
Yes |
None |
Counselling mainly via NHS 24 Living Lives |
|||||||
| Highland |
B |
1 CM / Salus |
Yes |
Yes |
None |
Initially own CM; Salus delivery from 2013. |
|||||||
| Lanarkshire |
B |
Salus |
Yes |
Yes |
Yes |
Admin |
|||||||
| Lothian |
A |
Team |
Yes |
Yes |
Yes |
Admin, welfare & employment rights advice |
Previously had a counsellor within the team |
||||||
3.2 Cases' primary health condition, by Board
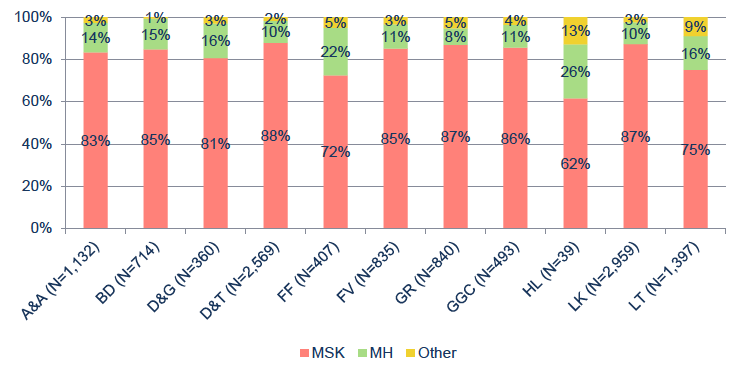
The primary health condition of cases is shown for each Board in Figure 11; this was collected at the entry assessment. Fife and Highland have the greatest proportion of cases with mental health conditions, although the numbers are very small in Highland. Differing proportions between Boards may be related to the way the services are marketed or managed in these areas.
Figure 11: Proportion of cases with different primary health conditions by Board
3.3 Absence status at entry
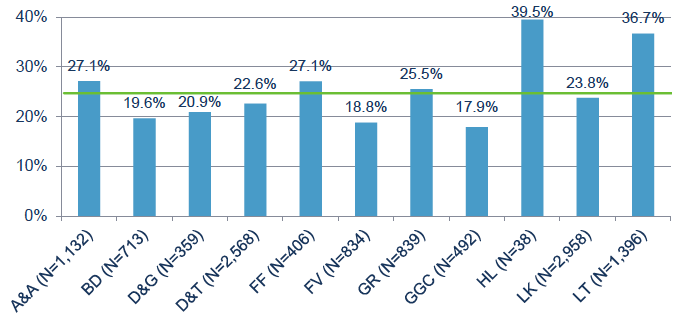
The absence status at entry assessment for cases in the different Board areas are shown in Figure 12, with the green line showing the average figure (24.7%, N=11,735). Boards which had a greater proportion of cases entering who were absent include Highland (although the numbers are very low), Lothian, Ayrshire & Arran, Fife and Grampian.
Figure 12: Proportion of cases who were absent at entry assessment, by Board. The average for all cases is shown (green line, N=11,735).
3.4 Completion of programme
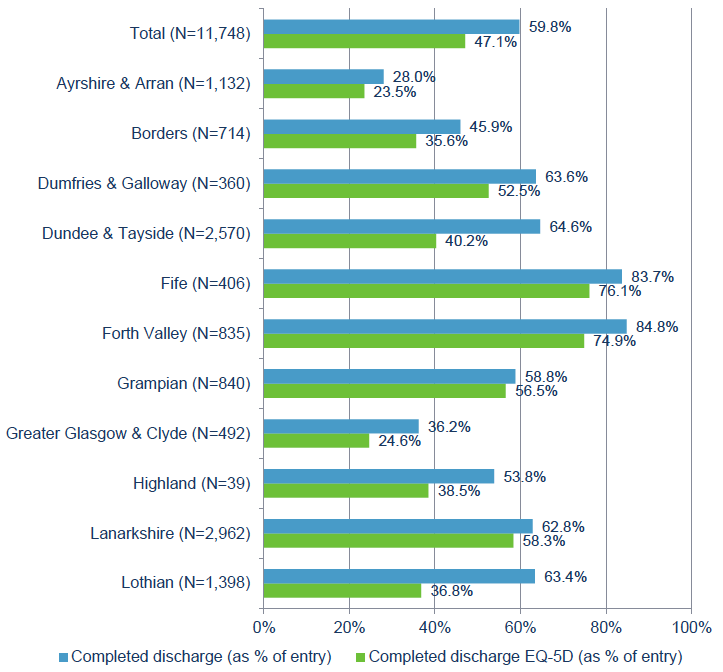
There were differences in the full completion of discharge paperwork between Boards (Figure 13). Completion of the discharge paperwork is classified in two ways: those who completed at least some of the discharge paperwork ('Completed discharge'); and those who completed the discharge EQ-5D ('Completed discharge EQ-5D', i.e. provided a more complete set of the discharge paperwork for the case - this is a subset of the group who 'completed discharge'). The percentages shown are of the number of cases who completed the entry assessment (i.e. were eligible for the service). For example, some discharge paperwork was received for 28% of cases that entered the Ayrshire and Arran programme, 36% of Greater Glasgow and Clyde, and 46% of Borders, with Fife and Forth Valley completing paperwork for 84% and 85% of their cases respectively. Reasons for this may relate to resources or to staffing issues. It is therefore difficult to compare the effectiveness of the service provision in different Boards.
Figure 13: Proportion of cases from each Board who completed the discharge paperwork and EQ-5D
3.5 Duration in the programme
The average duration of time that cases were in the programme varies between Boards. Figure 14 shows the average and standard deviation (error bars) of duration in the programme for those who completed at least some of the discharge paperwork.
Figure 14: Average duration of time that cases were in the programme, by Board, for those who completed the discharge paperwork
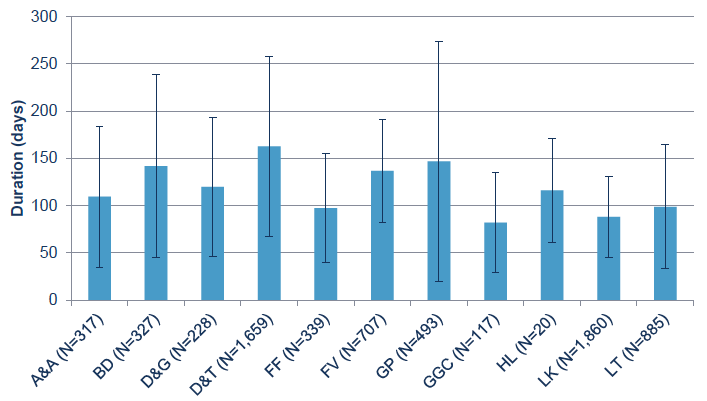
The longest average durations are seen for Dundee and Tayside (163 days), Grampian (147 days), Borders (142 days) and Forth Valley (127 days). The shortest durations are seen at Greater Glasgow and Clyde (82 days) and Lanarkshire (88 days). The average for all these cases is 121 days ( SD 81.6).
3.6 Service delivery
Because significant amounts of data are missing from some Boards, care should be taken when considering the differences in service delivery between them. However, the data which are available are summarised in Table 10, showing the number of cases that received that service, and the average and maximum number of sessions attended by a case. Note the N value is the number of cases for whom there were data showing that they had been offered at least 1 therapy session (i.e. those recorded as being offered no sessions, or where these data are missing, are excluded). No comment can be made about the suitability of the amount or duration of service provision as details on the differences in the needs of cases are not known.
The average number of therapy sessions provided by Board is also shown for physiotherapy (Figure 15), counselling / CBT / psychology services (Figure 17) and occupational therapy (Figure 19).
The average duration of time that cases were in the therapeutic services is shown by Board for physiotherapy (Figure 16), counselling / CBT / psychology services (Figure 18) and occupational therapy (Figure 20). The duration in the therapeutic service excludes cases that are recorded as having their first therapy service provision before the enrolment assessment, and those for whom the discharge from the therapy service is before the first appointment with the therapy service; these are considered to be recording errors.
Table 10: Service provision by Board
| Board |
Model |
Physiotherapy |
Counselling |
Occupational Therapy ( OT) |
||||||
|---|---|---|---|---|---|---|---|---|---|---|
| N |
Mean no. of app'ts attended |
Max no. of app'ts attended |
N |
Mean no. of app'ts attended |
Max no. of app'ts attended |
N |
Mean no. of app'ts attended |
Max no. of app'ts attended |
||
| A&A |
C |
916 |
3.4 |
12 |
191 |
4.0 |
12 |
17 |
1.1 |
2 |
| BD |
A |
365 |
3.6 |
14 |
92 |
5.0 |
24 |
117 |
1.9 |
15 |
| D&G |
C |
255 |
3.3 |
12 |
64 |
4.5 |
16 |
No data |
||
| D&T |
A |
2,208 |
4.1 |
24 |
246 |
4.9 |
18 |
343 |
1.9 |
16 |
| FF |
A |
255 |
4.2 |
10 |
85 |
5.2 |
12 |
47 |
1.0 |
1 |
| FV |
A |
694 |
3.7 |
13 |
59 |
3.7 |
9 |
15 |
1.4 |
3 |
| GGC |
B |
203 |
3.9 |
6 |
14 |
2.6 |
5 |
No data |
||
| GP |
C |
532 |
5.3 |
22 |
56 |
5.0 |
12 |
No data |
||
| HL |
B |
No data |
No data |
No data |
||||||
| LK |
B |
2,249 |
4.2 |
12 |
229 |
3.9 |
8 |
7 |
1.0 |
1 |
| LT |
A |
860 |
2.8 |
11 |
116 |
4.5 |
17 |
420 |
2.7 |
19 |
It is worth noting that Lothian WHSS provision is an occupational therapy managed service which may account for the higher number of cases receiving occupational therapy compared with other Boards (Figure 20).
Figure 15: Average number of physiotherapy sessions attended by cases by Board. The error bars show one standard deviation.
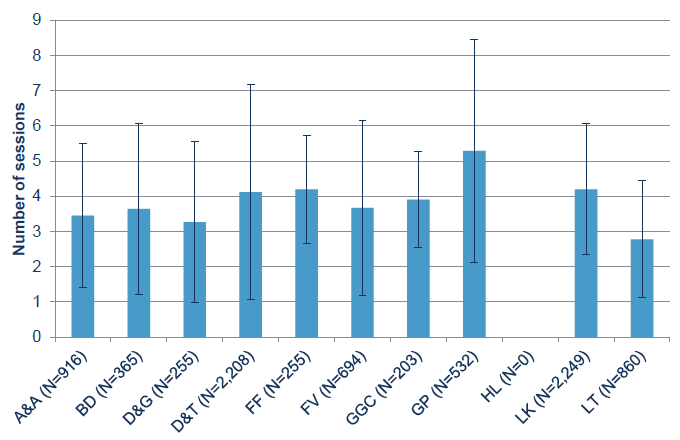
Figure 16: Average duration of time that cases were in physiotherapy service by Board. The error bars show one standard deviation.
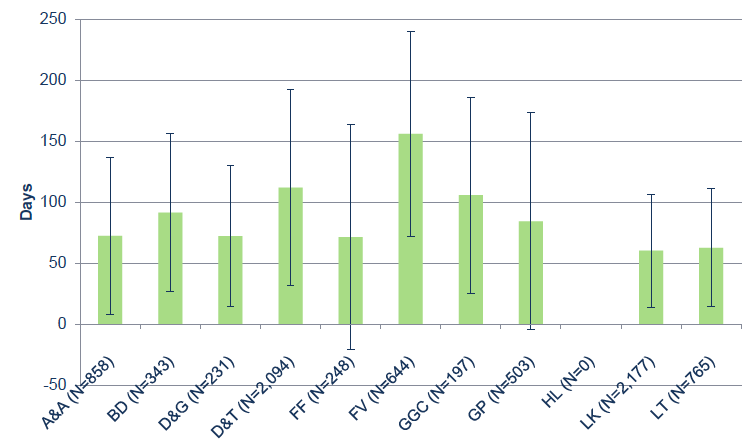
Figure 17: Average number of counselling / CBT / psychology sessions attended by cases by Board. The error bars show one standard deviation.
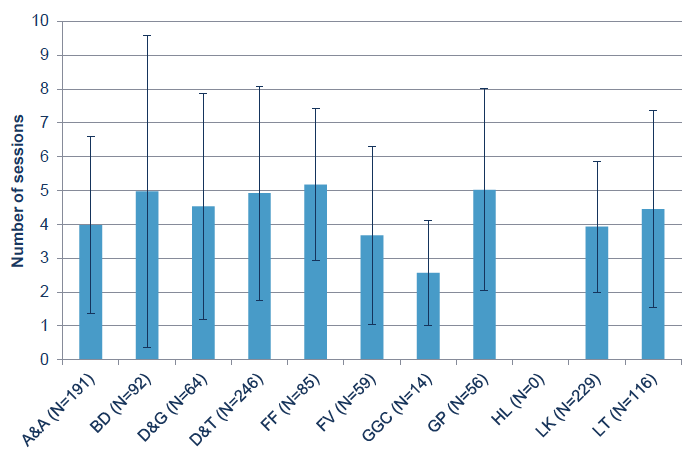
Figure 18: Average duration of time that cases were in counselling / CBT / psychology service by Board. The error bars show one standard deviation.
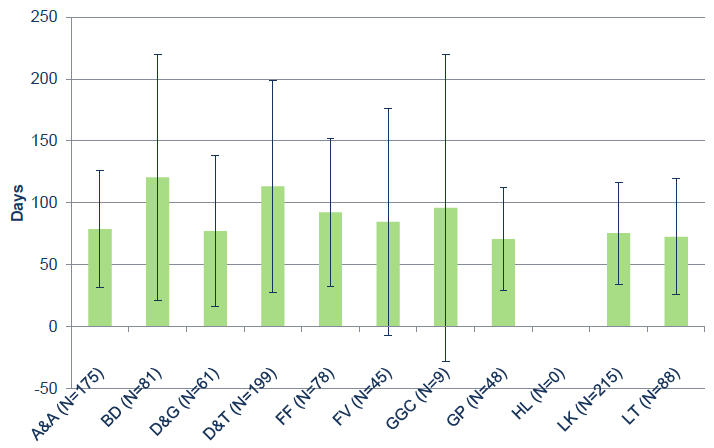
Figure 19: Average number of occupational therapy sessions attended by cases by Board. The error bars show one standard deviation.
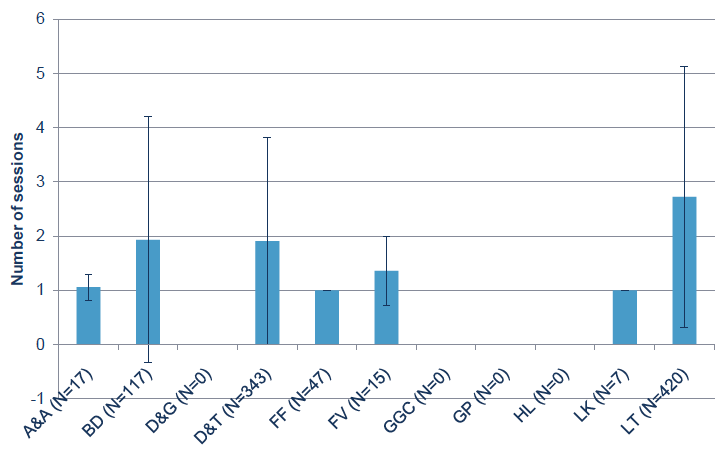
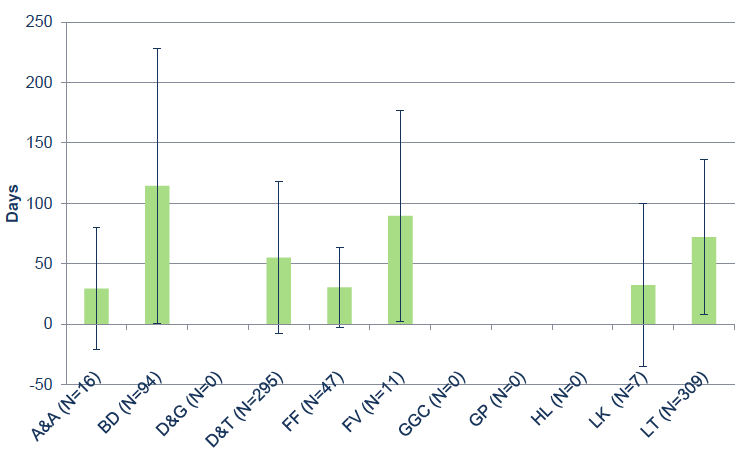
Figure 20: Average duration of time that cases were in occupational therapy service by Board. The error bars show one standard deviation.
Contact
There is a problem
Thanks for your feedback