Scottish Out-of-Hospital Cardiac Arrest data linkage project: initial results
This report presents the initial results of the Scottish Out-of-Hospital Cardiac Arrest data linkage project (OHCA data linkage project).
Survival following OHCA
Survival figures for OHCA where resuscitation was attempted are shown in table 2. The percentage of patients alive at 24 hours, 30 days and 1 year is given. In addition, return of spontaneous circulation ( ROSC) is an outcome measure frequently reported in other OHCA registries and publications and therefore we have included it here for comparison. Definitions for ROSC vary. The Scottish Ambulance Service record ROSC if a patient regains a palpable pulse which is sustained until arrival at the Emergency Department, a proxy for the Utstein definition of 'sustained ROSC' (palpable pulse for greater than 20 minutes).
Table 2 shows survival figures after OHCA in Scotland based on two different sets of assumptions in analysis of the data. In column A, we have used only patients where data could be linked (ie around 75%) in the denominator, yielding an overall 30 day survival of 8.4%. For the column B, the assumption has been made that patients who were not part of the linked dataset died shortly after their OHCA, which gives a lower 30-day survival figure of 6.2%. The presupposition here is that patients pronounced dead in the community without being transported to hospital are more likely to have insufficient data recorded for probabilistic data linkage ( see the methodology section for further information). The actual 30-day survival percentage will lie between the two figures, but is probably closer to that reported in column B.
Table 2: Outcomes after OHCA
| Outcome | A: Proportion based on linked dataset as denominator (%) | B: Proportion using all arrests as denominator and assumption that insufficient data for linkage = death (%) |
|---|---|---|
| ROSC | 16.7 | 12.2 |
| Alive at 24hrs | 12.7 | 9.3 |
| Alive at 30 days | 8.4 | 6.2 |
| Alive at 1 year | 8.0 | 5.9 |
In line with other published reports, 30-day survival is used as a proxy for survival to discharge from hospital. Detailed data for hospital discharges will be available for analysis in the future.
In the dataset, just over 800 (8.6%) cases fulfilled criteria for inclusion in the 'Utstein comparator group' meaning that the OHCA cases are witnessed, presented with a shockable presenting heart rhythm and bystander CPR was started. The 30 day survival in this group was 23.2%, substantially higher than for the whole cohort. The international literature reports survival to hospital discharge in this group between 18.5% and 52% [1], [33], [42].
Comparison of Scotland's survival rates with other registries
The results of the EuReCa ONE project were mentioned earlier - this project demonstrated significant differences in the incidence of OHCA, and also survival rates across Europe. The percentage who had ROSC among the 27 included countries ranged from less than 10% to over 40%. The percentage with ROSC in Scotland is at the lower end of this spectrum. Similarly, our 30-day survival sitting between 6.2% - 8.4% (see Table 2) puts Scotland among the countries with the lowest survival rates, lower than the overall European survival rate of 10.3% reported by EuReCa ONE. Substantially higher 30 day survival rates are found in Finland, the Netherlands and Switzerland [11], [43]. Comparable proportions of people who survived 30 days were found in Denmark and other parts of the United Kingdom [17], [19]. It is important to reflect on these differences in the context of the different population included in different datasets (eg some studies or registries only include OHCA cases with a cardiac origin, while others include cases with other aetiologies such as drugs-related cases or cases due to trauma, some report only witnessed OHCA cases, and others also include unwitnessed cases), and the differences in data collection and data processing (eg handling of missing data) [15] . The EuReCa ONE project collaborators themselves also identified sources of variability in data processing and collection.
Using logistic regression to make like-for-like comparisons
In addition to overall survival figures we have made a series of comparisons of OHCA survival between different groups using logistic regression techniques. This makes it possible to adjust for factors - for example age, sex and deprivation - that might differ between sub-groups and confound any associations. Logistic regression techniques adjust for these factors enabling us to make like-for-like comparisons.
The results of this type of modelling should be interpreted as relative measures. For example when the survival between males and females is compared using logistic regression, the risk of death for males is used as the reference category and the estimated risk for females is expressed relative to that of males.
(Technical note: we recognise that odds ratios over-estimate relative risks when outcomes are common, ie occur in greater than 15% of the study population [44] . For accessibility, the results here are described in terms of higher and lower risk but are actually calculated as higher and lower odds. We plan further analysis to compare the results of both approaches [45] . Using logistic regression models is in line with the majority of published papers in this research field thus enabling comparisons.)
Effect of age and sex on survival of OHCA patients
The previous section showed that overall, males in the cohort are more likely than females to be affected by an OHCA. In contrast, the percentage of females who survive after an OHCA is lower compared to males (see Figure 8, crude analysis). More detailed analysis of our data have shown that women are more likely to present with a less favourable heart rhythm (non-shockable). In the linked dataset, the proportion with shockable presenting heart rhythm was 17.5% among females and 29.8% among males. The adjusted analysis presented in Figure 8 show that taking these differences, and differences in age distribution into account (adjusted analysis), there is no longer any sex difference in survival. This finding is in line with other published work [46] .
Figure 8: Results of logistic regression analysis examining the effect of sex on risk of death at 30 days after OHCA. The diamonds refer to the estimated odds ratios for 30 days mortality and the bars refer to the 95% confidence intervals. Males are the reference category. Values above 1 for the lower limit of the confidence interval suggest a statistically significant higher risk for 30 days mortality for women in the crude estimates that is not observed for the adjusted estimates.
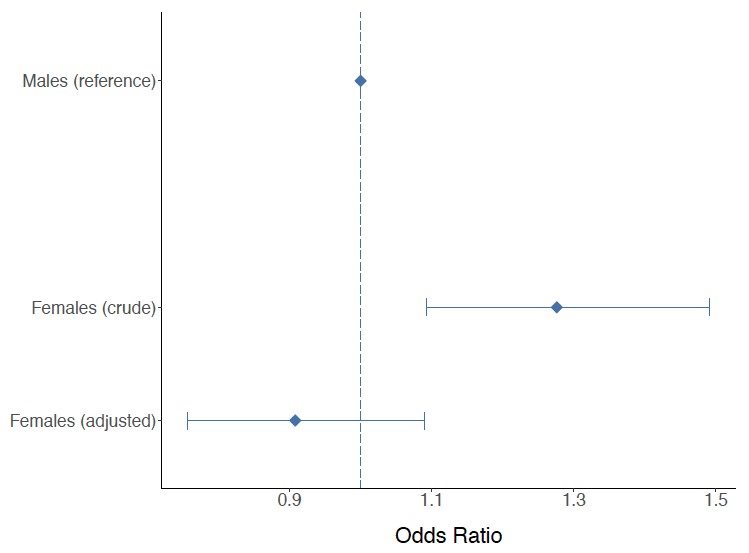
In Figure 8, the crude data shows that a higher proportion of females die within 30 days of their OHCA. However the sex difference is no longer present after adjusting for age and presenting heart rhythm as illustrated by the fact that the 95% confidence intervals include the value of 1.
Figure 9: Results of logistic regression analysis examining the effect of age on risk of death at 30 days after OHCA. The age group <45 years is the reference category. The diamonds refer to the estimated odds ratios for 30 days mortality and the bars refer to the 95% confidence intervals. Values above 1 for the lower limit of the confidence intervals for the age groups 65-75 and >75 suggest a statistically significant higher risk for 30 days mortality patients older than 65 years compared with patients younger than 45 years. The adjusted analysis is adjusted for sex.
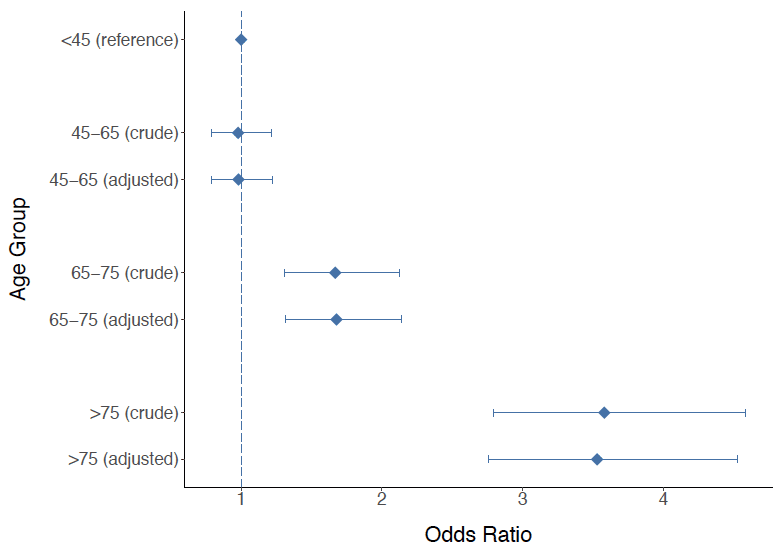
In Figure 9, both the crude and adjusted analysis show that patients from 65 years and older are more likely to die within 30 days after their OHCA compared with younger patients. This finding is consistent with other published figures [46] .
Effect of SIMD status on survival of OHCA patients
Figure 3 has already shown that people living in more deprived areas are more likely to experience an OHCA. Further analysis show that patients from deprived areas are also less likely to survive following OHCA. Figure 10 shows the likelihood of 30 day survival for each of the first four quintiles of SIMD compared with people from the least deprived areas ( SIMD5). People who lived in the most deprived areas of Scotland ( SIMD1) are 43% more likely to die within 30 days after their OHCA compared with people who lived in the least deprived areas in Scotland ( SIMD5).
Figure 10: Results of logistic regression analysis examining the effect of SIMD quintiles on risk of death at 30 days after OHCA. SIMD5 (least deprived) is the reference category. The diamonds refer to the estimated odds ratios for 30 days mortality and the bars refer to the 95% confidence intervals. Values above 1 for the lower limit of the confidence intervals for SIMD1 suggest a statistically significant higher risk for 30 days mortality for patients in SIMD1 compared with patients from the least deprived areas. The adjusted analysis is adjusted for sex, age and urban rural classification.
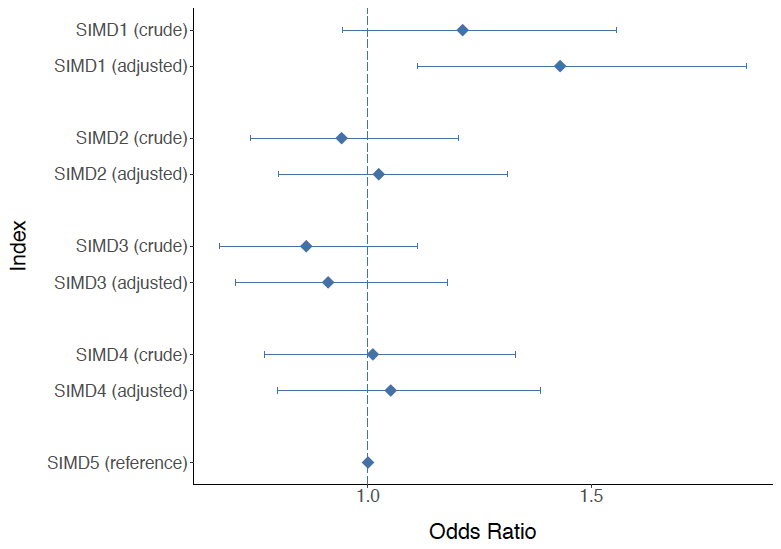
Figure 10 shows that in both the crude and adjusted analysis patients who lived in SIMD1 are more likely to die within 30 days after their OHCA compared with patients who lived in the least deprived areas.
The effect of SIMD on survival is most pronounced among males. Furthermore for both males and females the effect is greatest among younger patients (younger than 45 for females and younger than 65 for males). Our data appear to show that the effect of deprivation may be explained by less bystander CPR and higher likelihood of comorbidities among young OHCA patients living in SIMD1 areas compared with people of similar age from less deprived areas (these results are not shown here).
The underlying explanation of these SIMD-related differences will be multifactorial, but lifestyle factors such as smoking are likely to play a significant role [32], [47].
More in depth analysis focusing on the association between SIMD and the incidence and outcomes of OHCA are planned.
Effect of urban and rural environment on survival of OHCA patients
In Table 1, the incidences of OHCA are shown for the six urban rural categories [28] . Note, these percentages are based on only the patients in the linked dataset and are therefore subject to the caveats already stated. Patients from areas classified as remote accessible towns, large urban areas and other urban areas have the highest incidences of OHCA, and remote rural areas the lowest.
Given the small numbers in some groups, a dichotomous (two-category) urban-rural measure was created (Table 3) for the following analysis of differences in 30-day survival.
Table 3: Aggregation of urban and rural categories
| Six categories |
Two categories |
|---|---|
| Large urban areas |
Urban |
| Other urban areas |
Urban |
| Accessible small towns |
Rural |
| Remote small towns |
Rural |
| Accessible rural |
Rural |
| Remote rural |
Rural |
Figure 11: Results of logistic regression analysis examining the effect of living in urban or rural areas of Scotland on risk of death at 30 days after OHCA. Urban area is the reference category. The diamonds refer to the estimated odds ratios for 30 days mortality and the bars refer to the 95% confidence intervals. Values above 1 for the lower limit of the confidence intervals for rural category in the adjusted analysis suggest a statistically significant higher risk for 30 days mortality in patients who lived in rural areas compared with urban areas. The adjusted analysis is adjusted for sex, age and SIMD.
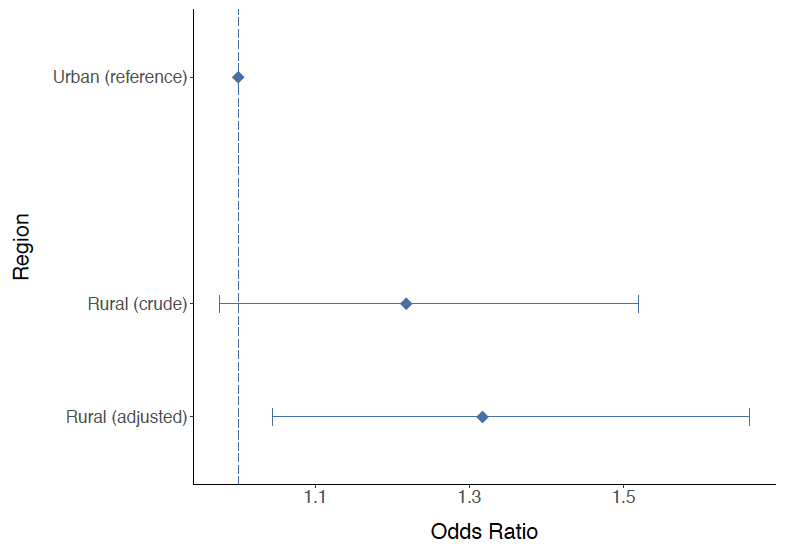
In Figure 11, the adjusted analysis shows that patients living in a rural area are more likely to have died 30 days after OHCA compared with patients living in an urban area.
People living in rural areas are less likely to survive an OHCA. The adjusted analysis shows that this effect persists after taking into account the age, sex and SIMD distributions. Further analysis will investigate the effect of other potential factors such as heart rhythm and bystander CPR.
Effect of Initial heart rhythm on survival of OHCA patients
As mentioned in the previous section, a shockable initial heart rhythm after OHCA is predictive of increased survival. Taking all patients with a known initial heart rhythm into account (91% of the total dataset), we found that people who present with a shockable initial heart rhythm are 88% more likely to survive until 30 days after the OHCA compared with patients with a non-shockable rhythm. These results are based on a logistic regression model adjusted for age and sex (adjusted odds ratio 0.12 (95% confidence interval 0.10-0.14, further adjustment for SIMD and urban rural category did not change the estimates).
Effect of bystander CPR on survival of OHCA patients
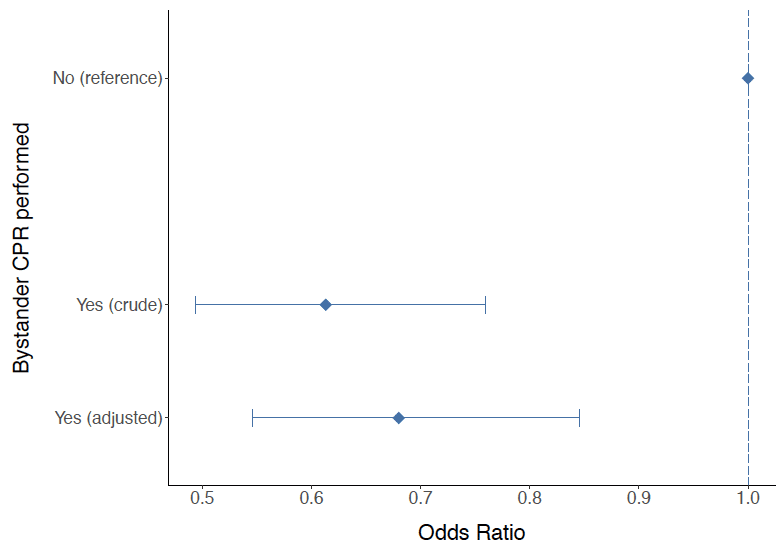
A positive effect of bystander CPR on survival was found in OHCA cases where the first ambulance arrived within eight minutes after one of the Ambulance Control Centres received an OHCA call. In figure 12, the likelihood of survival with and without bystander CPR is compared. This figure shows that on average, cases with bystander CPR are 32% more likely to be alive 30 days after the OHCA.
In Figure 12, both the crude and age, sex, SIMD and urban rural category adjusted analysis show that patients who receive bystander CPR are more likely to survive 30 days after OHCA compared with patients who do not receive bystander CPR.
As mentioned previously, we suspect that the available bystander CPR data is underreported. Therefore, it is likely that the true effect of bystander CPR on survival is even greater. Furthermore, not all CPR is equally effective. A limitation of the current available data is the lack of timing of the start of bystander CPR making it impossible to calculate how long before the arrival of the first ambulance a bystander started CPR. Chest compressions started earlier are likely to be more effective in preserving life than those started after a significant delay [35] .
Currently work is underway to solve some data issues for arrival times. Therefore, only cases where the first ambulance arrived within eight minutes are included in the current analysis.
Figure 12: Results of logistic regression analysis examining the effect of bystander CPR on death at 30 days after OHCA within all cases where an ambulance arrived within eight minutes. The group where bystander CPR was unknown is reported as the reference category. The diamonds refer to the estimated odds ratios for 30 days mortality and the bars refer to the 95% confidence intervals. Values above 1 for the lower limit of the confidence intervals for the Yes category in the crude and adjusted analysis suggest a statistically significant lower risk for 30 days mortality in patients who received bystander CPR compared with the group for which the bystander CPR status is missing or unknown. The adjusted analysis is adjusted for age, sex, SIMD and urban rural category.
Contact
There is a problem
Thanks for your feedback