Rare Disease Scotland: progress report
An update on the work carried out in Scotland against the 51 Commitments in the UK Strategy for Rare Diseases.
1. Empowering Those Affected By Rare Diseases (1 – 8)
| Commitment |
Description |
|---|---|
| 1 |
Strengthen the mechanisms and opportunities for meaningful and sustained patient involvement in rare disease service provision and research, recognising patient groups as key partners – including in the development of the four country plans to implement the Strategy. |
| 2 |
Improve awareness amongst service providers and others of the effects that rare diseases can have on a person’s education, family, social relationships and ability to work. |
| 3 |
Encourage effective and timely liaison between the NHS and other public service providers, and encourage providers to consider the effects of rare disease on people’s lives when they are developing and managing services. |
| 4 |
Make sure that patients and their families have a say in decisions about treatment and in the planning, evaluation and monitoring of services. |
| 5 |
Consider how to give all patients with rare disease clear and timely information about: their condition and its development; treatment and therapy options; practical support. |
| 6 |
Improve access for patients (or where appropriate their parents or guardians) to their personal data. |
| 7 |
Support patients to register on databases, where these exist. |
| 8 |
Help patients to contribute to research and other activity related to rare disease. |
The Scottish Government is fully committed to empowering people in terms of their health and social care. A number of plans, policies and recommendations have been made since the last biennial report that are being driven and delivered across Scotland. These will also directly impact on people who are affected by rare diseases. The plans and policies listed below give a brief explanation of the work that is progressing throughout Scotland.
1.1 The Rare Disease Implementation Oversight Group
The role of the Rare Disease Implementation Oversight Group is to monitor the implementation of the Scottish Rare Disease Plan ‘It’s Not Rare to Have a Rare Disease’ and to ensure that the 51 Commitments in the UK Strategy for Rare Disease are being met.
The group is made up of clinicians, geneticists, biochemists, as well as representatives from NHS National Services Scotland, Patient groups, NHS National Education Scotland, the Farr Institute and the Scottish Government.
1.2 Health & Social Care Delivery Plan
The Health and Social Care Delivery Plan [4] , published in December 2016, sets out the Scottish Government’s plans for enhancing health and social care services by 2021. The plan aims to focus on care being provided to the highest standards of quality and safety, whatever the setting, with the person at the centre of all decisions. The Audit Scotland report ‘ NHS in Scotland 2016’ [5] , underlined the importance of bringing together the different programmes of work to improve health and social care services.
Delivering the Plan
The plan seeks to build on the excellence of NHSScotland, recognising the critical role that services beyond the health sector must play and ensuring that it is ultimately fit for the challenges facing us as country. It focuses on three aims:
- Better care – “we will improve the quality of care for people by targeting investment at improving services, which will be organised and delivered to provide the best, most effective support for all”.
- Better health – “we will improve everyone’s health and wellbeing by promoting and supporting healthier lives from the earliest years, reducing health inequalities and adopting an approach based on anticipation, prevention and self-management”.
- Better value – “we will increase the value from, and financial sustainability of, care by making the most efficient and consistent delivery, ensuring that the balance of resource is spent where it achieves the most and focusing on prevention and early intervention.
One of the main principles of the plan is that individuals, and where appropriate, their families should be at the centre of any decisions that affect them. They should be given more freedom, choice, dignity and control over their care. Care planning should anticipate the individual’s health and care needs – both by helping those with chronic and other complex conditions to manage their needs more proactively.
There are a number of actions set out within the plan with a view to achieving the aims, below are a sample of examples.
- In 2017, the Scottish Government will ensure that Health and Social Care Partnerships ( NHS boards, local authorities and other care providers) make full use of their new powers and responsibilities to shift investment into community provision by reducing inappropriate use of hospital care and redesigning the shape of service provision across hospital, care home and community settings. This will be a key lever in shifting the focus of care across health and social care services.
- By 2018, the aim is to have increased health visitor numbers with a continued focus on early intervention for children through addressing needs identified through the Universal Health Visiting Pathway [6] , which started in 2016. As a result of this, every family will be offered a minimum of 11 home visits including three child health reviews by 2020, ensuring that children and their families are given the support they need.
- By 2021, the aim is to ensure that everyone who needs palliative care will get hospice, palliative or end of life care. All who would benefit from a ‘Key Information Summary’ [7] will receive one – these summaries bring together important information to support those with complex care needs or long-term conditions, such as future care plans and end of life preferences. More people will have the opportunity to develop their own personalised care and support plan. The availability of care options will be improved by doubling the palliative and end of life provision in the community, which will result in fewer people dying in a hospital setting.
- By 2021, the aim is to have strengthened the multi-disciplinary workforce across health services. We will have a refreshed role for district nurses by 2017, train an additional 500 advanced nurse practitioners by 2021 and create an additional 1,000 training places for nurses and midwives by 2021. This will build on four successive increases in student nursing and midwifery intakes to meet additional demand, especially in primary and community settings.
- By 2021, the aim is to have increased the number of undergraduates studying medicine by 250 as a result of the 50 additional places in Scotland’s medical schools introduced in 2016.
All the actions can be viewed in the plan at: http://www.gov.scot/Publications/2016/12/4275/downloads
The Health and Social Care Delivery Plan addresses Commitments 3, 4, 5 and part of 11 (see below) of the UK Strategy for Rare diseases. One of the most common themes in feedback responses from people with rare diseases and their carer/families is that it is very difficult joining up health and social care. This plan for Scotland will mean that the people with a rare disease will be central in the care planning process, with all elements of primary, secondary and social care involved in the journey and planning of care. It ensures that the person is at the centre of all the care and support they require, that they have a say in their care package and are given freedom, choice and say in the decisions that directly affect them.
1.3 Realistic Medicine
In 2016, the Chief Medical Officer’s annual report introduced the concept of “Realistic Medicine”, this highlights that decision making about an individual patient’s healthcare should be focused on the individual and discussed and agreed with them, their family/carer and the clinician. It is about providing people the treatment that is right for them at the right time with the right support. Its aims of reducing harm and waste, tackling unwarranted variation in care, managing clinical risk, and innovating to improve are essential to a well-functioning and sustainable NHS. Realistic Medicine is not about rationing healthcare; it is about changing the overall approach to healthcare.
The full report can be found at: http://www.gov.scot/Resource/0049/00492520.pdf
This was followed up in 2017 with ‘Realising Realistic Medicine’ [8] which talks about realising the vision of Realistic Medicine for the future – “By 2025, everyone who provides healthcare in Scotland will demonstrate their professionalism through the approaches, behaviours and attitudes of realistic medicine”.
Realistic Medicine addresses Commitment 1, 4 and 5 of the UK Strategy for Rare Diseases. It means that the person with a rare disease and/or their carer/family will have a direct say in their treatment, taking account of what is right for them and their circumstances. No-one should have decisions made about them without them having a say, and they should fully understand what will happen, what their treatment will be and how it will affect their life.
1.4 Making it Easy: A Health Literacy Plan for Scotland
In order for patients to feel empowered, they must have the knowledge, understanding, skills and confidence to use health information and be active partners in their care, they must be health literate. The Scottish Government is currently taking forward the ‘Making it Easy: A Health Literacy Action Plan for Scotland’ [9] in order to “make Scotland a health literate society that enables all of us to live (and die) well on our own terms and with any health condition we may have.” This has involved developing an online national literacy resource for Scotland (The Health Literacy Place [10] ), developing an e-learning module for NHS staff and establishing a national demonstrator site across NHS Tayside. Projects within NHS Tayside have included improving signage and navigation of the hospital environment, using simpler language in appointment letters and utilising the ‘teachback’ technique to check patient understanding. A progress report was published in July 2017 and a new Action Plan was published in December 2017 [11] .
This links in with the Scottish Government’s work in enacting the Patient Rights (Scotland) Act 2011 and in particular the legal right for patients to participate as fully as possible in decisions and to be given the necessary information, in a way they can understand, to allow this participation.
Health literacy addresses Commitments 3, 4 and 5 of the UK Strategy for Rare Diseases. It is very important for people with rare diseases and their carer/family members that they understand the condition, the effects, the treatment options available, what they entail and what the outcomes are. Additionally, those living with a rare disease often need to attend numerous appointments, therefore it is important that the person and carer/family member understand what the appointments are for and where the relevant clinic is. This should be a straight forward process that does not add further stress onto what can already be a stressful time for patients and families.
1.5 House of Care Model for Scotland
The House of Care Model for Scotland [12] , developed by the Scottish Government in partnership with The Health and Social Care Alliance Scotland [13] (The Alliance), provides a simple visual model of a house build around collaborative care planning conversations between people and their health care professionals. The care and planning conversations are at the centre of the house/model and are supported by aspects such as health literacy, ‘more than medicine’, committed multi-disciplinary teams of clinicians and effective organisational processes and arrangements.
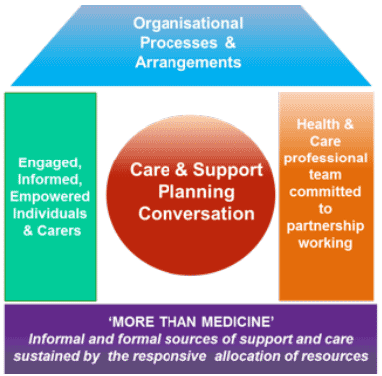
Building the House of Care requires the kind of whole-system transformation needed to recognise the assets, rights and capabilities of people, and place them in the driving seat of their care and support. The Scottish Government has provided £505,000 funding towards implementation of the House of Care model in addition to the £395,000 provided by the British Heart Foundation. The approach has been implemented within 55 GP practices across five adopter sites (Lothian, Glasgow, Tayside, Ayrshire & Arran and Lanarkshire).
The purpose of the care and support planning conversation itself is to empower the patient; it recognises that although healthcare professionals have knowledge and expertise about the clinical care of a condition, the person with the condition knows best how it impacts on their life. The focus should be on what matters to them rather than their condition or disease. It is a real opportunity for them to share information and openly discuss issues and concerns, as well as to get help with accessing the services and support they require to live with their disease or condition. Dr Sue Arnott, Clinical Lead on House of Care for NHS Lanarkshire states that House of Care “is a way to allow patients to have the opportunity just to become involved again, because they were used to having tests and tasks done and things measured, but when you actually get down to it there was very little opportunity for them to tell their story and I really felt that this was a way for them to do that”.
House of Care addresses Commitments 1, 2, 3, 4 and 5 of the UK Strategy for Rare Diseases. Very often a person with a rare disease and/or their carer/family member will become fully knowledgeable in the particular condition. House of Care recognises this and acknowledges that sometimes while clinicians will know about the care and treatment of the condition, the personal experience of the person with the rare disease is not always taken into account. House of Care will mean that the focus of discussion will be on what matters to the person, and will allow them to share information on what they know and have learned about the rare disease, and openly discuss their concerns, preferences and any issues. It should also help the person to access services and support that will help them to live with their rare disease.
1.6 What Matters to You?
In 2016, the Scottish Government and Healthcare Improvement Scotland ( HIS) formed a partnership with people who work in care to hold Scotland’s first ‘What Matters To You?’ [14] day on Monday 6 June 2016. ‘What Matters to You?’ day aims to encourage and support more meaningful conversations between people who provide health and social care and the people, families and carers who receive health and social care. This has now become an international movement with many countries around the world participating.
The ‘What Matters to You?’ approach goes beyond health and social care, reaching many other parts of the public sector that impact directly on people’s health and wellbeing. In 2017, schools, child minders, housing associations and other parts of the public and the third sector in Scotland, all signed up and participated.
By talking to the people they are caring for about what’s important to them, listening to the answers and taking action on what they hear, staff can provide the care and support that people really need and want.
The aim of the Scottish Government and HIS is that this becomes an on-going conversation, taking place every day in health and care settings across Scotland.
More information and stories about ‘What Matters to You?’ stories can be found on the website at: http://www.whatmatterstoyou.scot/stories-asking-matters/
The following example is taken from the ‘What Matters to You?’ day report 2016 and demonstrates that the things that matter to people might not necessarily be medical issues.
Staff Involvement with ‘What Matters to You?’
I spoke with the mother of an 18 year old boy who has Down’s syndrome – he has recently made the transition from school (and children’s services) to a day centre and adult services.
She discussed with me that she felt that it was important that she remains a big part of her son’s care. Although he is 18, he has the mindset of a younger man and still looks to his mother for comfort. Her biggest fear would be if he was told that this was not appropriate.
We discussed how now that he attends the day centre, he would be encouraged to make appropriate relationships (no cuddling, only handshakes etc) but that he would be encouraged to keep his loving embraces for his mother. She seemed very pleased with this.
In contrast to this, she also discussed with me how it was important to her that his sleep pattern gets better again, as recently he has been up a lot through the night and she feels that as he is an adult now, she can’t tell him what to do.
I discussed with her that I would educate him around his sleep hygiene pattern and should the need arise will attend a GP appointment to have this reviewed.
We also discussed how it was important to her that he attended his day centre. She struggles with how much he misses his friends so when he is having a bad day, he refuses to get out of his bed and go to the centre. I discussed how I would create a storyboard for him which she can go over with him which will remind him about all the new friendships he has made at his day centre and also about the groups he attends through his centre at another centre within the area (where he sees some of his old friends from school). I asked Mum if she felt that it would be better to use actual pictures of him at his centre and she agreed that he would respond better to this. I then contacted his centre and clarified that this would be possible and they will supply photographs of him at the centre.
His mother was very happy with our discussion and the planned outcomes and thanked me for my help.
‘What Matters to You?’ addresses Commitments 1, 2, 3, 4 and 5 of the UK Strategy. It is a question that should be asked of people with a rare disease, and their carers/families. Quite often people feel like they are not included in their care and the real issues that are facing them are not discussed in the health care setting. The ‘What Matters to You?’ initiative helps to facilitate this discussion by training staff to really listen to what matters to the individual and improve the care and support that they really need. It will also help to raise awareness of rare diseases as staff will hear first-hand experiences of the rare disease and what it is like to live with the condition.
1.7 Care Opinion
Care Opinion [15] (previously Patient Opinion) is a not-for-profit social enterprise that provides an online feedback service that enables people in Scotland to give real-time feedback, and engage in constructive dialogue with healthcare service providers about the services they, their families, or the people they care for, have received.
The Scottish Government has supported the roll out of Care Opinion across Scotland since 2013. A contract was awarded in April 2015, which provides for every territorial NHS Board in Scotland and relevant special boards to be fully registered with the service. Care Opinion have recently been awarded a new contract and the Scottish Government will continue to provide for the NHS Boards to fully register with the service until 31 March 2020.
All Boards subscribe to Care Opinion and are reading and responding to issues directly. There are now around 1000 NHSScotlandstaff reading stories and we continue to see a higher distribution of staff responding as time goes on. This allows people posting stories to receive a targeted response and provides assurance that their concerns, or messages of thanks, have reached the appropriate staff member(s).
Care Opinion held an event in Glasgow on 17 May 2017 for clinicians wishing to explore how they and their teams can use Care Opinion to support their local learning and improvement work. Some clinicians at this event reported barriers to testing ways of supporting clinicians to respond to postings on Care Opinion. This was subject to social media discussion, which involved some Scottish Government officials emphasising support to empower more clinicians to use Care Opinion if they wish to do so. A further event for Clinicians is planned for February 2018.
In 2017, there were 3029 stories about health and social care services in Scotland shared, and to date over 10,000 stories have been shared. Of these stories, 60 have initiated changes in how health and social care services are being delivered, these include:
- NHS Ayrshire & Arran are making changes to ensure appropriate support is in place for vulnerable people “Sending a vulnerable adult home alone”
- NHS Borders have created a new information leaflet for people attending ambulatory care appointments “We came away with no questions answered”
Care Opinion intends to focus on development in the following areas:
- Support Care Opinion and NHS Board clinical leads to explore effective ways to empower and support clinicians to respond to posts and to use information to further refine and develop clinical involvement, that is linked to local learning and quality improvement work.
- Continue to seek time-effective ways for subscription managers across Scotland to share best practice.
- Seek ways to improve site accessibility and enable a wider range of people to share their experiences.
- Create case studies and further exemplar videos to demonstrate the impact of using Care Opinion in order to encourage feedback.
- Continue to raise public awareness through partnerships with third sector patient-led organisations, social and conventional media.
Care Opinion addresses Commitments 2, 3 and 4 of the UK Strategy for Rare Diseases. It allows people to share their experiences of the care they have received from the NHS. These can be either positive or negative experiences which are directly accessed by the relevant staff in the relevant health board. It gives staff the opportunity to hear and address first-hand experiences of care. This can help open a dialogue between the person and staff member(s), or allow staff member(s) to consider making changes to service provisions and/or share good practice with other health boards.
The extracts below are from people and relatives of people with a rare disease.
Steven-Johnson Syndrome
Comment from Patient:
My son became seriously unwell, developing a nasty condition called Stevens Johnson Syndrome. After several contacts with our local GP practice within a 24 hour period, and a trip to our local out-of-hours service, he was admitted to hospital.
His condition worsened and the situation was distressing for all involved, including the staff, most of whom had never experienced this illness before.
However, I cannot fault the professionalism of the people looking after him, in particular Dr Kelly and an amazing nurse, Heather. Heather clearly does not just do her job, she has an exceptional gift of engaging with children and displaying a level of empathy I have never seen in any professional before.
After six days of not being able to eat, Heather told my son she’d find him anything he wanted, and she did. He was still unable to eat but just being able to have a small taste of something he liked meant a lot. Of note, other fantastic nurses on the ward were Victoria, Hazel and Emma. Committed, talented nurses.
I could give many more examples of how these special individuals went the extra mile but, what was truly the worst week of our lives, could have been much worse had it not been for these fantastic, unsung heroes. The NHS is full of them.
Response from NHS Board:
Thank you very much for taking the time to share your experience with us at such a difficult time for you and your family. It is always rewarding to have the hard work and kindness of staff recognised. I will ensure all staff involved in caring for your son are aware of your comments.
I hope your son continues to make progress.
Best wishes.
Neurofibromatosis
Comment from patient:
My sister lives in your region, she doesn’t drive and has two young children. To get to the hospital, she needs to take two trains and a taxi, and the return journey, including her appointment takes in the region of seven hours. I explained to her at the time that our local hospital doesn’t provide neurological services and that is why she has to travel, however, what I am struggling to understand now is why she needs to keep attending there for follow up appointments.
NHS Board Response:
I’ve passed your feedback to the managers for both of these services to highlight the points you’ve made. The General Manager for Ophthalmology would like to have a look at this in more detail to see if there’s a way we could change this to make it easier for your sister.
Patient response:
Thank you for the quick and helpful response. I have updated my sister tonight and she is really pleased someone is at least willing to properly consider the options around this. She will be in touch via email with her personal details.
1.8 Our Voice
In June 2014 the Cabinet Secretary for Health and Wellbeing said:
“We must do more to listen to, and promote, the voices of those we care for. We need the voices of patients, those receiving care and their families to be heard in a much clearer and stronger way.”
Lots of different organisations have come together to develop Our Voice [16] , including the Scottish Government, NHS Scotland, the Scottish Health Council, HIS, the Convention of Scottish Local Authorities ( COSLA), the Health and Social Care Alliance Scotland (the ALLIANCE) and other third sector partners.
Before developing the Our Voice framework, they wanted to ensure that they were delivering something that people wanted, was useful and would make a difference to how people’s voices are heard across Scotland. Many different engagement activities were undertaken, including national events, discussion groups, online surveys and connecting through social media in order to speak to as many people as possible.
Once the feedback was gathered, the team found 7 key themes that came up time and again.
They were:
- Active Citizenship
Support to help people develop the skills needed to take an active role in making decisions about their own care and support. A need for more open and useful conversations between patients, staff and the wider health and social care systems. - Benefits and Outcomes
Supporting people to speak out and have their voice heard brings positive benefits for health and wellbeing. Encouraging health and social care services to act on what they hear should be a goal of the Our Voice programme. - Culture Change
A change of values and culture is needed. People’s views should be welcomed and steps taken to remove barriers such as fears about the effect of giving feedback on future treatment. - Methods and Approaches
There should be a range of ways for people to have their views heard. Face-to-face and online methods should complement each other. - Information and Support
Appropriate support should be available to make sure patients and people who use services have equal opportunity to have their voices heard. This includes clear information on how to get involved and communication support if needed. Access to advocacy and peer support helps build up people’s ability to speak up for themselves. - Principles and Standards
There should be a single standard for participation across health and social care. This should build on the good practice that already exists such as the Participation Standard and the National Standards for Community Engagement. - A Whole System Approach
An approach which strengthens the voices of patients, people who use services, carers and members of the public within health and social care must run at individual, local and national levels. This approach means people can have their say and influence decision making throughout the whole system.
The Our Voice website provides information on rights and responsibilities for individuals, information on how to make complaints, self-directed support and advocacy services.
It also contains information on the National Voice, which provides opportunities for people to join in with discussions about national health and social care policy. It can involve joining a website for a discussion forum or attending a group. There is also information on consultations and details of support organisations and networks.
For more information on Our Voice and how you can participate, please see the website: https://www.ourvoice.scot/
Our Voice addresses Commitment 1 and 4 of the UK Strategy for Rare Diseases.
1.9 National Specialist Services Committee
The National Specialist Services Committee ( NSSC) is responsible for providing recommendations to the NHS Board Chief Executives’ Group ( BCEs) and to the Scottish Government Health and Social Care Directorates ( SGHSCD) on the commissioning of highly specialised services for patients in Scotland with complex needs or rare conditions.
NSSC reviews proposals for national designation of specialist health services and Managed Clinical Networks. They then make recommendations on whether national commissioning is appropriate for each of the proposed national services/networks. Proposals for national services/networks might arise from service planning by SGHSCD, the National Planning Forum, Regional Planning Groups and NHS Boards; or they might be applications from clinicians for designation of specific services/networks which are supported by their NHS Board(s).
In the first instance, NSD supports appropriate applications on new developments for submission to the National Professional, Patient and Public Reference Group ( NPPPRG), who liaise with professional, patient and public representative groups, regional planning groups and other relevant bodies. The group gather information in order to provide expert advice to the National Specialist Screening Committee [17] .
1.10 National Network Management Service ( NNMS)
The NNMS commissions national clinical and diagnostic networks on behalf of NHS Boards and the Scottish Government. They provide high quality management and operation support to enable them to focus on adding value to healthcare in Scotland through better access to specialist care.
The national networks ensure patients with rare or complex conditions have access to high quality specialist care. In particular, the diagnostic networks support early diagnosis and intervention by ensuring that patients have the right test at the right time. However, they all bring together everyone involved in providing care when the full range of skills required isn’t available within a single health board or region – this includes health professionals, carers, patients families and voluntary groups.
This helps to:
- Better understand and meet patients’ and carers’ needs.
- Facilitate the design and mapping of services across Scotland.
- Measure and improve the quality of care.
- Ensure health professional and carers receive the information and education they need.
As such, national clinical and diagnostic networks directly support more than a quarter of all commitments within the UK Rare Disease Strategy – 1-5, 7, 8, 11, 12, 15, 18, 23, 32).
| National Networks in Scotland |
||
|---|---|---|
| For children & adults |
For Children |
Diagnostic |
| Burns |
Epilepsy |
Biochemistry |
| Inherited Metabolic Disease |
Endocrine |
Clinical Imagining |
| Cleft Lip and Palate |
Cystic Fibrosis |
Microbiology & Virology |
| Familial arrhythmias |
Allergy |
Pathology |
| Phototherapy |
Rheumatology |
Cancer |
| Gender identity |
HIV/ PID |
- Sarcoma |
| Acquired brain injury |
Exceptional Healthcare Needs |
- Adult Neuro Oncology |
| Haemaglobinopathies |
Disorders of Sex developments |
- Pancreatic/hepatobilia |
| Diaphragmatic Hernia |
Renal & Urology |
|
| Inherited bleeding |
Visual Impairment |
|
| Perinatal Mental Health |
||
| Neuromuscular Disorders |
||
Access to individual network websites for information and guidance is available on the NNMS website at http://www.mcns.scot.nhs.uk/
Guidance on the role of networks was set out by the Scottish Government in the CEL 29 (2012) “Managed Clinical Networks: Supporting and Delivering the Health care Quality Strategy”. This recognised the important role of networks in influencing service re-design, quality improvement, strategy and planning across pathways that may reach across health boards, sectors and agencies. It established a set of core principles for networks that describes some of the governance and structural requirements for networks and outline some specific areas for networks to address, including:
- Working to a documented evidence base. Often for national networks this will be through the development of pathways and guidelines based on the evidence available, the knowledge and experience of the specialist clinicians and the experiences of the patients and their families. This will be complemented by a programme of audit and quality improvement within the network to support the delivery of high quality care.
- Optimising the education and training potential of the networks. Sharing knowledge across Scotland is a key role for national networks and they will develop an education strategy to ensure there are appropriate opportunities available at the right level for the different groups of professional staff within the network and for patients and carers. Examples of ways this may be delivered are through national conferences, online learning, local roadshows and multi-disciplinary case discussion meetings.
- Engaging stakeholders, particularly patients and their families or carers. National networks where possible look to include patients and their representatives as active members of the network alongside clinical stakeholders and try to ensure good communication with all. In addition, national networks will employ a variety of methods to engage with patients and families including through patient and family events, online or clinic questionnaires, newsletters, social media and websites. What matters to patients and families strongly influences the improvement priorities of the network.
- A defined structure setting out the points at which the service is to be delivered and the connections between them. National networks will map out the services available for patients and families across Scotland for the area they support and look to influence any potential improvements in the pathways of care.
On 24 October 2016, the NNMS held an event for health care professionals and partners. Through a programme of presentation and workshops by network leaders and experts, the event focussed on forging relationships to maximise and share the impact of the national networks on health and social care.
More information on the progress of new NMCNs and pathways can be found below at section 3.1.
1.11 Health and Social Care Standards
In 2014, Ministers committed to a review of the Care Standards with the aim of developing new standards capable of being applied across both health and social care services. The new standards ‘Health and Social Care Standards: My support, my life’ [18] which come into effect on 1 April 2018, will be applied to a diverse range of services from daycare for children, housing support and care at home for adults, to hospitals, clinics and care homes. They will apply to the NHS as well as services registered with the Care Inspectorate and HIS. This sets out the standards that people should expect when using health and social care services.
The Standards are focused on improving people’s experience of care and are based on the following outcomes:
- I experience high quality care and support that is right for me.
- I am fully involved in all decisions about my care and support.
- I have confidence in the people who support and care for me.
- I have confidence in the organisation providing my care and support.
- I experience a high quality environment, if the organisation provides the premises.
The Standards are underpinned by five principles: dignity and respect, compassion, be included; responsive care and support and wellbeing; which reflect the way that everyone, including people with rare diseases should expect to be treated. These standards help towards meeting Commitments 3, 4 and 5.
1.12 Provision of Communication Equipment and Support
In March 2016, the Scottish Parliament passed Part 4 of the Health, (Tobacco, Nicotine etc. and Care) (Scotland) Act 2016 [19] on the Provision of Communications and Equipment and Support. This gives children and adults across all age ranges and care groups, who have lost their voice, are at risk of losing their voice, or who have difficulty speaking, a statutory right to access the communication equipment and support they need. The legislation gained Royal Assent in April 2016 and is not specific to particular health conditions.
The legislative duty has not commenced as Directions to support the implementation of the legislation are being prepared for the NHS and other key service providers.
Discussions are also taking place with the Scottish Government legal colleagues and Health and Social Care Integration policy colleagues to determine the legal responsibilities and functions that Integrated Joints Boards have before the full legislative process can commence. Although the legislative duty is not complete, specialist augmentative and alternative communication services are being, and continue to be, provided across Scotland.
This legislation addresses Commitments 2 and 4 of the UK Strategy for Rare Diseases. It is an important step forward for people with progressive rare diseases such as Parkinson’s Disease, Motor Neurone Disease, and Huntington’s disease. It will allow people to be able to communicate and have their “voice” heard when they are no longer able to speak or have difficulties speaking, ensuring that they receive the care and support that they want and need.
1.13 Frank’s Law
The First Minister, during her Programme for Government (PfG) announcement on 5 September 2017, announced that the Scottish Government would, over the next year begin work to fully implement Frank’s Law [20] , by extending Free Personal Care to those aged under 65 who are assessed as needing this service, regardless of their condition. Extending Free Personal Care to people under 65 will benefit around 9,000 people in Scotland.
1.14 National Patient Portal
The Scottish Government has commissioned a programme of work to advance the development of a national patient portal which will benefit all people in Scotland, but this will also help to meet Commitment 6 and 19 in the UK Strategy for Rare Disease. The programme is currently working on the delivery of a technical proof of concept, developed in collaboration with an agreed supplier, as well as an outline business case. This work is expected to be concluded by March 2018 in line with the existing aim of launching a portal with initial functionality by 2020. This initial functionality, which would be subsequently expanded, is likely to include access to a summary patient record, online GP services, electronic communications and personalised health information for every citizen in Scotland.
People with rare diseases often have to attend a number of different clinics in order to manage their treatment. This can also include having numerous tests carried out or providing various clinicians with information. The national patient portal will allow people with a rare disease and their carer/family access to information such as appointment letters, access to GPs or other services, a summary of their information and some as well as personalised health information, for example, some test results. This will give the person more flexibility in managing their condition and being able to access services when they need it.
1.15 Scottish Genetics Speciality Group
The role of NHS research is to support the delivery of clinical research in Genetics. It also manages participant recruitment ensuring that they are recruited in time and on target. The research includes Scottish led studies and ones which Scotland is participating in. At the moment there are approximately 30 studies and about one third of these are led from Scotland.
The Genetics Speciality supports the delivery and promotion of clinical research in a wide range of areas, including:
- rare diseases;
- causes and prevention of birth defects;
- common disorders such as familiar cancer; and
- genetic approaches to treatment and prevention.
In terms of rare diseases, the national approach made possible by the National Institute for Health Research ( NIHR) Clinical Research Network Portfolio, and supported by the Scottish Genetics Speciality Group means that together, they are able to collect enough people with a particular condition to make research more feasible. This approach provides more opportunities for people with rare genetic diseases to participate in research, which will lead to improved care and the development of new treatments.
A number of studies have been available to people with a rare diseases, but the majority to date, have been observational (understanding the cause and natural history of a rare disease). However, there are a small number of interventional studies – there is Scotland-wide participation in the Association for Improvements in the Maternity Services ( AIMS) study for Marfan syndrome and the Cancer Prevention Programme3 ( CaPP3) for Lynch syndrome.
Other studies which have been carried out and the outcomes of which are due to be implemented are:
The DDD Study
The Deciphering Development Disorders ( DDD) study aimed to find out if using new genetic technologies could help doctors understand why patients get developmental disorders. All of the Scottish Genetic Centres participated in the study, recruiting some 1400 participants. The outcome demonstrated a three-fold increase in diagnosis using Exome enriched Next Generation Sequencing compared to using conventional technology. Previous figures showed that 9% of patients obtained a successful diagnosis using the conventional methods, but by using Exome enriched Next Generation Sequencing, 27% of participants received a diagnosis for a rare development disorder.
The Scottish Genetics Laboratory Consortium (see Section 4.4) is planning to implement this as standard across Scotland, however, there are serious cost implications attached to the test, and NHS Boards have to manage this along with all the other services that they offer. As a result, Scotland is not as far advanced as their English counterparts in implementing this, nevertheless, the Consortium is aware that this is the only test that will lead to a diagnosis in many children with severe developmental disorders and are looking into the matter very carefully.
Meaning
Exome enriched Next Generation Sequencing
Next Generation Sequencing is the term used to describe modern technology that enable scientists to sequence DNA faster and more cheaply than previous sequencing techniques. It has revolutionised the study of genomics, by allowing us to sequence every gene in a person. This is particularly important as many rare diseases are caused by faults in genes that can only be detected using this technology.
The RAPID Study
The RAPID study Dundee participated in, demonstrated the clinical utility and cost saving of non-invasive prenatal testing ( NIPT) for chromosomal trisomies compared to conventional technology which requires amniocentesis.
The new form of testing is non-invasive as it only requires a blood sample being taken from the mother. It can be carried out at 10 weeks of pregnancy and there is no chance of miscarriage. The test uses fragments of fetal DNA, that is found in the mothers blood stream during pregnancy, to check for Trisomies. Trisomies means that there are three copies of one particular chromosome, instead of two (one from each parent), examples of Trisomies include Down syndrome, Edwards Syndrome and Patau syndrome.
Following participation in this study, Dundee piloted this approach demonstrating a cost saving and reduced risk to pregnancies. The Scottish Screening Committee is now overseeing the implementation of this and have commissioned a business case from NHS National Services Division, which was considered at their meeting in November 2017. Next steps involve seeking agreement from Directors of Finance and Board Chief Executives on the investment required to make this available across Scotland.
For more information about NIPT visit Antenatal Results and Choices: http://www.arc-uk.org/tests-explained/non-invasive-prenatal-testing-nipt
The Scottish Genetics Speciality Group procedures help towards meeting Commitment 7 and 8 of the UK Strategy for Rare Diseases.
Contact
There is a problem
Thanks for your feedback