Scotland's Oral Health Plan: consultation on the future of oral health
Consultation on how we take dental services forward to meet the challenges of the future.
3 Addressing the Challenges
Identifying the Challenges
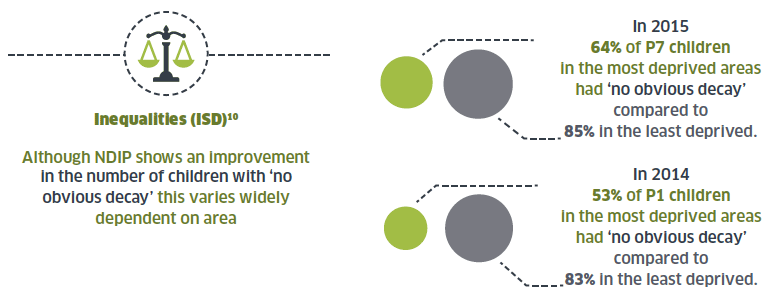
3.1 One of the Scottish Government's key priorities is the need to address the significant and persistent inequalities in the population and the adverse effect these have on health outcomes. The evidence from the National Dental Inspection Programme ( NDIP) shows that although oral health has improved significantly across all communities, children living in the most deprived communities still have more decay experience compared with those in the least deprived.
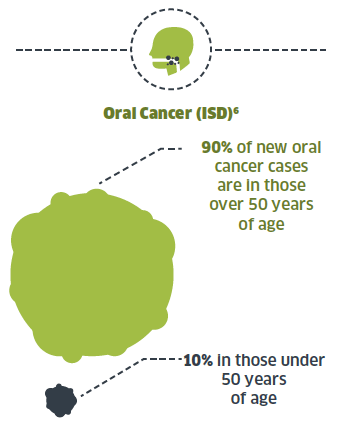
3.2 There continues to be an increase in the incidence of oral cancer, while that of other cancers is decreasing. While oral cancer primarily affects those over 50 years of age it can also affect younger people.
3.3 The current system in NHS dentistry is embedded in a restorative culture. However this does not fit with the new preventive agenda that we are already seeing with the Childsmile Programme. There is a need to further incentivise prevention rather than treatment amongst the dental team, with the resultant improvements in oral health and costs avoided of otherwise having to provide relatively expensive restorative treatments.
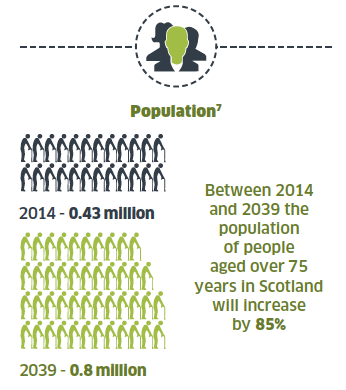
3.4 The improvements that have been made in oral health in Scotland have also presented us with new challenges. The increasing ageing population combined with more adults retaining some or all of their natural teeth inevitably means there will be a significant increase in people requiring domiciliary care, either in their own home or in residential care.
Reducing Oral Health Inequalities
3.5 Despite the success of the Childsmile Programme, health inequalities with respect to oral health persist in Scotland. For example, 53 per cent of Primary 1 children in the most deprived areas have 'no obvious decay'; the equivalent figure for the least deprived areas is 83 per cent. [8] This gap between least and most deprived needs to be further addressed and engagement with parents, communities and certain Third Sector organisations will be key to achieving this.
3.6 Similarly, the proportion of adults living in the most deprived areas who had some natural teeth was 86 per cent, compared with 95 per cent of those in the least deprived areas. In addition, nearly three times as many people from the most deprived backgrounds as those from the least deprived had no natural teeth. [9]
3.7 At present, as part of the Childsmile Nursery Programme, three and four year olds benefit from daily supervised toothbrushing. We will extend this programme to two year old children with nursery places. In addition we will extend the fluoride varnish element of the Childsmile Nursery Programme to the 20 per cent most deprived children at a Scottish level, as measured by the national Scottish Index of Multiple Deprivation ( SIMD).
3.8 For adults, we will look to take a more holistic approach to the NHS dental examination by introducing an Oral Health Risk Assessment ( OHRA) to help patients improve and maintain their oral health. This would mean patients receiving dental advice more specific to their needs. For example, the benefits of smoking cessation and diet advice in relation to oral health can also contribute to the improvement of the general health of patients.
3.9 The 2012 National oral health improvement strategy for priority groups [12] set a clear direction for NHS Boards regarding frail older people, people who were homeless and people with special care needs (e.g. a person with a learning disability). It is clear that there are many effective measures to prevent oral diseases if action is taken early. NHS Boards have begun to take action to support people within these priority groups. In future the intention would be to encourage NHS Boards to identify and share best practice. The Scottish Government will look at ways to facilitate this and establish a more joined-up approach across NHS Boards and localities.
Oral Cancer Pathway
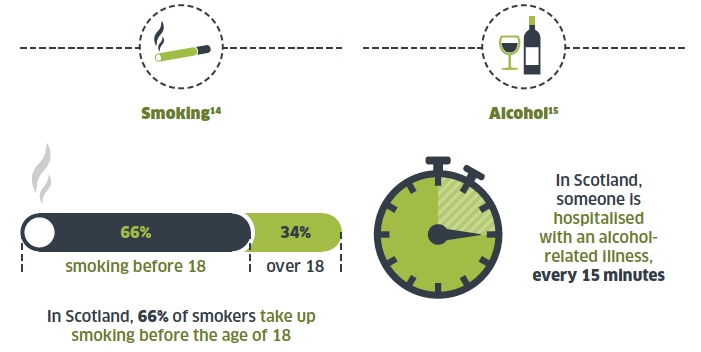
3.10 There continues to be an increase in the incidence of oral cancer, while that of other cancers is decreasing. In the United Kingdom, oral cancers account for between 1 per cent and 4 per cent of all malignancies. [13] The major risk factors in the development of oral cancer include tobacco use and the excessive consumption of alcohol, and these risks multiply when in combination.
3.11 A clear association is seen between social deprivation and incidence rates of oral cancer and this relationship is stronger in males. Whilst approximately 90 per cent of new cases of oral cancer occur in people aged over 50 years, oral cancer should not be considered a disease affecting only older people.
3.12 At the dental examination a discussion between dentist and patient about risk factors can help patients manage those behaviours which increase the risk of oral cancer. If, at the dental examination, the dentist has concerns that a patient may have signs of oral cancer we will ensure that there is a consistent approach to urgent referral to an oral cancer care pathway to streamline diagnosis and treatment.
Summary of Proposals:
- Move towards a national SIMD basis for targeting fluoride varnish in children;
- Improve our engagement with parents, communities and those Third Sector organisations that help support people with special care needs;
- Look at ways to ensure a consistent joined-up approach between NHS Boards to improve oral health and services for people with special care needs;
- Review the approaches taken by NHS Boards regarding their oral cancer pathways to streamline diagnosis and treatment.
Modernising NHS Dental Services
3.13 The current system of remuneration for independent GDPs is complex, difficult to administer and manage, while equally difficult for patients and GDPs to understand. The number of different types of payments, and mechanisms for making payment, mean that it is difficult to appropriately incentivise GDPs to provide the care which delivers the desired oral health outcomes.
3.14 There are over 400 items of treatment that a GDP could provide, each of which has a set fee (for example, GDPs earn a fee for filling a tooth). The items of treatment which GDPs can provide under NHS arrangements and the associated payments to GDPs, and patient charges, are set down in the Statement of Dental Remuneration ( SDR).
3.15 It is our aspiration to introduce a preventive care pathway with more emphasis on maintaining or improving the level of oral health. Our vision for a new preventive dental culture requires a system of payments to dentists which reflects its positive nature and aligns payments to the needs of the patient, whilst rewarding the time, effort and hard work that the dental team put in to promoting and maintaining good oral health.
3.16 Initially this new preventive care pathway will be introduced for children in good, stable oral health, building on the continuing success of the Childsmile Programme. We anticipate that the majority of children at present would qualify for this new preventive treatment pathway. The new pathway will run concurrently with item of treatment. This recognises that where a child has poor or unstable oral health then continuing to remunerate the dentist through item of treatment would be more appropriate.
3.17 As children with stable oral health transfer into the adult service (i.e. from the age of 18) they will remain on the preventive care pathway. Children with poor or unstable oral health on reaching the age of 18 will remain on item of treatment.
3.18 Initially all existing adults will remain on item of treatment, as this recognises that a proportion of the adult population will require treatment on a regular basis. Over time it is expected that adult patients with stable oral health would move from item of treatment to a preventive treatment pathway. This would be a gradual change and informed by the new preventive pathway for younger adults.
3.19 We will also review the items of treatment within the SDR to ensure they are up to date and fit for purpose.
Oral Health Risk Assessments ( OHRA)
3.20 Our intention would be to introduce an Oral Health Risk Assessment ( OHRA) for all patients at 18 years of age as part of oral health care planning. An OHRA involves a full dental examination and includes a discussion between the dentist and patient about associated risk factors such as smoking, alcohol intake and medication. This patient-centred approach encourages the involvement of patients in managing their own oral health.
3.21 Introducing OHRAs at this age reintroduces oral health surveillance at a key age. This would provide young people at a transitional stage in their lives with tailored oral health information that will assist them in caring for their oral health more effectively.
3.22 We anticipate that OHRAs would be repeated at regular intervals to ensure that this group of people were receiving the most appropriate treatment for their oral health and to ensure they are on the correct pathway.
Patient Charges
3.23 At present children under 18 years of age are entitled to free NHS dental treatment, while all adult patients receive free NHS dental examinations.
3.24 Following a dental examination, unless an adult patient is entitled to free NHS dental treatment or qualifies for help towards the cost, they are currently required to pay 80 per cent of their NHS dental treatment cost up to a maximum of £384 per course of treatment, with the Scottish Government meeting the remaining costs.
3.25 At present the charging system is extremely complex; the amount an adult patient is required to pay towards the cost of their NHS dental treatment depends on the extent and nature of the treatment they receive.
3.26 We propose that when adult patients on the preventive care pathway receive treatment, they will pay a simplified system of charges.
3.27 This could be the first step in simplifying the system of patient charges towards the cost of NHS dental care and treatment.
Summary of Proposals:
- All children with stable oral health would transfer into the new preventive care pathway.
- All adults (and children with poor and unstable oral health) would remain on item of treatment.
- The existing SDR will be reviewed to ensure it is up to date and fit for purpose.
- An OHRA would be introduced, in the first instance at 18 years of age and would be free of charge.
- As children transfer into the adult service (at 18 years of age) they would remain on the new preventive care pathway, unless the OHRA determines that they should revert to item of treatment.
- If, after completing the OHRA, it is decided that an adult patient, who is required to pay a contribution to their NHS dental treatment, will remain on item of treatment they will continue to pay a percentage of the cost of their NHS dental treatment, up to a set maximum per course of treatment.
- If an adult patient's OHRA determines that they qualify for the new system of preventive dental care, we propose a simplified system of charges payable when treatment is provided.
Enhanced Service Model
3.28 A full range of NHS dental treatments are able to be delivered by GDPs. However, some treatments such as oral surgery and treatment under intravenous sedation, are increasingly being referred inappropriately to the PDS and HDS, which inevitably has a detrimental impact on these services. These procedures could alternatively be delivered by GDPs with enhanced skills or specialists working in 'enhanced service' practices.
This will:
- allow patients to receive more complex treatments closer to home without the need to attend a hospital;
- shift the balance of care from secondary to primary care dental services.
Top Ten Reasons for Admitting a Child to Hospital for Day Cases (2013-14) [16]
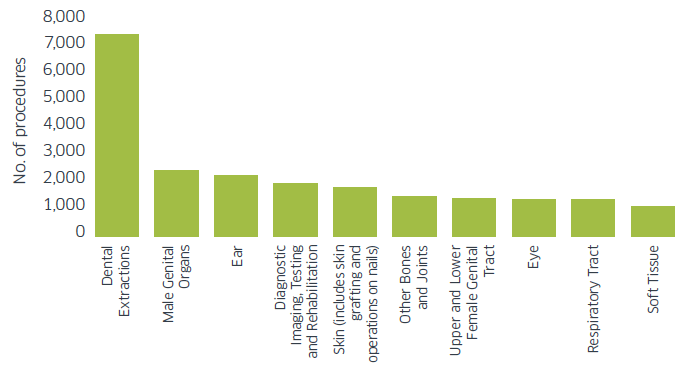
3.29 Given H&SCPs' role in strategic planning and commissioning of health and care services, we anticipate that H&SCPs will be able to commission enhanced services within a National Framework, including:
- domiciliary care (complex cases);
- oral surgery (complex extractions);
- restorative services (complex treatment);
- treatment under intravenous sedation;
- orthodontics.
Domiciliary Care for Dependent Older People in Care Settings
3.30 At present the majority of oral health care for dependent older people in a care home setting is provided by the PDS. Our proposal is to ensure that these services are delivered where possible by GDP-led teams. This could be by introducing an enhanced service model for the provision of domiciliary care in a care home setting. There should be recognition that practices delivering an enhanced service to treat care home patients may need specific experience and equipment. The same approach could be used for highly dependent people cared for at home.
Emerging Technologies and Treatments
3.31 We will continue to review the clinical and economic evidence for new technologies and treatments to determine whether they can be delivered within the NHS through an enhanced service model.
Finance
3.32 At present the budget for GDS is held centrally by the Scottish Government. There are a number of areas where we envisage greater control by NHS Boards and H&SCPs in the delivery of local NHS dental services, for example, the proposals around enhanced service delivery. Given that H&SCPs are now fully operational it would seem sensible to begin to consider options for them to take on greater responsibility for the financial planning and management for GDS.
Summary of Proposals:
- Introduce an enhanced service model for the provision of domiciliary care in a care home setting, and for highly dependent people in their own homes.
- Undertake in partnership with NHS Boards and H&SCPs the development work to pilot additional enhanced services within GDS in oral surgery, restorative services, intravenous sedation and orthodontic care.
- Consider options for how H&SCPs can take on greater responsibility for the financial planning and management for GDS.
Contact
Email: David Notman, david.notman@gov.scot
There is a problem
Thanks for your feedback