Scottish Cancer Patient Experience Survey 2015/16
Results from the 2015/16 Scottish Cancer Patient Experience Survey. The survey covers the full care journey that a cancer patient experiences, from thinking that something might be wrong with them to the support they received after their acute-care treatm
This document is part of a collection
Hospital care as day patient/outpatient
When patients go to hospital for shorter periods of time - such as for specialist clinics, treatment, or follow-ups - it is equally important for them to experience continuity of care, feel supported and informed, and be able to access someone to speak to about any worries and fears.
Questions in this section seek to gauge people's experiences of these aspects of care.
One of the areas explored is whether patients received coordinated and consistent administration. One key to good care is health professionals having the correct records and documents, not only for medical accuracy but also to instill confidence and trust in the care being received and to avoid patients having to repeat details of their care to date.
The majority of patients (84%) had been treated as an outpatient or day case for cancer care (Table 38).
Table 38: Treatment as outpatient or day case
| Have you been treated as an outpatient or day case for cancer care? |
n |
% |
|---|---|---|
| Yes |
4,018 |
84% |
| No |
742 |
16% |
| Total |
4,760 |
100% |
Worries or fears as outpatient/ day patient
Patients were asked whether they were able to find someone on the hospital staff to talk to about their worries and fears. Nineteen per cent of patients reported that they did not have worries or fears, indicating that around four in five patients do experience worries or fears during outpatient or day case episodes (a higher rate than for inpatient stays).
Of the patients that did experience worries/fears, around one in ten (9%) were not able to find someone to talk to (Table 39). This is a more positive result than the similar question asked for inpatient cancer treatment, where double the proportion of patients (18%) were unable to find someone to speak to about their worries or fears.
Table 39: Worries and fears as outpatient / day case
| While you were being treated as an outpatient or day case, did you find someone on the hospital staff to talk to about your worries and fears? |
n |
% |
|---|---|---|
| Yes, definitely |
2,173 |
69% |
| Yes, to some extent |
701 |
22% |
| No |
294 |
9% |
| Total |
3,168 |
100% |
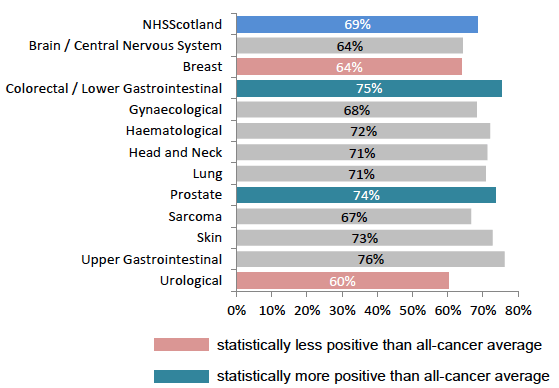
Patients with breast (64%) and urological tumours (60%) were both statistically below the all-cancer average in reporting being able to find someone to speak to about their worries and fears. Patients with colorectal / lower gastrointestinal (75%) and prostate tumours (74%) were both statistically above average (Figure 30).
Figure 30: % finding staff member to talk to about worries or fears, by tumour group
Right documents available for outpatient appointment
In the overwhelming majority of cases (98%), patients reported that cancer doctors had the right paperwork for their outpatient appointment (Table 40).
There was some variation in responses from different tumour groups. However, statistical tests concluded that these differences as a whole were not statistically significant.
Table 40: Right documents available for outpatient appointment
| The last time you had an outpatients appointment with a cancer doctor, did they have the right documents, such as medical notes, x-rays and test results? |
n |
% |
|---|---|---|
| Yes |
3,707 |
98% |
| No |
95 |
2% |
| Total |
3,802 |
100% |
Contact
There is a problem
Thanks for your feedback