Scottish maternal and infant nutrition survey 2017
Results from the 2017 Scottish Maternal and Infant Nutrition Survey. This first Scotland-only survey gathered data on maternal nutrition and infant feeding.
1. Introduction
1.1 Maternal and infant nutrition in Scotland
It is known that the diet and nutritional status of mothers before and during pregnancy and the feeding received by infants is associated with the long term health of the population. ( R1, R2) There is also increasing evidence of the importance of preconception health and the influence this has on the likelihood of an infant going on to develop chronic diseases later in life. ( R3)
The Scottish Government aims to ensure that all children have the best possible start in life, are ready to succeed and are able to live longer, healthier lives. These outcomes form part of the Scottish Government's National Performance Framework. ( R4)
To help achieve these aims the Scottish Government published the Maternal and Infant Nutrition Framework for Action in January 2011. ( R1) The Framework was designed to support a variety of organisations in improving maternal and infant nutrition in Scotland.
The NHS and local authorities play a leading role in this work, but private and third sector organisations also have an opportunity to influence nutritional behaviours and choices.
Vision for the Maternal and Infant Nutrition Framework for Action:
- Women entering pregnancy are a healthy weight, in good nutritional health and this continues throughout their pregnancy and beyond.
- All parents receive full information they can understand on infant feeding to enable them to make an informed choice on how they will feed their infant.
- All women receive the support they need to initiate and continue breastfeeding for as long as they wish.
- Infants are given appropriate and timely complementary foods and continue to have a wide and varied healthy diet throughout early childhood.
It is recommended breastfeeding should continue beyond six months, alongside the introduction of appropriate solid foods, for up to two years of age or as long as the mother chooses.
1.2 Current maternal and infant nutrition recommendations
The Scottish Government currently has a number of recommendations in relation to maternal and infant nutrition. ( R1, R5, R6) These recommendations are summarised below and are discussed in more detail in sections 2- 8 of this report.
Pregnancy planning
- Actively planning for pregnancy is recommended. This should include taking folic acid while trying to conceive and continuing to do so until the twelfth week of pregnancy.
- Women are also advised to eat a healthy diet, maintain a healthy weight, stay active and refrain from smoking, drinking alcohol and taking recreational drugs.
- A Vitamin D supplement should be taken throughout pregnancy and whilst breastfeeding.
Breastfeeding
- It is recommended that infants are exclusively breastfed for the first six months of life. Thereafter, breast milk should continue to be given alongside appropriate complementary foods for up to two years or beyond, or for as long as the mother wishes.
Formula milk
- Where a mother chooses not to breastfeed, infant formula milk should be used until the baby is 12 months old. Guidance for the safe preparation, storage and handling formula should be followed.
- It is not necessary to switch to follow-on formula / second stage milk after six months. "Goodnight" milks are not recommended and specialist "over the counter" formula milks are rarely required.
Complementary foods and vitamin supplements
- At around six months of age a variety of complementary foods should gradually be introduced to infants alongside continued breastfeeding (and/or breast milk substitutes, if used).
- Cows' milk can be introduced as a main drink after 12 months. If provided, whole milk (rather than semi-skimmed or skimmed) should be used until the child is at least two years of age.
- Infants sh ould be given Vitamin D drops from birth [1] , unless receiving 500mls or more of formula milk a day.
1.3 The Scottish Maternal and Infant Nutrition Survey
In June 2015, The Scottish Government announced its intention to carry out the first Scottish Maternal and Infant Nutrition Survey ( MINS) to support the implementation of the Maternal and Infant Nutrition Framework for Action (2011). ( R1)
The overall aim of the survey is to gather data on maternal nutrition, breastfeeding, infant feeding and related health behaviours. This information will assist health services and other organisations to design and implement effective nutritional support for families.
Aims of the Scottish Maternal and Infant Nutrition Survey:
- Establish the extent to which mothers make suitable nutritional and health adjustments preconception and during pregnancy.
- Measure the proportion of mothers who consume alcohol just prior to and during pregnancy.
- Examine factors associated with mothers' feeding intentions and feeding and care practices adopted in the early weeks.
- Investigate the types of breastfeeding challenges experienced by mothers and their reasons for stopping breastfeeding.
- Establish how infants are being fed, and investigate variation in practices amongst different population groups.
- Investigate the introduction of complementary foods to infants and mothers' experiences of receiving information in relation to this.
- Measure levels of awareness of, and registration on, the Healthy Start Scheme and understand how Healthy Start vouchers are being used.
The decision to carry out the new Scottish survey was made in response to the cancellation of the previously well established UK-wide Infant Feeding Survey ( IFS). ( R7) The UK survey, conducted at five year intervals between 1975 and 2010, was a valuable resource that collected information directly from mothers at various stages following the birth of their babies. It provided data that helped to inform the work of many early years organisations.
The cancellation of the UK survey provided the Scottish Government with an opportunity to design a new survey more closely aligned with the MIN Framework ( R1) and related maternity and neonatal policies. The new Scottish survey continues to seek the views of mothers, but it also collects information from expectant mothers for the first time.
The Children and Families Directorate of the Scottish Government was responsible for directing the survey. To assist in this work, an Implementation Group was established to provide subject matter expertise and advice (see Appendix A for membership of this group).
The Scottish Government commissioned the Information Services Division ( ISD) of NHS National Services Scotland to oversee the day to day running of the project and to provide methodological advice and analytical / reporting expertise to the survey.
1. 4 Survey design
Three separate groups of women were invited to self-complete a questionnaire between March and July 2017:
| Antenatal: | Expectant mothers who were 20+ weeks pregnant between May and June 2017. |
|---|---|
| 8-12 week: | Mothers whose babies were 8-12 weeks old and who gave birth in Scotland between March and April 2017. |
| 8-12 month: | Mothers whose babies were 8-12 months old and who gave birth in Scotland between July and August 2016. |
A separate questionnaire was designed for each part of the survey, each focussing on maternal nutrition, breastfeeding, infant feeding and related health behaviours as appropriate to the relevant stage of pregnancy / motherhood.
For each part of the survey, the aim was to achieve a sufficiently robust sample to allow results to be presented at a national level and, where possible, to present results broken down by:
| Respondent age: | 19 or under, 20-24, 25-29, 30-34 and 35 or over. |
|---|---|
| Deprivation: | The Scottish Index of Multiple Deprivation ( SIMD) can be used to identify areas with higher or lower levels of deprivation. Respondents' postcodes were used to allocate responses to one of five deprivation groups ( SIMD 1 = most deprived; SIMD 5 = least deprived). Note that the SIMD identifies deprived areas, not deprived individuals. |
| NHS board of residence: | There are 14 NHS board areas in Scotland. Due to the small number of respondents living in NHS Orkney, NHS Shetland and NHS Western Isles, results for these boards have been combined. |
For the antenatal survey, National Records of Scotland ( NRS) Birth Registration Records were used to estimate the number of women who would be 20 or more weeks pregnant between May and June 2017. The appropriate number of survey packs, containing a covering letter, paper questionnaire and pre-paid return envelope, were printed and distributed to all Maternity Services across NHS Scotland. Maternity Service staff presented the survey packs to expectant mothers at routine antenatal appointments.
For the two postnatal surveys (8-12 week and 8-12 month), NRS Birth Registration Records were used to identify all women in Scotland with babies of the correct age. NRS mailed survey packs directly to these mothers.
A survey contractor (ScotCen Social Research) was appointed by the Scottish Government to test and prepare the survey materials and to carry out data collection.
Participation in the survey was entirely optional and respondents had the opportunity to complete the questionnaire either on paper or online. The timing of the fieldwork for each survey was carefully planned to avoid the same women being asked to complete more than one questionnaire.
Full details of the design, methodology and analysis methods used for the 2017 Scottish Maternal and Infant Nutrition Survey are described in the MINS Technical Report.
1.5 Survey response
More than 2,500 responses were received for each part of the survey, providing sufficient data to present results at a national level. Although response to each part of the survey was lower than anticipated, in most cases it has been possible to present results by respondent age, deprivation and NHS board of residence.
[Figure 1.1; Table 1.1]
Survey response rates.
Figure 1.1: Response to each part of the 2017 Scottish Maternal and Infant Nutrition Survey (number and percentage of responses to each part of the survey).
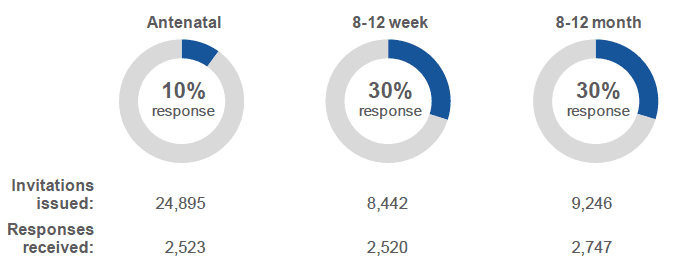
In the previous 2010 UK-wide Infant Feeding Survey ( IFS) the response rate for Scottish participants ranged from 45% (N = 3,107) to 31% (N = 2,119) depending on the stage in the survey. ( R7) However, it should be noted that the methodology and sampling strategy used in the IFS differed from that used in this survey.
1.6 Profile of survey respondents
Younger women and those who lived in the most deprived areas responded to the survey proportionately less frequently than older women and those who lived in the least deprived areas. This means that younger women living in the most deprived women are under-represented, whereas older women living in the least deprived areas are over-represented.
To help correct for these differential response rates, all survey results have been weighted by respondent age, SIMD quintile and NHS board of residence. Weighting methods are described in more detail in the MINS Technical Report.
[Figure 1.2; Table 1.2]
Survey response varied by age, deprivation and NHS board of residence.
Figure 1.2: Profile of survey respondents versus survey population (percentage of respondents (%, ◘) / percentage of women in survey population (│), by respondent age, deprivation and NHS board).
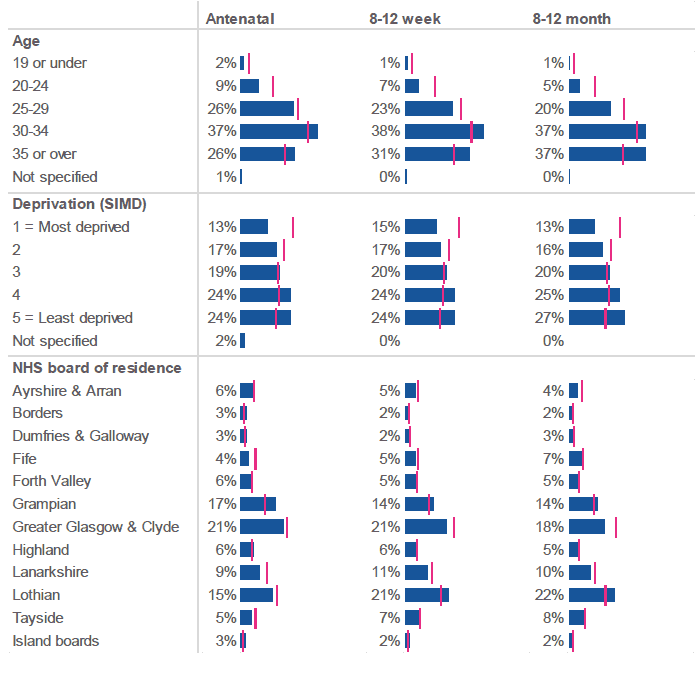
Respondents to the antenatal survey
The vast majority of women who responded to the antenatal survey (95%) were at least 20 weeks pregnant when they completed the survey; 3% were less than 20 week pregnant and 2% had already given birth. Half of respondents (50%) indicated that this was their first pregnancy.
[Figure 1.3; Table 1.3a]
The majority of respondents to the antenatal survey were at least 20 weeks pregnant.
Figure 1.3: Profile of antenatal survey respondents (percentage of respondents, by number of weeks pregnant and whether this was the respondent's first pregnancy).
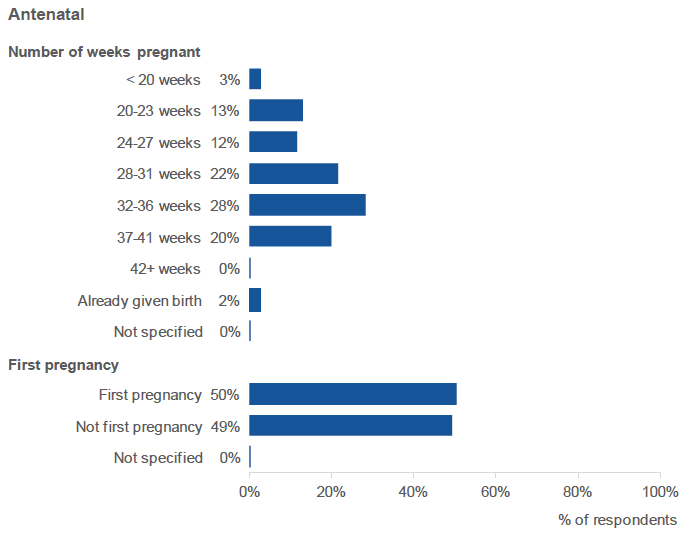
Source: Q1, Q2, Antenatal Survey
Respondents to the 8-12 week survey
For the 8-12 week survey, survey packs were mailed out to those being invited to participate when their babies were between six and nine weeks old (spanning the eight week target age).
The majority of respondents (68%) confirmed that their infant was at least eight, but less than 12, weeks old when they completed the survey. Twenty percent (20%) had infants aged less than eight weeks; 12% had infants aged 12 weeks or more.
The vast majority gave birth to a single baby (98%), with nearly half of respondents (48%) indicating that this was their first baby.
[Figure 1.4; Table 1.3b]
The majority of respondents to the 8-12 week survey completed the survey when their baby was between eight and twelve weeks old.
Figure 1.4: Profile of 8-12 week survey respondents (percentage of respondents, by age of baby, whether this was the respondent's first baby, and whether it was a multiple birth).
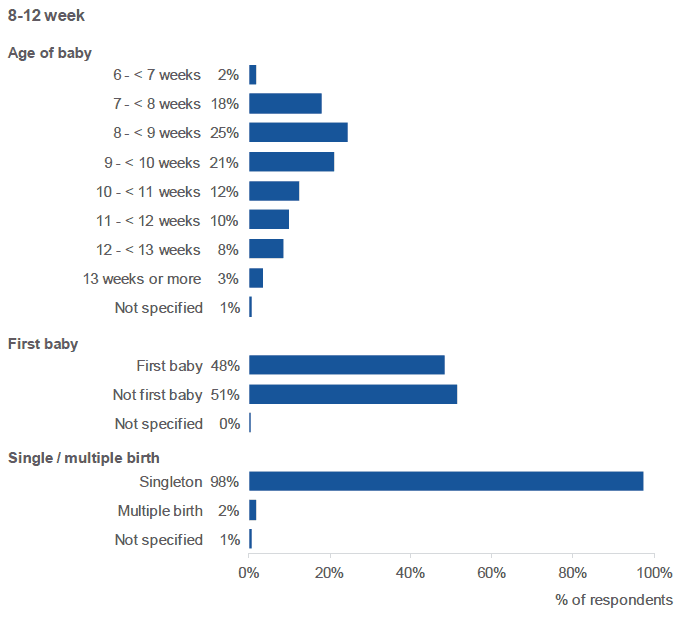
Source: Q2, Q18, Q1, 8-12 Week Survey
Respondents to the 8-12 month survey
For the 8-12 month survey, survey packs were mailed out to those being invited to participate when their infants were between seven-and-a-half and eight-and-a-half months old (spanning the eight month target age).
The majority of respondents (88%) confirmed that their infant was eight or nine months old when they completed the survey. Five percent (5%) had infants aged less than eight months; 7% had infants aged ten months or more.
The vast majority of respondents gave birth to a single baby (97%), with just over half (51%) indicating that this was their first baby.
[Figure 1.5; Table 1.3c]
The majority of respondents to the 8-12 month survey completed the survey when their baby was eight / nine months old.
Figure 1.5: Profile of 8-12 month survey respondents (percentage of respondents, by age of baby, whether this was the respondent's first baby, and whether it was a multiple birth).
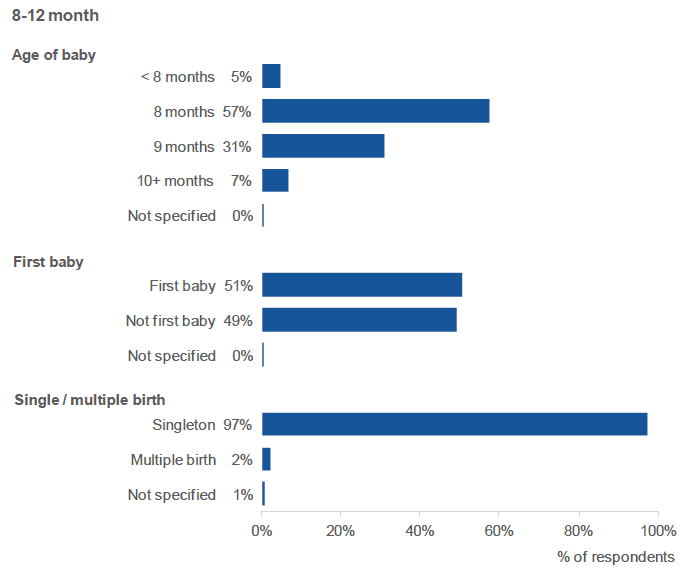
Source: Q3, Q1, Q2, 8-12 Month Survey
1.7 Interpretation of survey results
Main results and tables
- All results have been weighted by respondent age, deprivation ( SIMD quintile) and NHS board of residence to correct for differential response rates amongst different groups of women.
- For each part of the survey, weighted percentage estimates are presented in the report, showing how respondents answered each question.
- Tables showing these weighted percentages, plus weighted and unweighted counts, have been produced to accompany this report. These tables are referenced throughout the report.
- Unless otherwise stated, specific differences mentioned in the text are statistically significant at the 95% confidence level.
- Tables showing all results by respondent age, deprivation and NHS board of residence also accompany this report; these tables present the 95% confidence interval associated with each result.
- Although not referred to within the report, tables showing results by respondent ethnicity are also available. However, it should be noted that the vast majority of respondents (92 - 94%) indicated that "white" best described their ethnic group.
Rounding of results
- Where percentages do not add up to 100%, this may be due to rounding or because some respondents did not provide an answer to a question.
- Similarly, where two or more results have been aggregated, the resulting percentage may appear 1% higher / lower than expected due to rounding.
- Any results smaller than 0.5% are reported as 0%.
- For "tick all that apply" questions, where respondents could indicate more than one answer, percentages may sum to more than 100%.
Results based on small numbers of respondents
- Results based on small numbers of respondents should be treated with caution.
- Results based on responses from fewer than 50 respondents have been highlighted.
- Results based on responses from fewer than 30 respondents are not shown (except for a small number of key analyses).
Consistency of response
It should be noted that some respondents were not always consistent when responding to similar types of questions. For example, in the antenatal survey, there is more than one question about stopping / reducing alcohol intake before pregnancy and responses to these questions do not always correlate.
Comparison to the 2010 UK-wide Infant Feeding Survey
Throughout this report, several results from this survey are compared to equivalent results from the 2010 UK-wide Infant Feeding Survey ( IFS). ( R7) While many results are broadly comparable, it should be noted that the question wording and methodology used in both surveys differed. It should also be noted that the demographic profile of women giving birth in Scotland has changed since 2010 ( e.g. mothers are now generally older). Any comparisons between the two surveys have not been statistically tested and should be considered with the points noted above in mind.
Comparison to official Scottish National Statistics
To help provide context to this survey, several results are compared to figures sourced from official Scottish National Statistics publications (for example, Births in Scottish Hospitals and Scottish Infant Feeding Statistics). ( R8, R9)
It should be noted that survey results are only based on a sample of the population, whereas the official statistics referenced in this report are based on all women who gave birth in Scotland. While the survey is helpful in establishing variations between different groups of women, data presented in the official statistics for Scotland should be regarded as the definitive source.
Contact
There is a problem
Thanks for your feedback